Experts Matter. Find Yours.
Connect for media, speaking, professional opportunities & more.

New System of Infrared Sensors Maintains Privacy While Keeping Patients Safe
Short of cameras, there are few tools at the disposal of health care providers or loved ones to remotely monitor patient safety within hospitals and assisted living care facilities. This challenge was on Bob Karlicek's mind when he and a team of other researchers developed a new system of infrared sensors that is able to provide real-time data about a person’s movements in a room while also maintaining their privacy. “We can thread this balance of information and privacy,” said Karlicek, the director of the Center for Lighting Enabled Systems & Applications (LESA). “It turns out that lighting and light field sensing give us a tremendously powerful tool for figuring out where people are and estimating what they are doing, but without creating an image of who they are.” The system relies on what Karlicek calls occupant-centric control. More specifically, a set of sensors uses infrared light to measure distances between sensors and objects in order to identify where someone may be in a room. This information can help determine if a person is standing, sitting, or lying down on the floor. It can also distinguish between where people are standing and how they are interacting with other people. Such measurements could alert a caregiver that someone has fallen or document the last time someone checked on their loved one. The use of infrared light to measure distance is not a new concept. What’s novel about this approach, Karlicek said, is the development of a very inexpensive sensor that has data analytics built right into it, allowing the sensors to collect data, process it, and communicate with each other in order to track movement within a room. Karlicek is available to discuss this technology and other efforts LESA is working on to make buildings more capable, efficient, and helpful to the people who use them.

Overshadowed by COVID – The opioid pandemic is still taking its toll across America
For more than two decades opioids have been ravaging American cities, towns, and communities. It prompted national attentions and official commissions advising the President. But lately, as the world has turned almost all its focus on COVID-19, the opioid issue has been sitting in the shadows. Not necessarily idle or waiting, but just no longer the topic of a national conversation to find a cure. Before COVID-19 turned our nation upside-down, policymakers were taking steps to help patients access evidence-based treatment for opioid use disorder. This included focusing on removing health insurers’ barriers to medication and requiring insurers to provide parity for mental illness and substance use disorders — and holding them accountable for violations of the law in Massachusetts, Pennsylvania and New Hampshire, to name a few recent examples. While we continue to take steps to address COVID-19 to help keep the public safe, the American Medical Association has seen reports from more than 30 states concerning increases in opioid-related mortality, mental health crises, suicide and addiction-related relapse. Reports are from every region in the nation. This includes a 20 percent increase in calls to the Jacksonville, Fla., fire department concerning overdoses; an “unusual spike” in overdoses in DuPage County, Ill.; increased emergency department visits in coastal North Carolina and spikes in fentanyl-related overdoses in Seattle. Georgia, too, has not been spared, causing increased concern for many. - Dr. Patrice A. Harris is the immediate past president of the American Medical Association and chair of the AMA Opioid Task Force. So – at what cost or how far back have efforts been set by COVID-19? And how much harder will it be for America to regroup and take on its addiction to opioids? There are a lot of questions to be asked – and if you are a journalist covering this topic or looking to learn more about the state of the opioid epidemic in America – then let our experts help. Justin Cole is an expert in clinical pharmacy, Pharmacogenomics, and the pharmacy industry. Justin has been following this issue closely and is available to speak with media. Simply click on his icon to arrange an interview today.
