Experts Matter. Find Yours.
Connect for media, speaking, professional opportunities & more.

Could Vitamin-A bring back your sense of smell after Covid?
Researchers at the University of East Anglia and James Paget University Hospital are launching a new project to see whether Vitamin A could help people regain their sense of smell after viral infections including Covid-19. Smell loss is a common symptom of Covid-19, but even before Covid, many viruses had been causing smell loss and distortion and while most people naturally regain their sense of smell within a couple of weeks, many have been left with on-going smell disorders. Previous research from Germany has shown the potential benefit of Vitamin-A, and the UEA team will explore how this treatment works to help repair tissues in the nose damaged by viruses. They hope that the study, which has been funded by the National Institute for Health Research (NIHR), could one-day help improve the lives of millions around the world who suffer from smell loss, by returning their fifth sense. Smell loss expert Prof Carl Philpott from UEA’s Norwich Medical School and James Paget University Hospitals NHS Trust, said: “The huge rise in smell loss caused by Covid-19 has created an unprecedented worldwide demand for treatment. “Even before the Covid-19 pandemic hit, smell loss was thought to affect an estimated five per cent of people, with viruses accounting for 1 in 10 of those. “And around one in ten people who experience smell loss as a result of Covid-19 report that their sense of smell has not returned to normal four weeks after falling ill. “It’s a big problem, and our previous research has shown the impact of smell loss – including depression, anxiety and isolation, as well as risk of danger from hazards such as gas and spoiled food, and changes in weight due to reduced appetite. “A key problem for patients and their clinicians is the lack of proven effective treatments. “A recent study from Germany showed that people treated with vitamin A nasal drops improved twice as much as those in the untreated group. “We want to find out whether there is an increase in the size and activity of damaged smell pathways in patients’ brains when they are treated with vitamin A nasal drops. “This would show recovery of the damage caused by common viral infections, including Covid-19, in the nose.” The research team will work with patients who have lost their sense of smell due to a viral infection. They will either receive a 12-week course of nasal vitamin A drops or inactive equivalent drops, and have their brains scanned before and after the treatment. The scans will be compared to those of a control group who have not been treated with vitamin A drops. Prof Philpott said: “The patients will be smelling distinctive odours - roses and rotten eggs - while special MRI brain scans are taken. “We will look for changes in the size of the olfactory bulb - an area above the nose where the smell nerves join together and connect to the brain. “We will also look at activity in areas of the brain linked to recognising smells,” he added. Duncan Boak, Founder and Chair of Fifth Sense, said: “At Fifth Sense we have engaged with thousands of people who have experienced changes in their ability to smell or taste as a result of the Covid 19 virus. They join an already large community of people with a smell disorder that pre-dates the pandemic. “The question we are most often asked is about available treatments to support recovery. Not being able to smell is not only physically distressing but can affect the enjoyment of social occasions and present hazards and risks that might never have been previously considered such as not being able to detect gas leaks or spoiled food. “Research into potentially successful interventions is vital to help people feeling the impact of smell disorders that affects the quality and enjoyment of their life.” To take part in this trial, patients need to be referred to The Smell and Taste Clinic at the James Paget University Hospital by their GP. Recruitment is expected to begin in December 2021. To find out more visit https://rhinology-group.uea.ac.uk/apollo-trial or contact apollo.trial@uea.ac.uk. The NIHR is the largest funder of research in the country, and is the research partner of the NHS and social care. To find out more about other NIHR research happening near you, visit www.bepartofresearch.uk.

