Experts Matter. Find Yours.
Connect for media, speaking, professional opportunities & more.
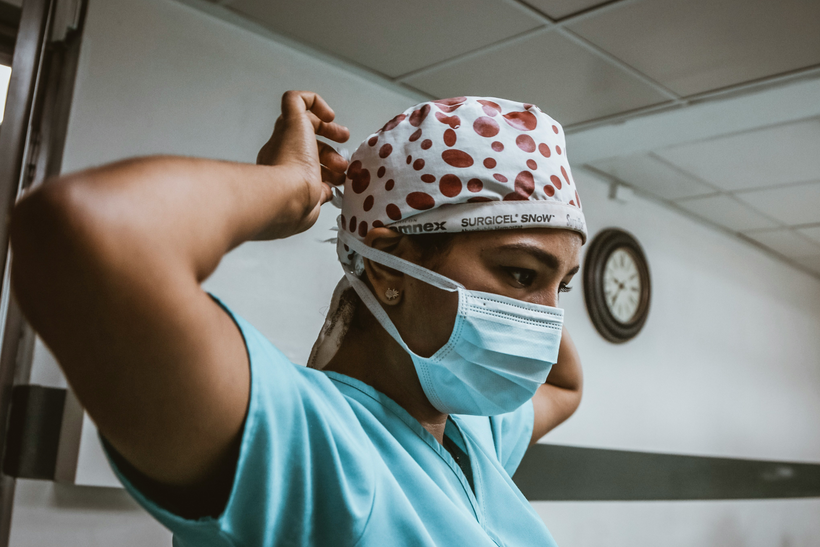
A Highly Skilled Healthcare Workforce Could Be in Jeopardy From COVID-19
While all healthcare professionals have stepped up during the COVID-19 pandemic and are essential to providing quality care, registered nurses are with patients 24/7 and provide essential, consistent surveillance, often being the first to take immediate action and alert colleagues in order to save patients. “I cannot stress enough that it is not about beds and space, it is about having a high-quality and properly educated workforce to care for the patients in those beds and spaces,” says Donna Havens, PhD, RN, FAAN, Connelly Endowed Dean and Professor of the M. Louise Fitzpatrick College of Nursing, who adds that the process depends on a highly skilled workforce. Though in some cases, because of the growing shortage across the nation during the pandemic, members of the workforce may not have the skills or experience to care for patients in the settings in which they may have been placed during the pandemic. Nurses who typically work in one particular clinical setting, e.g., pediatrics, may now be asked to provide care to adult intensive care unit (ICU) patients with very little education, if any, regarding the particulars of caring for this population. This may impact the quality of care—as well as increase distress and burnout among the workforce. The number of hospitalized patients is growing exponentially each day, and the healthcare workforce is expressing growing concern, distress, disappointment and anger about the numerous issues and challenges within the healthcare settings—as well as in regard to the general population disregarding healthcare experts’ and scientists’ guidance to adhere to practices that will mitigate the spread of the virus. Media coverage is articulating the workforce’s dismay and their calls for help—because they are tired, burned out and facing a struggle to go to work. While some traveling healthcare professionals, who practice by accepting assignments as temporary reinforcements across the country, were being sent to hot spots earlier in the pandemic, there are so many hot spots across the country today that this may no longer be a solution to ameliorate the shortage of quality care providers. Havens and colleagues at Villanova’s M. Louise Fitzpatrick College of Nursing launched a national 20-year study in May—the CHAMPS study—to explore the emotional and physical wellbeing of the healthcare workforce and those who support care. Their early findings document high levels of depression, stress and sleep issues. “Not only is the healthcare workforce growing tired, distressed and burned out, but many are also becoming ill themselves—many dying of COVID-19. This is demoralizing and severely impacts the number available to provide care. Some of the respondents from the CHAMPS study describe caring for healthcare colleagues who died from COVID while they were caring for them.” The World Health Organization designated 2020 as the Year of the Nurse and Midwife, and 2020 is also the 200th birthday of Florence Nightingale, who founded the nursing profession. “How ironic that during this time, nurses find themselves working in surge hospitals in tents, basketball arenas, parking garages and so forth, just as Nightingale’s early career was spent implementing processes to improve sanitation and hygiene,” says Havens.