Virtual Reality-Based Surgical Simulations Could Make Patients Safer
Suvranu De, the director of the Center for Modeling, Simulation, and Imaging in Medicine at Rensselaer, has dedicated more than a decade of research to making surgery safer by developing virtual reality-based surgical training simulations that closely mimic the optics and haptics a surgeon may encounter in the operating room. A new $2.3 million grant from the National Institute of Biomedical Imaging and Bioengineering of the National Institutes of Health will further his research in this space, by supporting the development of a collaborative virtual reality-based surgical simulation environment that allows medical professionals to practice technical, cognitive, and interpersonal skills as a team. “People will be wearing head-mounted displays, and they will be immersed in a virtual operating room working on a virtual patient as a team,” De said. “We want to have an expert team in the operating room focused on the treatment of a patient, and not just a team of experts.” Conceptually, this approach is similar to crew resource management practiced by aviation pilots, which has led to a significant reduction in aircraft accidents. The Virtual Operating Room Team Experience (VORTeX) simulation system will provide realistic distractions, interruptions, and other stressors that medical professionals may encounter in an operating room. Traditionally, this type of simulation training has required mannequins, instructors, and a dedicated space, as well as significant coordination and resources. In contrast, the VORTeX system will be both distributed and asynchronous – allowing participants to join the simulation from different locations, and instructors to review the simulation and provide feedback at their convenience. Machine learning algorithms will be used to crunch the data and provide feedback to participants, who will be able to return to the virtual environment to review their performance. De is available to discuss how this type of virtual training is developed and implemented.

STORY: All CAA Stores in South Central Ontario are now open
We are excited to announce that all CAA Stores will be re-opening on Friday, June 26, with proper safety, cleaning and physical distance measures in place. This decision was made with careful consideration as we reviewed the status of reopening in the province and the health and safety of our associates and members. The safety of our members, customers and associates remains our top priority. We have put in place some changes to the store operations to ensure everyone's safety while still offering the exceptional retail experience our members expect. They include: Installation of plexiglass screens at counters and desks Providing personal protective equipment for associates and members Limiting the number of members allowed in the store at one time Signage and floor decals to encourage physical distancing Sanitizing stations for members Changes to store hours The COVID-19 pandemic is an evolving situation and we will continue to monitor as needed to maintain the health and safety of our members and associates.
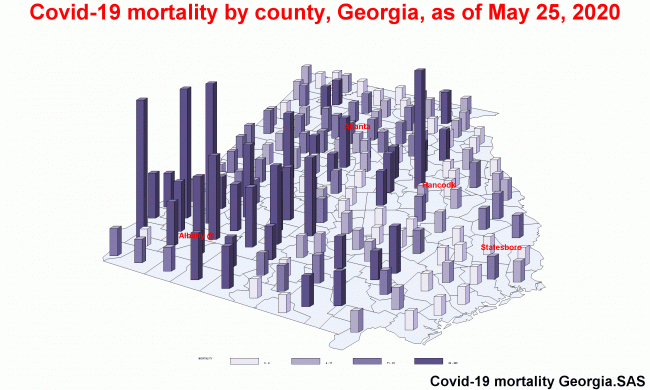
Graduate students in the Jiann-Ping Hsu College of Public Health at Georgia Southern University analyzed mortality data to reveal that a county in southwest Georgia is dealing with deaths from COVID-19 at a rate higher than most other counties in the country. The students found that the mortality rate of 305 per 100,000 residents (as of May 28, 2020) for Terrell County in southwestern Georgia, is 50% higher than that of New York state’s Nassau County, the documented highest rate in New York. The three other Georgia counties that are highest in terms of mortality rate are Hancock, Early and Dougherty counties. Three out of these four are in southwest Georgia, around the Albany area. That accounts for almost half of the 10 counties in the United States with the highest mortality rate, which is defined as a measure of the frequency of occurrence of death among a defined population. However, it’s interesting to note that none of Georgia counties reached the top 20 in terms of incidence and the death numbers per 100 confirmed Covid-19 cases, said professor Dr. Jian Zhang, a veteran medical epidemiologist. “Georgia is doing pretty well to stop the spread of the virus, and hospitals in Georgia are doing well to save hospitalized COVID-19 patients. The high mortality rate, in this case, may be deeply rooted in the historical burden of poverty in Georgia,” Zhang said. The findings are part of a service-learning project Zhang led. A six-student group formed the surveillance team that began running a real-time COVID-19 numbers in his Public Health Surveillance class. If you are a journalist covering COVID-19 and would like to learn more about this research taking place at Georgia Southern University – then let us help. Dr. Jian Zhang has worked with the Chinese Centers for Disease Control and Prevention, and the World Health Organization prior to moving to the United States.