A missed opportunity - hospital doctors must stop 'risky' medicines
Hospital doctors and pharmacists should stop ‘risky’ medicines before patients leave hospital - according to researchers at the University of East Anglia. One in two older people are prescribed a medicine which over time has become inappropriate or unnecessary. In a recent National Overprescribing Review titled ‘Good for you, good for us, good for everybody’, the government called on doctors and pharmacists working in GP surgeries to tackle the problem of overprescribing. But research from UEA’s School of Pharmacy has found that nine out of 10 older hospital patients and their family believe that inappropriate or unnecessary medicines should also be spotted and stopped whilst they are in hospital. And the team say that by the time people are back under their GP care, a major opportunity has been missed. Prof Debi Bhattacharya, from UEA’s School of Pharmacy, said: “We know that half of older people admitted to hospital arrive having been prescribed a medicine that over time has become inappropriate for them. These medicines will have more risks than benefits. “And their side effects cause problems, like making them feel drowsy, nauseous or have trouble getting to sleep. These problems impact a person’s quality of life to the extent that they can cause re-hospitalisation. “Our research has shown that very few patients have one of these ‘risky’ medicines stopped whilst in hospital. “Continuing medicines when they are not needed unnecessarily harms people and wastes NHS money. “The time is right to undertake research into ways of safely increasing the number of inappropriate and unnecessary medicines that are stopped,” she added. To tackle the problem, Prof Bhattacharya is leading a £2.4 million trial to stop risky medicines in hospital - in collaboration with researchers at the Universities of York, Newcastle, Leeds and Leicester, the Norfolk and Norwich University Hospital and Addenbrooke’s Hospital in Cambridge. Patient and Public Engagement lead for CHARMER, Katherine Murphy, said: “We are working with hospitals and GP organisations across England to see whether the new strategy works, helps people, causes no harm, and is good value for the NHS. “And for this trial to be meaningful to people, we need to make sure that we look at the things that matter to them when testing whether stopping a medicine has had a positive outcome.” The research team recently surveyed 200 people including patients, informal carers, doctors, nurses, pharmacists, physiotherapists and researchers to find out what they should look at in the trial. On reviewing the results Katherine Murphy said: “It was good to see that what people really want us to look at is whether patients can do the things that they want to do, not how much patients can do. “Being able to walk up a flight of stairs, for example, may be important to some patients but not to others. We need to make sure that medicines are prescribed that support people to get the best quality of life. In the trial, we also need to make sure that the way that we stop risky medicines causes no harm and is good value for the NHS.” For more information about the CHARMER study visit https://www.uea.ac.uk/web/groups-and-centres/charmer/about-the-research The research has been funded by the National Institute of Health and Social Care research.
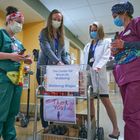
ChristianaCare recognized by American Medical Association with 2021 Joy in Medicine distinction
ChristianaCare one of only 44 nationwide to receive the distinction; one of only five to receive the highest level – Gold Recognition (WILMINGTON, Del. – Oct. 7, 2021) ChristianaCare has been named a recipient of the American Medical Association’s Joy in MedicineTM Health System Recognition Program. The distinction recognizes health systems that demonstrate a commitment to preserving the wellbeing of health care team members by engaging in proven efforts to combat work-related stress and burnout. The American Medical Association awarded ChristianaCare a “Gold Recognition” – the highest level within the program. Only 44 health systems nationwide received the Joy in Medicine distinction, with only four other health systems along with ChristianaCare achieving the Gold Recognition. “When caregivers feel supported and fulfilled in their work, the quality of both their experience and their patient’s experience improves,” said Heather Farley, M.D., MHCDS, chief wellness officer and head of ChristianaCare’s Center for WorkLife Wellbeing. “That’s why, when the COVID-19 pandemic struck, we deepened our investment of resources to support our caregivers. While there’s still a long way to go, we are grateful to receive this recognition as it affirms our commitment to helping our caregivers foster meaning, connection and joy in work and in life.” ChristianaCare received the “Gold Recognition” for achieving six criteria: An organization-wide commitment to improving physician wellbeing. An assessment of the costs of physician burnout. Evidence-based interventions to reduce and eliminate burnout. Leadership commitment to address areas for improvement. Interventions to improve teamwork. Structured programs that actively engage doctors to cultivate community at work. These criteria align with ChristianaCare’s commitment to support its caregivers in alignment with the organization’s core values of love and excellence. ChristianaCare has implemented structured ways of working that encourages leaders to create environments where their workers feel safe asking questions and feel empowered to identify and solve problems. ChristianaCare also uses numerous surveys and assessments to track progress in improving the wellbeing and experience of caregivers. ChristianaCare’s Unique Center for WorkLife Wellbeing ChristianaCare established the Center for WorkLife Wellbeing