Start Your Children's Day Off Right So They Can Be Productive at School
Though the 2020 school year may be very different from past years, it's still an ideal time to get kids back on track—with their activity, nutrition and overall wellness to support a productive and happy school year. Breakfast is an important meal for kids and should not be overlooked. According to the Academy of Nutrition and Dietetics, kids who eat breakfast in the morning are more alert during the school day and perform better. If you don’t have a lot of time for a sit-down breakfast, try brown-bagging it with a banana, a bag of trail mix made with whole-grain cereal, shelled pistachios and a favorite dried fruit (like diced apricot, pineapple or mango). "When it comes to school lunches, even if lunch break this year means your child is sitting at your kitchen table and not at the school cafeteria, that does not mean you can't have fun and pack a nutritious lunch," says Rebecca Shenkman, MPH, RDN, LDN, director of the MacDonald Center for Obesity Prevention and Education at Villanova's M. Louise Fitzpatrick College of Nursing. A continued favorite lunch box fad for kids is the Bento Box lunch. "These sleek lunch boxes offer an easy way to provide a visually appealing meal for kids while helping parents compartmentalize and assemble a healthy meal by placing a different food group in each section," says Shenkman, who suggests cut-up grapes, whole wheat crackers with peanut butter, cheese sticks and sliced cherry tomatoes—"anything to get kids to eat healthier and that you can keep in the fridge until they're ready to eat knowing that you provided them nutritional energy for the day."

Individuals With Intellectual and Developmental Disabilities More Likely to Contract COVID-19
Recent news coverage has indicated that individuals with intellectual and developmental disabilities (ID/DD) are more likely than those without ID/DD to contract COVID-19 and to die as a result of it. "Similar to other individuals with disability, those with ID/DD often have pre-existing health conditions that increase their risk," says Suzanne C. Smeltzer, EdD, RN, the Richard and Marianne Kreider Endowed Professor in Nursing for Vulnerable Populations at Villanova University's M. Louise Fitzpatrick College of Nursing. Some people with ID/DD live in group settings in which they come in contact with others who may be infected with COVID-19. The frequent turnover of personal assistants and contact of persons with ID/DD with multiple personal assistants may increase the risk of COVID-19 in part because of their exposure to multiple potential carriers and the need for many of their personal assistants to use public transportation. Dr. Smeltzer says, "There is also concern in the disability community, among family members of individuals with disability and among disability advocates that those with these disabilities will be viewed as less deserving of more aggressive therapies, such as ventilators. The quality of life of persons with ID/DD may be considered by others as low, even though quality of life can only be judged by the people themselves." Initial limitations put in place in many health care institutions included the exclusion of family members and other support persons because of risk for COVID-19 infection. However, a groundswell of advocacy resulted in changes in this policy because individuals with ID/DD hospitalized during the COVID-19 pandemic were being deprived of essential support. "These support persons are needed to help those with ID/DD understand what was happening in the hectic health care settings and to help with communication and decision making," says Dr. Smeltzer. "Individuals with ID/DD need the same care as others and must receive explanations about their care and must be allowed to participate in making decisions about their care."