Individuals With Intellectual and Developmental Disabilities More Likely to Contract COVID-19
Recent news coverage has indicated that individuals with intellectual and developmental disabilities (ID/DD) are more likely than those without ID/DD to contract COVID-19 and to die as a result of it. "Similar to other individuals with disability, those with ID/DD often have pre-existing health conditions that increase their risk," says Suzanne C. Smeltzer, EdD, RN, the Richard and Marianne Kreider Endowed Professor in Nursing for Vulnerable Populations at Villanova University's M. Louise Fitzpatrick College of Nursing. Some people with ID/DD live in group settings in which they come in contact with others who may be infected with COVID-19. The frequent turnover of personal assistants and contact of persons with ID/DD with multiple personal assistants may increase the risk of COVID-19 in part because of their exposure to multiple potential carriers and the need for many of their personal assistants to use public transportation. Dr. Smeltzer says, "There is also concern in the disability community, among family members of individuals with disability and among disability advocates that those with these disabilities will be viewed as less deserving of more aggressive therapies, such as ventilators. The quality of life of persons with ID/DD may be considered by others as low, even though quality of life can only be judged by the people themselves." Initial limitations put in place in many health care institutions included the exclusion of family members and other support persons because of risk for COVID-19 infection. However, a groundswell of advocacy resulted in changes in this policy because individuals with ID/DD hospitalized during the COVID-19 pandemic were being deprived of essential support. "These support persons are needed to help those with ID/DD understand what was happening in the hectic health care settings and to help with communication and decision making," says Dr. Smeltzer. "Individuals with ID/DD need the same care as others and must receive explanations about their care and must be allowed to participate in making decisions about their care."

MEDIA RELEASE: Watch for Bikes: Top nine tips for cycling safety success
The summer months are fast approaching and with more cyclists and drivers expected to re-emerge on the roads, CAA South Central Ontario (SCO) is encouraging motorists to keep the safety of cyclists in mind when sharing the road. “Cycling is an excellent way to stay active during the pandemic and many more are picking up the activity, but as the province works towards reopening, we need to stay vigilant for everyone’s safety,” says Teresa Di Felice, AVP of government and community relations at CAA SCO. All drivers and cyclists are advised to follow public health guidelines, be predictable, be patient, communicate their intentions with signals, regularly check blind spots, and turn on their lights during dawn, dark and dusk. “In Ontario, there are tough penalties for those who do not follow the rules of the road, yet many remain unaware of what these rules are. Whether you’re on two wheels or four, get to know the following rules and best practices,”adds Di Felice. CAA is also reminding all motorists of these important rules of the road: Be aware. Do not use headphones or mobile devices while driving and pay attention. Yield to cyclists. Motorists should not be driving in a bike lane unless making a right turn. Watch for the approaching cyclists and never speed up and cut off a cyclist when making a right turn Keep a safe distance. Drivers must keep at least a one metre distance from other cyclists. If it is not possible, safely change lanes to pass. The penalty for not doing so is a $110 fine. Practice the Dutch Reach. Avoid “dooring” cyclists by doing the Dutch Reach. CAA launched a new Dutch Reach video for users to practice as more people out on their bikes. Some cycling-specific safety tips: Ride with traffic. Riding against traffic flow is dangerous, illegal and a leading cause of car-bike collisions. Protect yourself. Drivers, use your seat belts. Cyclists, wear your helmets. Be visible. Use reflectors and lights in dark and overcast conditions. It’s the law. Be predictable. Obey traffic signs and be clear with your intentions with other drivers. Under Ontario’s Highway Traffice Act (HTA), a bicycle is considered a vehicle, just like car or truck and must follow the same rules of the road. Ride close to home. As cyclists start to use their bikes for the first time in awhile, remember to stay close to home as you are starting out. Put your cycling safety knowledge to the test with CAA’s new cycling safety quiz. For all other cycling information, visit caasco.com/cycling. If you run into a problem that cannot be fixed on the spot, CAA Bike Assist will transport you and your bicycle to wherever you need to go. It's available as part of your membership 24 hours a day, 7 days a week, 365 days a year.
