Experts Matter. Find Yours.
Connect for media, speaking, professional opportunities & more.

Local neighborhood conditions are important for children’s brain development
Growing up in a disadvantaged neighborhood is related to children’s brain structure and neurocognitive performance, according to a study published May 3, 2021 in the journal JAMA Pediatrics. It is associated with the brain’s cortical structure and volume as well as how children pay attention, their executive function, reading, flexible thinking, and other tasks that support learning. These differences could potentially contribute to other inequities during adolescence as well as later in life for these children, though there is no evidence that such neighborhood-related differences are fixed or immutable. Children’s brains exhibit plasticity, meaning that they can change and grow in response to learning and experience. The study’s findings shine a spotlight on the larger population trend and do not serve as a predictor of any individual child’s outcome. “This points to the importance of investing in policies and programs that help improve local neighborhoods and to support and empower communities to promote children’s neurodevelopment and long-term health and well-being,” said Daniel A. Hackman, assistant professor at the USC Suzanne Dworak-Peck School of Social Work and lead author of the study. Researchers from the USC Suzanne Dworak-Peck School of Social Work and the Keck School of Medicine of USC used data from the Adolescent Brain and Cognitive Development (ABCD) Study, collected from October 2016 – 2018. The ABCD Study is the largest long-term study of brain development and child health ever conducted in the United States. “Disadvantaged neighborhoods may lack quality health services, access to nutritional foods, and well-maintained parks and rec facilities,” said Megan Herting, assistant professor in the department of preventive medicine at the Keck School of Medicine at USC and senior author of the study. “They may also expose residents to more pollutants or social stressors.” In addition to Hackman and Herting, study authors include Dora Cserbik, Jiu-Chiuan Chen, and Rob McConnell of the department of preventive medicine at Keck School of Medicine; Bita Minaravesh of the USC Dornsife Spatial Sciences Institute; and Kiros Berhane of the Department of Biostatistics at Columbia University Mailman School of Public Health. Neighborhood disadvantage and the brain The study participants were 8,598 nine- to eleven-year-old children in 21 sites from the ABCD Study, and includes youth from diverse backgrounds, family income levels and neighborhood environments. Using this ABCD data, the multidisciplinary team of researchers tested whether neighborhood disadvantage is associated with neurocognition and brain structure through the National Institute of Health Toolbox Cognition Battery and magnetic resonance imaging (MRI) scans. Neurocognition refers to specific cognitive functions related to particular neural systems, such as executive function, memory, problem-solving and perception. Executive function is the set of cognitive functions that allows people to select behaviors, make efforts to regulate or control their behavior or thinking in given situations, and to focus on goals despite distractions. Brain structure refers to global and regional measures of the brain’s cortex and subcortex, such as volume and surface area. The researchers found that neighborhood disadvantage was associated with worse neurocognitive performance on nearly all tasks and smaller cortical surface area, as well as cortical volumes and subcortical volumes, across the whole brain. The associations remain after adjusting for family socioeconomic status and largely remain after adjusting for perceptions of neighborhood safety. “Our findings aren't specific to the child's home life, as we accounted for socioeconomic factors at each child's home,” Herting said. “But the research suggests neighborhoods may have different levels of social and educational resources and opportunities that can impact a child's neurodevelopment.” Disadvantaged neighborhoods are those in which people generally have lower levels of income, employment and education. Growing up in these conditions can be stressful for children and adults. However, comparing disadvantaged neighborhoods across the country is challenging to social work researchers, who understand that when looking at national samples they may pick up regional differences for which they must account. Neighborhood similarities and differences The impressive scope and scale of the ABCD study made it possible for these researchers to delve into rich local data that enabled them to understand the similarities and differences of disadvantaged neighborhoods within the context of their cities. Hackman, whose research interests include understanding neighborhoods and the context that children and adolescents grow up in, wanted to be able to look at the research question from both the national perspective as well as the local perspective. “This is the first large, national study of neurodevelopment to determine that the role of neighborhood disadvantage is similar across all regions of the country, and we found that what mattered most were the local differences in neighborhood disadvantage within each city, rather than how cities differ from each other overall” Hackman said. “This highlights the broad relevance of neighborhood disadvantage, and the importance of unique local conditions. His interest was even more piqued when he saw a clear narrative emerge