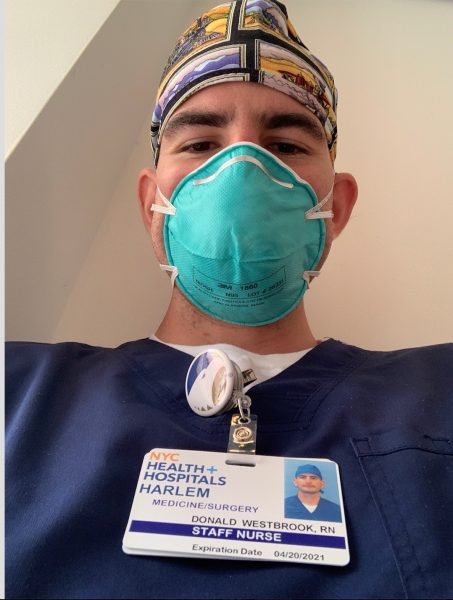
Diary of a COVID-19 crisis nurse in NYC: A Georgia Southern student’s first job
On May 1, Tucker Westbrook could finally sleep in. He’d been on duty as a COVID-19 crisis nurse at Harlem Hospital Center in New York City for 11 consecutive days, with a routine that began before the sun came up and ended long after the city had gone dark. Most mornings, he’d wake at 5:45 am., center himself with prayer and meditation, eat breakfast, and hop on a bus in time to clock in for his shift at the largest public hospital in Central Harlem by 7 a.m. Each day as he entered the halls of the facility’s surgical floor, which was transformed into a COVID-19 holding unit for the larger part of his three-week work rotation, he was unsure of what he’d encounter. Just weeks earlier, Westbrook, a May 2019 Georgia Southern University nursing graduate from Butler, Georgia, accepted a short-term contract to assist with the Coronavirus pandemic in the epicenter of the U.S. outbreak. This was Westbrook’s first professional job, following what was supposed to be a yearlong mission trip in Southeast Asia, but was cut short due to the pandemic, and nothing could fully prepare him for the impact of his initial experience. “The first day, I thought, ‘I’m not prepared for this,’” he admitted. “Those first few days I was on pins and needles and thought, ‘how am I going to mess up?’” The stakes were high. By the time he arrived in New York City, thousands had already been hospitalized, and many had died. Seasoned nurses and doctors were depleted and morale was low across the city, he explained on the phone as he looked out over a desolate Times Square from his hotel window. “They asked me, ‘why did you come here?’” Westbrook recalled. “And I said that I wanted to be, hopefully, a light in this dark place right now. The patients, the doctors, the nurses, the nursing assistants, the janitorial assistants — my goal is to learn everyone’s names and greet them with a smile behind my mask.” A friend encouraged Westbrook to look for a temporary nursing job upon his return from abroad. When he applied for highly competitive positions with a crisis staffing agency, he requested placement in an area hard hit by the pandemic. “Just like Southeast Asia, I wanted to go where there was the biggest need, and I had enough gifts to meet that need,” Westbrook said. This was Westbrook’s first trip to New York, and he stepped into a scene where images of makeshift morgues and ventilator shortages splashed across the media came to life in front of him. “It has been surreal to see,” he said. Assigned to provide cluster care to potential COVID-19-positive patients for minimal exposure, Westbrook also focused on simple acts of kindness to help ease increased anxiety among the patients. “That might be things as small as giving a wet rag to wipe their face,” Westbrook said. “It may be filling their jars with ice cold water in the morning. Whatever might help them feel more comfortable.” Westbrook’s patients were diverse: a teenage gunshot victim who sobbed at the prospect of being infected with the virus; an adult male who discussed intimate thoughts about death with his family over the phone; and a woman who was depressed until Westbrook sat with her so she didn’t feel alone. Experiencing humanity in its most delicate form was life-defining. “I was learning more about nursing care but also continuing to serve (my patients) beyond simply giving them medicine,” Westbrook said. “I was able to advocate for them with the doctor, especially without their families there. I’m learning how to go above and beyond, and what our job responsibilities are. I want to keep growing and learning to continue to give care to my patients.” The hospital staff also offered enormous support and guidance to Westbrook, who almost two weeks into the job felt exponentially more confident in his abilities. “If you had told me about any of this I wouldn’t believe it,” he said. “It has been incredible. I did not think I could do that at all, and here I am on the other side. This was such a lofty and high goal to complete this and do well. I’m thankful to even be here and have this opportunity.” Westbrook credits his father for encouraging him to study nursing, and Georgia Southern faculty for their expert instruction, which he put to use in New York, as well as their sage advice. “I wasn’t sure I was going to get my license,” he said. “My desire to become a doctor or a missionary became more and more compelling, but my professors assured me that it would be worthwhile to pursue my license, and they were right.” Following a quarantine in his family’s home, Westbrook will begin pre-medicine classes at Georgia Southern this summer. If you are a journalist looking to know more about Tucker’s story or the nursing program at Georgia Southern University – let us help with your coverage. Barry Joyner is the dean of Georgia Southern University’s Waters College of Health Professions - simply click on his icon to arrange an interview today.