in 2016 to develop support systems to enable clinicians to reconnect with the joy and meaning in medicine. “We recognized the growing problem of stress and burnout in health care, and we made a decision to tackle it head-on,” said Janice E. Nevin, M.D., MPH, ChristianaCare president and CEO. “The work of our psychologists, researchers, clinicians and peer supporters in the Center for WorkLife Wellbeing is built on the understanding that when we care for ourselves, we are better able to care for others, resulting in decreased medical errors and a better experience of care for everyone involved.” The Center soon expanded its mission to support all of ChristianaCare’s caregivers, including those who don’t work in clinical roles. The Center also has received national recognition for its expertise and leadership in the field of workplace wellbeing. Throughout the pandemic, the Center for WorkLife Wellbeing has proactively shared a variety of resources to support caregivers as they work to provide safe, effective care and reduce the spread of COVID-19. This includes: The Care for the Caregiver program, which provides confidential individual peer support and group support to caregivers when they experience stress related to patient care or the workplace. Peer supporters and organizational leaders receive training so they can provide psychological first aid to caregivers whom they recognize are struggling as well as connect them to helpful resources if needed. Emotional support through mindfulness resources and regular rounds where the Center’s experts can check on staff wellbeing. OASIS Rooms, which are quiet sanctuaries inside the hospital where caregivers can go to take a break, de-stress, meditate or enjoy a chair massage. 24/7 mental health services and programs to help caregivers maintain healthy habits including proper exercise, sleep and nutrition. Fitness centers that are free for all caregivers to use and provide easy access to exercise and fitness programs. “I always use the analogy, you can’t take the canary out of the coal mine and teach it to be more resilient and then put it back in the same coal mine and expect it to survive,” Dr. Farley said. “You actually have to change the coal mine – the environment surrounding our caregivers and clinicians. That’s what we’re doing in the Center for WorkLife Wellbeing.” Solutions to a National Problem A national study examining the experiences of physicians and other health care workers who worked in health systems during the COVID-19 pandemic found that 38% self-reported experiencing anxiety or depression, while 43% suffered from work overload and 49% had burnout. “The COVID-19 pandemic has placed extraordinary stress on physicians and other health care professionals,” said American Medical Association President Gerald E. Harmon, M.D. “While it is always important for health systems to focus on the wellbeing of care teams, the imperative is greater than ever as acute stress from combatting the COVID-19 pandemic has contributed to higher rates of work overload, anxiety and depression. The health systems we recognize today are true leaders in promoting an organizational response that makes a difference in the lives of the health care workforce.” Launched in 2019, the Joy in Medicine Health System Recognition Program is a component of the American Medical Association’s practice transformation efforts, an ambitious initiative to advance evidence-based solutions to address the physician burnout crisis. Candidates for the program were evaluated according to their documented efforts to reduce work-related burnout through system-level drivers. Scoring criteria were based on demonstrated competencies in commitment, assessment, leadership, efficiency of practice environment, teamwork and support. About ChristianaCare Headquartered in Wilmington, Delaware, ChristianaCare is one of the country’s most dynamic health care organizations, centered on improving health outcomes, making high-quality care more accessible and lowering health care costs. ChristianaCare includes an extensive network of primary care and outpatient services, home health care, urgent care centers, three hospitals (1,299 beds), a freestanding emergency department, a Level I trauma center and a Level III neonatal intensive care unit, a comprehensive stroke center and regional centers of excellence in heart and vascular care, cancer care and women’s health. It also includes the pioneering Gene Editing Institute. ChristianaCare is nationally recognized as a great place to work, rated by Forbes as the 5th best health system to work for in the United States and by IDG Computerworld as one of the nation’s Best Places to Work in IT. ChristianaCare is rated by HealthGrades as one of America’s 50 Best Hospitals and continually ranked among the nation’s best by Newsweek and other national quality ratings. ChristianaCare is a nonprofit teaching health system with more than 260 residents and fellows. With its groundbreaking Center for Virtual Health and a focus on population health and value-based care, ChristianaCare is shaping the future of health care. #####
Experts in the Media – UConn’s Dr. David Banach is the go-to voice on COVID boosters