from the data. “The consistency of the data was so compelling,” Hackman said. Though disadvantaged neighborhoods may vary from city to city, the researchers found the associations were largely consistent across 21 metropolitan areas within the U.S. For policymakers, a takeaway is that neighborhoods were related to these important aspects of child development everywhere, and that though each city is different, the unique local conditions are important to address. In addition, the global relationship between neighborhood and overall brain structure and neurocognitive performance suggest that intervention approaches may be most successful if they are comprehensive and focused on improving children’s contexts, rather than narrowly targeted to the development of particular cognitive skills. “This research is important as it not only highlights that neighborhoods matter, but it also suggests that promoting neighborhood equity based on the unique local conditions within cities could be important for the short and longer-term health and overall development of children and adolescents,” Hackman said. According to the study, although the magnitudes of association between disadvantaged neighborhoods and neurocognition and brain structure are statistically small, they are potentially meaningful. One reason is because even small effects may have large consequences as they accumulate over time at a population level. Another reason is because these are comparable to, but smaller, than effect sizes for family socioeconomic status in these models. “There is also considerable evidence of resilience,” Hackman noted, as the authors caution that these associations are not predictive at the individual level. In particular, many youth from disadvantaged neighborhoods outperform their peers from more affluent neighborhoods, and also have larger cortical surface area and subcortical volume as well. In other words, living in a disadvantaged neighborhood is not deterministic and does not automatically predict any pattern of neurocognition and brain structure for any individual. Instead, the association uncovered by these researchers points to more reasons why improvements to neighborhoods can bring positive change. “Future research is needed to determine if our findings are, in fact, attributable to differences in community-based resources or differences in quality of schooling,” Herting said. “However, our findings do add to a growing literature suggesting the importance of neighborhoods and how they may contribute to place-based disparities in health and well-being in America.”

Thousands of men to trial prostate cancer home testing kit
Thousands of men worldwide are to receive a home test kit for prostate cancer – thanks to pioneering research from the University of East Anglia and the Norfolk and Norwich University Hospital (NNUH). The research team are trialling a new home-testing ‘Prostate Screening Box’ to collect men’s urine samples at-home. The urine samples will be used to analyse the health of the prostate in 2,000 men in the UK, Europe and Canada. This simple urine test is intended to diagnose aggressive prostate cancer and in a pilot study predicted which patients required treatment up to five years earlier than standard clinical methods. Lead researcher Dr Jeremy Clark from the University of East Anglia 'unboxes' the new home testing kit live on Sky News. The Prostate Screening Box has been developed in collaboration with REAL Digital International Limited to create a kit that fits through a standard letterbox. It means that men can provide a urine sample in the comfort of their own home, instead of going into a clinic or having to undergo an uncomfortable rectal examination. The research team hope that it could revolutionise diagnosis of the disease. Lead researcher Dr Jeremy Clark, from UEA’s Norwich Medical School, said: “Prostate cancer is the most common cancer in men in the UK. However it usually develops slowly and the majority of cancers will not require treatment in a man’s lifetime. It is not a simple matter to predict which tumours will become aggressive, making it hard to decide on treatment for many men. “The most commonly used tests for prostate cancer include blood tests, a physical examination known as a digital rectal examination (DRE), an MRI scan or a biopsy. “We have developed the PUR (Prostate Urine Risk) test, which looks at gene expression in urine samples and provides vital information about whether a cancer is aggressive or ‘low risk’. “The Prostate Screening Box part sounds like quite a small innovation, but it means that in future the monitoring of cancer in men could be so much less stressful for them and reduce the number of expensive trips to the hospital. “The prostate lies just below the bladder. It constantly produces secretions which naturally flow into the urethra - the tube through which urine passes from the bladder. The prostatic secretions carry cells and molecules from all over the prostate which are flushed out of the body on urination. We collect these and examine them. It’s a way of sampling the whole prostate in one go. “As the prostate is constantly secreting, the levels of biomarkers in the urethra will build up with time. Collecting from the first wee of the day means that overnight secretions can be collected which makes the analysis more sensitive.” The team have previously trialled the kit with a small group of participants, but in the next phase of the research study are rolling it out to thousands. Men taking part in the trial will receive a home urine-sampling kit and will be asked