Myth-breaking and COVID-19 (Coronavirus) – Manhattanville Expert Answers Your Questions
Information, news stories, articles and advice are coming at Americans from all sides these days when it comes to COVID-19, its spread, prevention, those vulnerable, and whether America should continue to shut down or carry on carefully. There’s a lot to know and it is vitally important that accurate, credible and reliable information is what’s being shared. That’s where the experts from Manhattanville College can help. Orhan Hakli, RN, MS-FNP-C, is an administrator in the School of Nursing and Health Sciences at Manhattanville College. He is a certified Family Nurse Practitioner in private practice who has worked in various areas of health care including medical-surgical nursing, cardiology, geriatrics, wound care, hyperbaric medicine, and primary care. Here are a few of the questions he has been facing in recent days from patients. Below, he breaks down some of the myths that are surfacing with facts. I heard drinking alcohol- especially Vodka- decreases my risk of getting COVID-19. MYTH- There is no credible evidence to support that alcohol consumption decreases the risk of COVID-19. Using hand sanitizers that contain at least 60% alcohol to clean your hands can be helpful. So, using hand sanitizers with 60% alcohol yes, drinking to prevent COVID-19 is a hard no. I heard coronavirus comes from animals. I have a dog at home. Should I get rid of him/her? MYTH- It is true that Coronavirus is common in animals but not in household pets, so cuddle away but wash your hands afterwards for personal hygiene purposes. If I go out, I will get sick MYTH- We recommend social distance, not social isolation. As long as you keep 6 feet from people, do not touch your mouth, nose, or eyes and wash your hands frequently, you should be fine. If I was in contact with someone who had the coronavirus, I should start taking antibiotics immediately. MYTH- This is a viral disease; antibiotics have no effects on viral diseases. They are effective only on bacterial infections. Getting products in the mail from China will make people sick. MYTH- The Centers for Disease Control and Prevention (CDC) tells us that Coronavirus, like many other viruses, do not stay alive for very long especially on the product surfaces that are in transit for days. There are two major ways that the virus can spread. Either people who are in close contact (within about 6 feet) through respiratory droplets produced when an infected person coughs or sneezes (which is the main way) or touching a surface or object that is contaminated with the virus then touching your mouth, nose, or eyes. The second way is not thought to be the main way the virus spreads. Coronavirus can live up to two days on surfaces but loses its effect as time passes. Takeaway point - keep your 6-foot distance from people and do not touch your mouth, nose, or eyes after touching objects. I heard African-American people cannot get coronavirus. MYTH- The CDC clearly indicates that this is a virus that affects the respiratory system regardless of race. Everyone is at equal risk of getting COVID-19. If I have Coronavirus I will likely end up in the ICU and die. MYTH- The World Health Organization (WHO) indicates that most people- in fact up to 80%- will recover on their own having mild to no symptoms at all. How the disease will affect you depends on age and other comorbidities you may have. Orhan Hakli is available to speak with media about the virus as a contagious disease, prevention, myths, strains on the health care system and public health measures. He has recently been advising the food service industry on measures they can take to prevent the spread of Coronavirus. To book an interview – simply click on his icon to arrange a time.

Baylor Gerontology Expert Shares Tips to Care for Aging Population During Coronavirus Pandemic
“This is not a vacation from caring; it is a time when caring is needed most of all,” social work professor says The Center for Disease Control and Prevention (CDC) has announced that older adults and people who have serious chronic medical conditions such as heart disease, diabetes and lung disease are at a high risk for the coronavirus. The virus hit hard in late January at a nursing facility in the state of Washington, where a number of residents died. As a result, the CDC has recommended strong restrictions on visitors to long-term care facilities, and the health organization continues to preach limited physical contact and “social distancing” – creating intentional space of six feet or more between each person – to stem the spread of the virus. James Ellor, Ph.D., The Dorothy Barfield Kronzer Endowed Professor in Baylor University’s Diana R. Garland School of Social Work, is an expert on working with older adults as well as disaster behavioral health. He said it’s important in this time of uncertainty to continue to support and minister to those older adults who are self-isolating in their homes and those in long-term care facilities. “Remember, no one stops caring about others just because germs are in the way,” Ellor said. “Express your caring in appropriate ways. This is not a vacation from caring; it is a time when caring is needed most of all. We also know that prayer is very important. Hold the person in prayer and let them know you are doing so.” In the following Q&A, Ellor shares tips on how to care for this population during this time. Q: What are some ways we can check on older relatives and neighbors