As COVID continues to wreak havoc across the globe, health systems in America are overwhelmed. And as the debate about a third shot continues, the FDA is prepared to allow Pfizer vaccine boosters as early as this week to those over 65 and to people at a higher health risk if exposed to the virus. UConn epidemiologist Dr. David Banach offered his expert perspective and insight on the need and effectiveness for those looking to learn more about booster shots and COVID vaccines: Booster shots of Pfizer’s COVID-19 vaccine may be administered as early as Friday, but who will get one is still up for discussion. “What the FDA review showed was in the general population, at this date and time, there wasn’t sufficient data to support booster doses,” said Dr. David Banach, hospital epidemiologist at UConn Health. Last week, the FDA’s advisory committee voted overwhelmingly not to recommend a third shot for people 16 and up. However, they did vote to authorize a booster dose at least six months after full vaccination for people who are 65 and older as well as individuals who are at high risk for severe COVID. “In older populations, there seems to be some potential benefit to giving a third dose within the Pfizer group,” said Dr. Banach. Dr. Banach said more information is expected in the days to come as this matter heads to the CDC’s independent advisory panel this week. “It’s going to provide more granular recommendations on how to proceed with that 65 and older group and potentially other groups as well,” said Dr. Banach. He added one of the groups up for discussion is healthcare workers. There continues to be an enormous amount of coverage and questions about vaccines and COVID-19, and if you are a journalist looking to know more and include an expert in your story, then let us help. Dr. David Banach is one of the lead experts on COVID-19 in America. He is available to speak with media regarding vaccination and what the future holds with COVID-19. To book an interview, simply click on his icon today.

Podcast: 3D printing’s vital solution to medical problem caused by COVID-19
"They were looking to solve a problem and I was able to use my additive manufacturing knowledge to help them out, and the result of that was that we developed a new technology and span a company out of it." Dr Mark Prince Senior Lecturer in Mechanical Engineering Aston University New device created in Aston University lecturer's home during coronavirus lockdown Aston Business School expert explains how 3D printers are already used to make hearing aids, dental crowns and hips ‘Imagination is the only limit’ for additive manufacturing’s future, according to Dr Ahmad Beltagui A senior lecturer at Aston University is helping ear, nose and throat (ENT) clinics around the world by using the hi-tech ingenuity of 3D printing. Dr Mark Prince used 3D printing to prototype and produce a valve for a mask so that ENT surgeons could continue to examine and treat patients without fear of spreading the virus. Dr Prince, a senior lecturer in mechanical engineering at Aston University, was talking about his experiences in the latest episode of the 'Aston means business' podcast, presented by journalist Steve Dyson. The podcast also features Dr Ahmad Beltagui from Aston Business School, who talks about the wider benefits, some downsides and future potential of 3D printing in successfully disrupting traditional manufacturing. Dr Prince said his interest in additive manufacturing, or 3D printing, peaked after meeting two consultant ENT surgeons in the West Midlands. He said: "They were looking to solve a problem and I was able to use my additive manufacturing knowledge to help them out, and the result of that was that we developed a new technology and span a company out of it. "The company is Endoscope-i Ltd, founded in 2012 and now with an annual turnover of £200,000. The idea was simple: can we get medical endoscopic images of the ears and throat using a smartphone and we came up with a technique to do that." He said that, traditionally, he would have used large, expensive equipment to prototype the systems and new products. However, that wasn't possible with most of the university closed down at the height of the pandemic last year. He, therefore, had to look at other technologies that were safe to use in the home without breaking lockdown restrictions. Dr Prince explained: "When we are looking at diseases or concerns of the throat and nose we often stick an endoscope up the nose and down the throat, but of course you can't do that through a mask. "One of the founding members, Mr Ajith George, suggested that we could put a valve in the mask that allowed an endoscope to pass through it and allow the procedure to go ahead without breaking containment." "Work on the device started in mid-March 2020 and was ready for free supply to the NHS in November. Dr Prince added: "What that has allowed the NHS to do is any ENT clinic was able to fit it to a mask, put the mask on the patient, and carry on with an endoscopy procedure without all of the concerns of the pandemic." Meanwhile, Dr Ahmad Beltagui, a lecturer in operations and information management at Aston Business School, said you could get 3D printers from as little as £200 all the way up to expensive versions working with "exotic materials" like titanium. He said there were four main benefits to manufacturers: "Compared to traditional manufacturing methods you can produce shapes that are harder to produce; you can produce things in very small volumes; you can innovate faster and produce lots of prototypes, and you can produce things nearer to where they are required so you don't have to produce in a factory in one place and transport somewhere else." Dr Beltagui said: "The COVID-19 pandemic saw 3D printers used in homes to produce equipment such as cheap face visors for their local hospitals. The great thing about 3D printing is anyone can produce anything they want. "That's also the biggest risk – there is no control over what people produce or how safely they produce it. "At the beginning of the pandemic, someone in Italy found that they could produce some spare parts to keep the ventilators in their local hospital going. But then a few days later the manufacturer of those ventilators was considering whether or not it should take legal action." However, he said the printing machines had gradually become more reliable and there was a better level of quality, while the cost was coming down. Dr Beltagui added: "As to the future, the only limit is your imagination."