to provide two urine samples – one to be taken first thing in the morning and the second an hour later. The samples will then be sent back to the lab for analysis. Dr Clark said: “Feedback from early participants showed that the at-home collection was much preferred over sample collection in a hospital. “We hope that using our Prostate Screening Box could in future revolutionise how those on ‘active surveillance’ are monitored for disease progression, with men only having to visit the clinic after a positive urine result. “This is in contrast to the current situation where men are recalled to the clinic every six to 12 months for a range of tests including DRE, PSA tests, painful and expensive biopsies and MRI. We are working to develop the test to help patients in three years’ time. “A negative test could enable men to only be retested every two to three years, relieving stress to the patient and reducing hospital workload,” he added. Robert Mills, Consultant Clinical Director in Urology at NNUH, said: “This simple, non-invasive urine test has the potential to significantly change how we diagnose and manage early prostate cancer for the benefit of patients and health care systems. It may enable us to avoid unnecessary diagnosis of low risk disease as well as managing patients more appropriately with surveillance for those with low risk of progression and early curative treatment for those at high risk of progression.” Paul Villanti, executive director of programs at Movember, said: “The PUR test has great potential to transform the way prostate cancer is managed. Not only can it accurately predict when a man’s disease will become aggressive and require treatment, but it has the added advantage of allowing men to complete it at home. “We are proud to have supported the development of the PUR test from its early stages as part of our Global Action Plan on Biomarkers, through to this trial involving thousands of men across the world. “Through our Global Action Plan on active surveillance, we have been able to identify hundreds of men from the UK, Germany, Italy and Canada who are suitable to take part in this trial. “We hope it will speed up the trial’s progress and get this test included as part of clinical care for men as quickly as possible.” The research has been funded by a Movember and Prostate Cancer UK Innovation award, the Masonic Charitable Foundation, the Bob Champion Cancer Trust, the King family, the Andy Ripley Memorial Fund, the Hargrave Foundation, Norfolk Freemasons and the Tesco Centenary Grant.

Social Work is Advancing Addiction Science Research
Tens of thousands of Americans die from drug use and addiction every year, with overdoses killing over 63,000 people in America in 2016, according to the National Institute on Drug Abuse. Add in deaths linked to alcohol overuse and tobacco, and the number climbs above half a million Americans. The collective work of several researchers at the USC Suzanne Dworak-Peck School of Social Work, in collaboration with other USC faculty and outside organizations, is advancing knowledge of substance use disorders. Social work has become a hub where researchers and practitioners drive understanding and improve treatment for this disease that impacts millions of families each year. “Either as a cause or consequence, addiction relates to every problem we deal with in social work,” said John Clapp, professor and associate dean for research and faculty development at the USC Suzanne Dworak-Peck School of Social Work. Addiction’s complexity The social work field is uniquely poised to help effect change because of its holistic approach to individual well-being and the public good. According to Clapp, substance use disorder problems are inherently ecological, impacting and being impacted by individuals, families, peers, neighborhoods, communities and public policy in complex and dynamic ways. Untangling those causes and effects and interdependencies is one part of the solution. The other part is understanding that simple solutions may stay out of reach. “We will not find a one-size-fits-all answer,” said Clapp. Looking at addiction as a genetic, psychological or sociological issue only shows one piece of the overall cause. A comprehensive approach is essential, he said, especially when statistics from the National Institute on Alcohol Abuse and Alcoholism (NIAAA) show alcohol use disorders alone as the third leading cause of preventable death in the world. A hub for addiction science The need for a transdisciplinary response to this worldwide crisis was behind the 2018 creation of the USC Institute on Addiction Science (IAS), a joint venture between social work and the Keck School of Medicine of USC, with membership from 10 different schools, colleges and hospitals. Its vision is to strengthen the discipline of addiction science and improve the lives of those touched by the disease. Clapp is co-director of the institute and one of its founding architects. IAS is quickly becoming the foremost place for a broad effort focused on addiction that brings together researchers from the fields of public health, social work, law, public policy, mathematicians, computer engineers and others in recognition of the promise of new approaches to longstanding problems. The USC Suzanne Dworak-Peck School of Social Work has eight faculty making substantial contributions to the prevention of addiction-related disorders as members of the IAS: Professor Avalardo Valdez, associate professors Julie Cederbaum and Alice Cepeda, and assistant professors Jordan Davis, Shannon Dunn, Jungeun Olivia Lee, Danielle