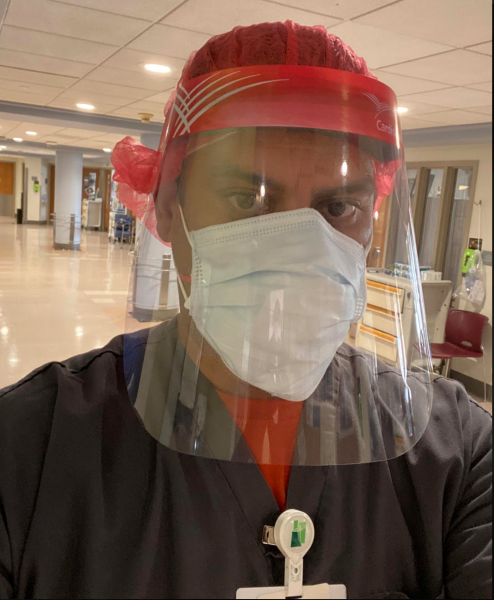
When the first cases of the novel coronavirus arrived in Chatham County, Georgia, Rafael Agosto, who has been a respiratory therapist at St. Joseph’s/Candler Hospital in Savannah for 17 years, had to recalibrate his approach to lung care. “Initially, it was kind of wild because we didn’t know what to expect and how to manage any of these patients,” said Agosto. “What are we looking for, and how do we treat this?” The primary role of a respiratory therapist is to assist patients who have trouble breathing by administering oxygen, managing ventilators and measuring lung function, among other methods. COVID-19 symptoms include fatigue, fever, cough and shortness of breath, and at the onset, Agosto and his colleagues raced to stabilize patients who tested positive for the precarious disease. “We were trying to keep them oxygenated,” he said. “It was sort of like pneumonia, but we wouldn’t treat it like a normal pneumonia because it’s like a deadly pneumonia. Patients were declining very fast so you didn’t have time like you normally would with other patients. And they were of all ages. That’s what was so scary.” While grappling with patient care, Agosto and his co-workers were also dealing with fear for their own safety with exposure to the virus in such close proximity. St. Joseph’s/Candler, Agosto’s employer since he graduated with a B.S. in respiratory care from Georgia Southern University’s Armstrong Campus in 2003, made it a priority to outfit the health care workers with proper personal protection equipment (PPE), Agosto said. “That was scary but they made sure we had what we needed,” he explained. “Safety was the number one key. So the proper PPE, it was everything. We had all of it. A face shield, goggles, scrub cap and masks. They were not comfortable at all. At least here when I wore them I had downtime, but in Boston, holy moly, my face was bruised.” Agosto registered for a four-week rotation with a crisis nurse staffing company that placed him at Good Samaritan Medical Center in Brockton, Massachusetts, a suburb of Boston. COVID-19-related deaths in Massachusetts were outpaced only by New York and California, and Brockton was the second hardest-hit community in the state. “The reason I went was the opportunity to help patients, number one, and to learn how they were managing their ventilator patients there so it could help here,” he explained. On April 19, Agosto reported to the facility, suited up for his first 12-hour shift. “I was in complete shock when I got in there,” Agosto said. “The ICU was full. Every single floor was possible for COVID.” The hospital averaged 80 to 90 cases throughout his stay, and the intensive care unit remained full. Days were hectic and taxing; lunch was an afterthought. His focus was on keeping patients off of ventilators, as global reports show that more than half of ventilated coronavirus patients don’t survive. Yet, “it started becoming hard to get them off ventilators,” and his group often didn’t have a choice but to put patients on 100% oxygen. Stress didn’t let up, but Agosto found moments of solace in interactions with patients. “I would walk into patients’ rooms and they all kept telling me the same thing — they’re scared,” he said. “Because they don’t know anything. It’s like a ghost town because the nurses are running around. Patients felt they weren’t being seen much.” In response, Agosto offered his undivided attention. “That’s one thing that made me feel really good,” Agosto continued. “Just to sit there and talk with them for a few minutes. Or just listening to them. That’s what we’re here for, and they were appreciative.” Agosto returned to Savannah healthy and with a new oxygen delivery device to share with his co-workers at St. Joseph’s/Candler. His manager ordered the devices to serve local patients. “The most important thing I took out of