Covering World Breastfeeding Week? Our experts are here to help
August 1-7 is World Breastfeeding Week, and the University of Mary Washington has the ideal expert for any journalist looking to learn more or cover this important topic. Did you know that breastfeeding is one of the top maternal priorities for many organizations, including the World Health Organization (WHO), the American Academy of Pediatrics (AAP) and the Centers for Disease Control and Prevention (CDC)? Assistant Professor of Communication Elizabeth Johnson-Young has done extensive research on women’s intentions to breastfeed and how the communication they receive during pregnancy and postpartum from various sources such as doctors, lactation consultants, friends and family, magazines, books and parenting groups can impact the decision to breastfeed. She's also explored the connections between breastfeeding and body satisfaction. Dr. Elizabeth Johnson-Young is a published expert on health communication, especially maternal and family health. She is ready to help if you are looking to cover this topic - simply click on her icon now to arrange an interview today.

Cyber attacks and ransomware are incidents that are happening more and more often. They are threatening America’s energy supply, food chain and critical infrastructure. Recently, two Georgia hospitals were victims of a recent attack. Media from across the country asked experts like Frank Katz, director of Georgia Southern University's Center for Applied Cyber Education, who is vulnerable and why. Katz, who directs the Center for Applied Cyber Education at Georgia Southern University’s Armstrong Campus in Savannah, said hospitals can be targets for extortion as well as sources of personal identifying information that can aid in further fraud. “They are more likely to pay than another type of business because it’s a life and death situation,” Katz told WSAV-TV. “It really has become a situation of money, pure and simple. These are thieves that know they can extort the money and often get it.” June 21 – Associated Press Frank Katz, director of the Center for Applied Cyber Education at Georgia Southern University, says hospitals are often easy targets. Having so many employees, he says user IDs and passwords can be easy to figure out. Plus, they’re dealing with emergency medical care. “They are more likely to pay than another type of business because it’s a life and death situation,” Katz said. June 21 – NBC News If you are a reporter looking to cover this subject and speak with Frank Katz, Georgia Southern’s Director of the Center for Applied Cyber Education – then let our experts help. Frank Katz, director of the Center for Applied Cyber Education is available, simply click on his icon or reach out to Georgia Southern Director of Communications Jennifer Wise at jwise@georgiasouthern.edu and she’ll assist with connecting you for an interview today.