without using physical touch and interaction? A: There is a fine line in this unknown time between caution and paranoia. Respect for each other’s boundaries is the critical value. It seems very awkward to want to affirm someone, yet not shake their hand. However, we need to use our words and ask what the other person is comfortable with, and by the same measure, let them know what you are comfortable with. At this point, the most obvious ways to check on people is through social media or paper and pencil. Drop them a note, call them on a phone, use other social media devices as appropriate. I would suggest that if you normally visit them, say on Fridays, be sure to continue to do that, albeit by phone or even just drop them a card. Q: If people have chosen to self-isolate or if they’re scared to venture out due to this health crisis, what are some ways people can help? A: Be consistent. If you have a pattern, continue the pattern. Remember the principles above. If the person is feeling out of control, talk quietly with them and offer them a card or other gesture of caring. Q: Can you explain the importance of personal interaction for people who are shut in? A: People with human contact simply live longer than those completely cut off from the world, with few exceptions. While about 15 percent of older adults are “shut in,” only about 5 percent are bed bound. That means that persons who are dependent on oxygen, for example, will be in their house, but not in bed. They depend on all of their outside contacts. Keep your normal visiting pattern, albeit with a card in the mail or phone call. If you are a member of a church, have the youth group use some of their extra “stay at home” time to make greeting cards intended to cheer up a person in your church or group that is home bound. Older adults like tactile things, particularly if they are sensory-impaired. If you make a card, put a feather in it, or some other feel-good item. If you are purchasing a card, there are some that have things in them that you can feel, or even hear. Some cards will allow you to record a short message. Q: Since so many long-term care facilities now have strict rules about visitors, are there any ways that people can interact or show support to residents in a safe manner? A: Most facilities are cutting off all contact from the outside. Only their own staff, physicians and hospice nurses are being allowed in. Even social workers, chaplains and other clergy are being kept out. In the Waco area, physicians are being screened for a fever or cough and could be turned away. As such, phone calls, cards and letters are all important. Several facilities in this area have begun to put room numbers on the windows of their facility, so that family can come by and wave through the window. Persons in long-term care facilities, even those with dementia, will pick up on the anxiety of the staff and especially the TV, which is often on all the time. A person with dementia may not be able to understand the anxiety but will be anxious when others are anxious. This makes the job of staff that much harder. Q: Anything else you’d like to share? A: The workers at these homes have a much harder job now. Don’t hesitate to send them a card or a treat if it can be obtained safely. Staff, even the people at the door telling you that you can’t come in to see your loved one, have a tough job now and need extra support from everyone. ABOUT JAMES ELLOR, PH.D. James Ellor, Ph.D., serves as professor and The Dorothy Barfield Kronzer Endowed Professor in Family Studies in Baylor University’s Diana R. Garland School of Social Work. works with older adults around issues of mental and spiritual health. He has served on the executive committee of the Midwestern Geriatric Education Center and provided education, counseling, and planning for individuals and groups who work with seniors. His research includes work in entrostomal therapy, hunger, the church as service provider, spiritual assessment, and intervention techniques with cognitively impaired older adults. ABOUT BAYLOR UNIVERSITY Baylor University is a private Christian University and a nationally ranked research institution. The University provides a vibrant campus community for more than 18,000 students by blending interdisciplinary research with an international reputation for educational excellence and a faculty commitment to teaching and scholarship. Chartered in 1845 by the Republic of Texas through the efforts of Baptist pioneers, Baylor is the oldest continually operating University in Texas. Located in Waco, Baylor welcomes students from all 50 states and more than 90 countries to study a broad range of degrees among its 12 nationally recognized academic divisions. ABOUT THE DIANA R. GARLAND SCHOOL OF SOCIAL WORK AT BAYLOR UNIVERSITY Baylor University’s Diana R. Garland School of Social Work is home to one of the leading graduate social work programs in the nation with a research agenda focused on the integration of faith and practice. Upholding its mission of preparing social workers in a Christian context for worldwide service and leadership, the School offers a baccalaureate degree (B.S.W.); a Master of Social Work (M.S.W.) degree available on the Waco or Houston campuses or online; three joint-degree options, M.S.W./M.B.A., M.S.W./M.Div. and M.S.W./M.T.S., through a partnership with Baylor’s Hankamer School of Business and George W. Truett Theological Seminary; and an online Ph.D. program. Visit www.baylor.edu/social_work to learn more.