this is that it’s serious, and people are doing everything they can,” Agosto said. “They’re putting their lives in jeopardy for the patients, and I’m glad I had the opportunity to do that.” The accomplishment of his goals in a time of crisis and his continued dedication as a respiratory therapist leave Agosto fulfilled. “I didn’t get sick,” he said. “I helped as much as I possibly could. I did what I wanted to achieve. I’m so happy and blessed because I still love my job.” If you’re a journalist covering COVID-19 and how Georgia Southern University is helping mitigate the spread of this virus – then let us help. Barry Joyner, Ph.D., is the dean of Georgia Southern University’s Waters College of Health Professions - simply click on his icon to arrange an interview today.

STORY: CAA Volunteers to deliver another BIG shipment of PPE to help Frontline workers.
CAA has once again partnered up with Mobilizing Masks for Health Care workers to deliver a large donation of 120,000 Personal Protective Equipment masks. Mobilizing Masks is a grassroots organization of physicians and advocates, that is facilitating a large-scale mask donation drive, to bring masks to hospitals most in need of PPE and to units where medical staff have high exposure to COVID-19 positive patients. While CAA has been helping the organization with the delivery of PPE’s since April 6th, this donation is one of the largest to date. The masks were donated by T & T Supermarket and delivered by CAA to 105 Gibson, a community centre in Markham. There they were sorted and distributed to long term care residences in the GTA. Since April 6th CAA South Central Ontario has helped to distribute: Surgical Masks - 570,805 N95 masks - 3,810 Face Shields - 2,900 Thank you to all the Associates and Network Providers who have contributed to getting this initiative off the ground and who continue to ensure that those on the frontline of our healthcare network are supported.

Twelve students in the Doctor of Physical Therapy (DPT) program at Georgia Southern University were awarded scholarships totaling more than $17,000 from the Savannah American Business Clubs (AMBUCS). “This is a recognition of the dedication we have to AMBUCS and helping others in our community,” said scholarship recipient and AMBUCS student leader Alexandra Adams. “Most of us are paying for our education with loans, and the scholarship helps relieve some of the financial burden that comes with pursuing a graduate degree. I am very thankful that AMBUCS has considered me for this scholarship the past two years.” The organization has hosted a League of Exceptional Bowlers on Saturdays for more than 50 years. The DPT students join the Savannah AMBUCS league to assist bowlers with physical and intellectual disabilities to promote an inclusive and competitive environment. In addition to the hands-on experiences, DPT students have the opportunity to interact with different members of the community. “It shows our commitment to the inclusion of our community and our passion for encouraging movement for everyone, despite their limitations, to increase their quality of life,” Adams said. “The program reinforces our classroom training, as well as, enhances our communication skills with others. Each member of our DPT program gets as much of a benefit from attending AMBUCS as the bowlers do.” A century-old membership organization dedicated to helping people with disabilities, the Savannah AMBUCS awards scholarships to students pursuing careers in the allied health professions and who volunteer with AMBUCs. If you’re a journalist looking to cover this story or would like to learn more about the physical therapy and other programs at Georgia Southern University – then let us help. Barry Joyner is the dean of Georgia Southern University’s Waters College of Health Professions - simply click on his icon to arrange an interview today.