Starter vape packs to be handed out in hospitals
A new trial from the University of East Anglia will see smokers attending hospital emergency departments given e-cigarette starter packs to help them quit. The initiative comes as a Cochrane Review - the international gold standard for high quality, trusted health information – about vaping is updated today. The review, led by the University of Oxford and involving the UEA team, shows how nicotine electronic cigarettes could increase the number of people who stop smoking compared to nicotine replacement therapy – such as chewing gum and patches – and compared to electronic cigarettes that do not contain nicotine. The new trial will offer stop smoking advice and an e-cigarette ‘starter pack’ to patients attending hospital emergency departments for any reason, to try to encourage and support them to quit smoking – even for those who might not have considered it before. The new trial is funded by the National Institute for Health Research (NIHR) and will be run by the Norwich Clinical Trials Unit at UEA. Prof Caitlin Notley, from UEA’s Norwich Medical School, said; “Many people who smoke want to quit, but find it difficult to succeed in the long term. “Electronic cigarettes mimic the experience of cigarette smoking because they are hand-held and generate a smoke-like vapour when used. They can be an attractive option for helping people switch from smoking, even if they have tried and failed in the past. “We know that they are much less harmful than smoking tobacco, and that they have been shown to help smokers quit. Trial co-lead Dr Ian Pope, also from UEA’s Norwich Medical School and an emergency physician, said: “Emergency Departments in England see over 24 million people each year of whom around a quarter are current smokers. “Attending the Emergency Department offers a valuable opportunity for people to be supported to quit smoking, which will improve their chances of recovery from whatever has brought them to hospital, and also prevent future illness.” The study will run over 30 months across five hospitals in England and Scotland – at the Norfolk and Norwich University Hospital, the Royal London Hospital and Homerton University Hospital in London, Leicester Royal Infirmary and the Royal Infirmary of Edinburgh. Smokers who agree to take part will be randomly assigned to receive either smoking advice during their emergency department wait, an e-cigarette starter pack and referral to local stop smoking services, or just written information about locally available stop smoking services. Both groups of patients will be asked if they are still smoking one, three and six months after they attended hospital. The research team hope to eventually recruit around 1,000 smokers to the trial. Prof Notley said: “We’ll be looking at the number of people who successfully quit smoking across both groups, to see which intervention works best. We’ll also work out how much it would cost to roll the scheme out nationally,” she added. ‘Electronic cigarettes for smoking cessation (Review)’ is published by the Cochrane Library on April 29, 2021.

Thousands of men to trial prostate cancer home testing kit
Thousands of men worldwide are to receive a home test kit for prostate cancer – thanks to pioneering research from the University of East Anglia and the Norfolk and Norwich University Hospital (NNUH). The research team are trialling a new home-testing ‘Prostate Screening Box’ to collect men’s urine samples at-home. The urine samples will be used to analyse the health of the prostate in 2,000 men in the UK, Europe and Canada. This simple urine test is intended to diagnose aggressive prostate cancer and in a pilot study predicted which patients required treatment up to five years earlier than standard clinical methods. Lead researcher Dr Jeremy Clark from the University of East Anglia 'unboxes' the new home testing kit live on Sky News. The Prostate Screening Box has been developed in collaboration with REAL Digital International Limited to create a kit that fits through a standard letterbox. It means that men can provide a urine sample in the comfort of their own home, instead of going into a clinic or having to undergo an uncomfortable rectal examination. The research team hope that it could revolutionise diagnosis of the disease. Lead researcher Dr Jeremy Clark, from UEA’s Norwich Medical School, said: “Prostate cancer is the most common cancer in men in the UK. However it usually develops slowly and the majority of cancers will not require treatment in a man’s lifetime. It is not a simple matter to predict which tumours will become aggressive, making it hard to decide on treatment for many men. “The most commonly used tests for prostate cancer include blood tests, a physical examination known as a digital rectal examination (DRE), an MRI scan or a biopsy. “We have developed the PUR (Prostate Urine Risk) test, which looks at gene expression in urine samples and provides vital information about whether a cancer is aggressive or ‘low risk’. “The Prostate Screening Box part sounds like quite a small innovation, but it means that in future the monitoring of cancer in men could be so much less stressful for them and reduce the number of expensive trips to the hospital. “The prostate lies just below the bladder. It constantly produces secretions which naturally flow into the urethra - the tube through which urine passes from the bladder. The prostatic secretions carry cells and molecules from all over the prostate which are flushed out of the body on urination. We collect