It’s here and it’s time America got serious about Covid-19, known as coronavirus. The CDC is working overtime, and leading government health officials are scrambling to ensure hospitals are equipped, front-line health providers are ready and the public is informed. But with any emergency, there comes the risk of misinformation and unnecessary worry. As the new coronavirus outbreak becomes an ever-looming threat in the United States, state infectious disease specialists say the first step to staying safe is this: Remain calm. Also, don’t worry about buying a mask. “You really have to make sure you get the accurate information and not … ‘Lock your doors, close the windows, buy a generator and hope for the best,’” said Dr. Peter Gulick, an infectious disease expert at the Michigan State University's College of Osteopathic Medicine and director of the MSU Internal Medicine Osteopathic Residency program. That’s not only alarmist and bad advice, he said, it’s a waste of energy. The best advice — like these tips from the U.S. Centers for Disease Control and Prevention — is tried-and-true, Gulick said: Wash hands often with soap and water for at least 20 seconds. It’s especially important after using the bathroom, before eating, and after blowing your nose, coughing or sneezing. No soap and water? Use an alcohol-based hand sanitizer with at least 60 percent alcohol. Avoid touching your eyes, nose and mouth with unwashed hands. Avoid close contact with people who are sick. If you’re sick, stay home. Cover your cough or sneeze with a tissue, then throw the tissue in the trash. Clean and disinfect frequently touched objects and surfaces using a regular household cleaning spray or wipe. If you think you’ve come in contact with someone with the virus (there have been no confirmed cases yet in Michigan) contact your health provider immediately. February 26 – The Bridge Regrettably, that too can often lead to financial reactions that can ripple across the economy. Lately, the surging stock market has plunged with worries from investors and Wall Street about how America’s workforce will be impacted if the virus spreads. Friday ended the worst week the stock market has had since 2008. NBC News 6 sat down with the Dean of the Broad College of Business at Michigan State University, Sanjay Gupta, to talk more about the stocks and what to expect after this week. “The stock market is clearly spooked, and it has become nervous with whatever is going on in the business world,” said Gupta. What has ‘spooked’ the business world, is COVID-19. “The coronavirus is quarantined lots of factories, in fact the whole country,” said Gutpa. Gutpa says the halt in Chinese manufacturing also limits businesses and goods here in the United States. “In our day to day lives, either there will be some things that we count on that may not be available. It might be that the priciest of those things that we count on change, or go up dramatically because we are so dependent on a foreign source,” said Gutpa. February 29 – WLNS TV Covering an outbreak like Covid-19 isn’t easy, there are multiple angles to explore and it is vital that only the correct facts are shared by media to the millions of viewers, readers and listeners that are waiting for the latest information – and that’s where our experts can help. Sanjay Gupta is the Eli and Edythe L. Broad Dean of the Eli Broad College of Business. He is an expert in the areas of corporate and individual tax policy issues and finance. Peter Gulick is currently an associate professor of medicine at Michigan State University, College of Osteopathic Medicine, and serves as adjunct faculty in the College of Human Medicine and the College of Nursing. Both experts have already been sought out by the media for their expert insight on this issue – if you are interested in arranging an interview, simply click on either expert’s profile to arrange a time today.

School Nurses Positioned to Help Solve School Shooting Epidemic
Since 2018 school nurses have responded to 38 school shootings, and they find themselves on the front line of gun violence, whether the act is by an active shooter in a school, a mass shooting in the community or anywhere in the country. "The epidemic of gun violence is a public health crisis affecting the whole country, but school nurses are ideally positioned to work alongside others who are committed to public health approaches to solve the issue of mass shootings," says Sunny G. Hallowell, PhD, assistant professor at Villanova University's M. Louise Fitzpatrick College of Nursing. Every school day, 95,000 school nurses enter U.S. schools prepared and ready to serve more than 55 million children for six and a half hours, 180 days a year. Families, school districts and communities entrust their children to school environments with the expectation that they will be kept safe from harm. School nurses are first responders whose skills are crucial to ensuring the health and safety of students, staff and faculty within schools and the surrounding community. Hallowell is coauthor of "School Nurses Share their Voices, Trauma and Solutions by Sounding the Alarm on Gun Violence," published recently in the medical journal Current Trauma Reports. She and her coauthors shed light on the impact of gun violence within schools from the perspective of school nurses, whose expertise is critical to the design and implementation of programs that keep students safe. "Nurses are trained both in the emergency trauma care and clinical responses necessary for addressing traumatic gun violence, as well as the mental health outcomes resulting from tragedy," says Hallowell. "There is a critical need for research that guides the selection of evidence-based safety programs that consider the developmental and the mental health needs of school communities." Standard response protocols such as school safety drills, fire drills and tornado, hurricane and earthquake drills have been implemented as early as the First World War. The memory of air raid drills and the lingering effect of the experiences have been well documented. As Hallowell's journal article shows, fear has long dictated how schools invest their resources in response to gun violence.