these and examine them. It’s a way of sampling the whole prostate in one go. “As the prostate is constantly secreting, the levels of biomarkers in the urethra will build up with time. Collecting from the first wee of the day means that overnight secretions can be collected which makes the analysis more sensitive.” The team have previously trialled the kit with a small group of participants, but in the next phase of the research study are rolling it out to thousands. Men taking part in the trial will receive a home urine-sampling kit and will be asked to provide two urine samples – one to be taken first thing in the morning and the second an hour later. The samples will then be sent back to the lab for analysis. Dr Clark said: “Feedback from early participants showed that the at-home collection was much preferred over sample collection in a hospital. “We hope that using our Prostate Screening Box could in future revolutionise how those on ‘active surveillance’ are monitored for disease progression, with men only having to visit the clinic after a positive urine result. “This is in contrast to the current situation where men are recalled to the clinic every six to 12 months for a range of tests including DRE, PSA tests, painful and expensive biopsies and MRI. We are working to develop the test to help patients in three years’ time. “A negative test could enable men to only be retested every two to three years, relieving stress to the patient and reducing hospital workload,” he added. Robert Mills, Consultant Clinical Director in Urology at NNUH, said: “This simple, non-invasive urine test has the potential to significantly change how we diagnose and manage early prostate cancer for the benefit of patients and health care systems. It may enable us to avoid unnecessary diagnosis of low risk disease as well as managing patients more appropriately with surveillance for those with low risk of progression and early curative treatment for those at high risk of progression.” Paul Villanti, executive director of programs at Movember, said: “The PUR test has great potential to transform the way prostate cancer is managed. Not only can it accurately predict when a man’s disease will become aggressive and require treatment, but it has the added advantage of allowing men to complete it at home. “We are proud to have supported the development of the PUR test from its early stages as part of our Global Action Plan on Biomarkers, through to this trial involving thousands of men across the world. “Through our Global Action Plan on active surveillance, we have been able to identify hundreds of men from the UK, Germany, Italy and Canada who are suitable to take part in this trial. “We hope it will speed up the trial’s progress and get this test included as part of clinical care for men as quickly as possible.” The research has been funded by a Movember and Prostate Cancer UK Innovation award, the Masonic Charitable Foundation, the Bob Champion Cancer Trust, the King family, the Andy Ripley Memorial Fund, the Hargrave Foundation, Norfolk Freemasons and the Tesco Centenary Grant.

New CBS Sitcom "United States of Al" Taps Experience of Social Work Student and Veteran
On April 1, 2021, CBS premiered United States of Al - a new comedy from producer Chuck Lorre (Two and a Half Men, Big Bang Theory) about a Marine combat veteran struggling to readjust to civilian life and the interpreter who served with his unit in Afghanistan and has just arrived to start a new life in America. The show explores the relationship between these two men and how they help each other adjust to their new lives. So, what does a CBS sitcom have to do with the USC Suzanne Dworak-Peck School of Social Work? Enter Master of Social Work (MSW) student Josh Emerson, who landed in the right place at the right time through his field internship at No One Left Behind. No One Left Behind (NOLB) is an all-volunteer, national nonprofit organization that supports recipients of the Special Immigrant Visa (SIVs), and those pursuing an SIV. The founders of No One Left Behind believe the U.S. has a moral obligation to protect these interpreters, and their families, who served side-by-side with American soldiers. Emerson, a veteran of the U.S. Army who deployed to Iraq and Afghanistan, is very familiar with Iraqi and Afghan interpreters. “I went on missions with these interpreters, got to know them, built relationships with them,” he said. “I was so very happy to be able to work with them in this capacity. In addition to providing resources for SIV ambassadors living in the United States, NOLB advocates on behalf of the SIV population to the executive and legislative branches of government provides subject matter expertise to the media, and partners with U.S. businesses to provide opportunities for what they call “this next generation of Americans.” Alea Nadeem, MSW ’15, is a board member of NOLB and reached out to USC with a field internship opportunity for social workers to do macro-level clinical work in a nonprofit setting. Nadeem became Emerson’s field instructor. “What Josh has brought to No One Left Behind has never been brought to the board before,” Nadeem said. “They now see the value in social work.” Bringing the issue to a larger audience Chase Millsap, a consultant and writer on United States of Al, is a former board member of No One Left Behind. “I am still very supportive, impressed and proud of all the work the NOLB team does on a daily basis,” he said. A veteran of the U.S. Marine Corps and U.S. Army Special Forces, he holds a master’s degree from USC Sol Price School of Public Policy. "USC helped me to learn the tools about how to connect entertainment and policy,” Millsap said. “United States of Al is a perfect example of those two worlds coming together in a powerful (and funny) way.” Millsap’s idea was to bring the issues around SIVs into America's living rooms, in a way that would make them relatable. Emerson’s experience as a veteran, his clinical and project management skills obtained through his social work studies and his stellar ability to work one-on-one with SIV recipients and applicants allowed him to inform the show’s stories with a wide breadth of knowledge. Emerson joined James Miervaldis, chairman of the NOLB board, in helping the writers and actors on the show understand the SIV issues, the ways in which NOLB provides assistance and advocacy, and sharing funny stories of cultural differences between Afghans and Americans. Emerson and Miervaldis have also been able to include some of NOLB’s SIV ambassadors in the process, those with an SIV who have already established themselves in the U.S. and are contracted by NOLB to help others assimilate. “They’re talking to the exact people they're portraying,” Emerson said. Nadeem sees Emerson’s contribution to the show as another platform through which to educate. “There are a lot of different tentacles to social work, and it may not seem like the most obvious place in TV and film, but it is,” she said. The show itself touches on everything social workers value ― service, challenging social injustice, dignity and worth of a person, the importance of human relationships and integrity. “This just makes so much sense that a social worker would be involved in this show because that's what we're always trying to communicate to a larger audience,” Nadeem said. “Through this show, you can make a greater impact for these folks to sort of assimilate them to be American citizens, and then also have the whole world appreciate their culture and appreciate what they've done for our nation to keep U.S. service members safe.” A valued member of the team Emerson, a father of five who resides in New Hampshire, knew he wanted to work with veterans after leaving military service. He felt that an MSW was the most versatile degree for this and chose the USC Suzanne Dworak-Peck School of Social Work because of its military social work track. “I think to be a good social worker you need to have experience in life,” Emerson said. “To have seen some things, or been through some things, to understand the population you're dealing with and what they're going through.” When Emerson began his internship at NOLB in 2020, Miervaldis immediately began working with him to focus on SIVs who recently had come to the United States. The first case Miervaldis assigned to Emerson was an SIV family with two young children who needed emergency surgery at a specialty hospital in Washington D.C. “This SIV packed up his family, his pregnant wife and the two kids, used up all his money to take them by bus from Texas to D.C. in the middle of a pandemic and ended up in a bad part of town,” Miervaldis said. As the SIV’s assigned caseworker, Emerson established a relationship and trust with the SIV, helped him obtain safe housing and a job interview, and coordinated details for the children’s surgery with the hospital. “He’s gone and done everything,” Miervaldis said. “We are very proud of Josh’s initiative and empathy for a family in such need. No One Left Behind is the safety net for our allies.” Last year, NOLB helped over 600 families with visas and resettlement. “Josh has exceeded all our expectations and done so while communicating with clients who speak in broken English, Dari and Pashtu, struggling during a pandemic,” Miervaldis said. “His professionalism and empathy are great credits to USC. We would not be where we are today without him. That is not hyperbole.” Miervaldis hopes NOLB will have more social work interns from USC to continue Emerson’s work. For him, Emerson’s project management skills have been the greatest asset, creating a new process for how NOLB provides help for SIV families. “We told Josh, you're a pathfinder, you're a pioneer,” Miervaldis said. “We need to figure out very quickly what works, what doesn't work, and he took it and said, ‘okay, point me in the right direction.’ He’s very much valued as a member of the team.” From advocacy to TV No One Left Behind gets about 20 messages every day from Iraqi or Afghan interpreters who served with U.S. forces in their countries, and who now receive daily death threats from the Taliban. “They're not allowed to live in their homes or their neighborhoods anymore because they helped the U.S.,” Emerson said. “Now the U.S. is withdrawing from all these countries, and the Taliban and terrorist activities in general are picking up, and these people are getting pressured and killed. NOLB has over 300 cases of SIVs who have been killed waiting for their visas.” Emerson hopes that the added exposure from United States of Al will bring awareness particularly to service members about what these interpreters are experiencing and how they can help. One of the requirements for an SIV is a letter of recommendation from the U.S. service member with whom they served, and those have been the most difficult items for SIV applicants to secure. “I have been able to provide some input to what should be addressed in the show,” Emerson said. “It's interesting to see how advocacy on an issue can turn into something this large scale.” See more news from USC Suzanne Dworak-Peck here.