Climate Change: A Direct Threat to Older Adults
Climate change will impact the health of all populations, but older adults are uniquely vulnerable because of the physiological changes of aging. More than half of older adults in the United States live in areas that disproportionately experience the effects of heat waves, forest fires, hurricanes and coastal flooding. Pennsylvania, New York, California, Florida and Texas account for the top five states where older adults are concentrated. Older adults who live in urban areas are vulnerable to heat island effect—the concentration and retention of heat in urban areas compared to rural areas—which places older residents in cities at increased risk of heat related illnesses and death. “Gerontological nurses need to be prepared to address the specific issues of older adults,” says Ruth McDermott-Levy, PhD, director of the Center for Global Health at Villanova University’s M. Louise Fitzpatrick College of Nursing. “We want to help nurses understand climate change and the need for specific interventions to support climate adaptation for the older adult population.” Climate change impacts require modifications in health plans for older adults. Prolonged heat will require greater needs for hydration, but the patient’s other conditions need to be considered as well. Elders with heart disease and renal failure will require astute nursing assessments to monitor the balance of hydration and electrolytes while not leading to fluid overload or electrolyte imbalances in the presence of extreme heat. With their research, practice and influence over policy, gerontological nurses are in an important position to be changemakers by measuring and documenting the harm and impact of climate change on older adults. They can advocate for measures that support older adults in disasters or extreme weather events. Nurse researchers can collaborate with climate scientists and policy makers to develop initiatives and programs that rely on climate and health evidence to support climate mitigation and adaptation for the older adult. “It is everyone’s responsibility to learn about climate change and to participate in slowing the trajectory of climate change,” Dr. McDermott-Levy says.

Making Children's Mental Health and School Safety a Priority
The U.S. Department of Education announced $71.6 million in grant awards to enhance safety in schools and improve student access to mental health resources. The grants will allow local leaders to tailor their approach to school safety and mental health in ways that meet their students' individual needs and their particular school's unique challenges. "This is a strong step towards helping children across the U.S. who have experienced traumatic events. We know from previous research that traumatic experiences, even those in early childhood, affect an individual at any time in their life," says Elizabeth Dowdell, PhD, RN, FAAN, professor at Villanova's M. Louise Fitzpatrick College of Nursing. "In healthcare, assessing, identifying and treating trauma has become a major public health challenge since trauma exposures frequently go unrecognized and unaddressed." The same is true in the educational system. For many children, adolescents, and adults, trauma results from an event, series of events or set of circumstances which are perceived or experienced to be physically or emotionally harmful or life-threatening. The landmark Adverse Childhood Experience study (1998) found that, in a population of 17,377 adult participants, 63% experienced at least one trauma exposure as a child and 20% experienced more than three trauma exposures. The experience of repeated trauma is sometimes referred to as toxic stress, which can have damaging effects on learning, behavior and health across the life span. These exposures included physical and sexual abuse, neglect and household dysfunction. Increased stress from family violence and chaos is trauma and, when combined with injury, is the leading preventable cause of morbidity and mortality. The lasting adverse effects from the trauma can affect a child's functioning and well-being, specifically mental and physical health, social, emotional and spiritual well-being as they age and develop. "Healthcare is shifting to a trauma-informed framework that focuses on what happened to the person rather than what is wrong with them and recognizes that individual's strengths and resilience. Schools are ideal locations for identification of traumatized children and the implementation of services to help them," says Dr. Dowdell. "School districts have to create physical safety and psychological safe places where all children can learn."