Madden, and Hans Oh. “Social work brings one of the broadest perspectives on the underpinnings and solutions to the addiction crisis,” said Adam Leventhal, director of IAS and professor of preventive medicine and psychology at Keck. “By approaching addiction as a health condition and a social justice issue, social work brings to the table the opportunity for high-impact, multi-modal intervention and social policy approaches, which are needed to address the addiction epidemic.” A holistic approach Social work faculty are raising the bar in addiction science research, developing new and novel approaches to improving outcomes for those affected by addiction. In a study recently published in Addiction, a multidisciplinary team lead by Davis and Clapp found gender differences in the risk factors for relapse following treatment for opioid use disorder. The study was the first in this field to use machine learning techniques to process large data sets and identify risk factors for relapse, said Davis, who also serves as associate director of the USC Center for Artificial Intelligence in Society (CAIS). The findings may result in more personalized treatment for opioid use disorder with lasting results. This dovetails with additional research Davis is conducting with computer science engineers at CAIS to collect and input neighborhood and census data into their models in an effort to better understand how these macro variables affect relapse. “We are finding that data points such as crime statistics, population density and concentrated poverty tend to be some of the most important predictors of relapse, over and above individual-level predictors such as impulsivity, motivation or gender,” Davis said. These findings echo Clapp’s description of addiction as ecological and point to the need for holistic solutions. “These machine learning techniques are helping us gain an apparent picture of what the most important factors are surrounding someone’s recovery,” Davis said. “Environment matters greatly.” Davis is also collaborating closely with Eric Pedersen, associate professor at Keck School of Medicine at USC, on several research efforts examining substance use among veterans. Most recently, they have assembled a survey group of approximately 1,200 veterans whom they survey quarterly about their well-being. A recently conducted survey of the group found that veterans with PTSD prior to the COVID-19 pandemic were now managing their symptoms with more frequent alcohol and cannabis use. Another joint research endeavor between the two is examining the use of mindfulness smart phone apps to help reduce substance use in Operation Enduring Freedom/Operation Iraqi Freedom veterans with PTSD and alcohol use disorder. Where well-being and inequalities intersect Jungeun Olivia Lee also seeks to decode the network of relationships between socioeconomic status, adverse childhood experiences and drug use. Her experience as a social work practitioner working directly with clients drives her motivation to demonstrate to policymakers what she sees as a linkage between unemployment, economic stress and substance use disorders. She is lead author on a paper published in Nicotine & Tobacco Research that found unemployment may advance nicotine addiction among young adults, rather than the idea that nicotine addiction may lead to unemployment. Lee’s research interests lie at the intersection of substance use and co-occurring mental health, social inequalities (such as poverty and low socioeconomic status), and adverse childhood experiences. She is interested in combining these three areas of inquiry to explore their influence on addictive behavior that can persist over generations of at-risk families, such as adolescent mothers and their children. Her memories of working directly with clients struggling with the impact of addiction remain clear in her mind. When Lee hears policymakers and others suggest that individual willpower will solve substance use disorder problems, she has a straightforward response: “People are not born with addiction.” In her view, many factors contribute to the triggered distress, including socioeconomic status and adverse childhood experiences. Lee is exploring an idea with other IAS researchers to investigate the relationship between financial strain and employment uncertainty and addiction. “Individual circumstances, such as losing a job, certainly influence substance use, but policy-level decisions, such as the generosity of unemployment insurance, can mitigate the impact,” she said. Transdisciplinary collaboration with social scientists, psychologists and medical researchers at IAS and across the USC campus enriches and amplifies her work. “We are breaking down discipline-specific silos and bringing new and valuable perspectives to this work,” she said. “The synergy is both useful and inspiring.” Looking ahead Researchers also hope to spark interest in the field among the next generation. A new minor for undergraduate students in addiction science was introduced at USC in Fall 2020. The minor is an interdisciplinary collaboration of the Keck School of Medicine, the USC Suzanne Dworak-Peck School of Social Work, the USC School of Pharmacy and the USC Dornsife College of Letters, Arts, and Sciences. It is designed to provide students with a transdisciplinary approach to understanding and treatment of the broad spectrum of addiction-related problems. The goal of addiction science research and education is to improve the long-term effect of addiction treatment and save lives. As society’s understanding of the cause of addiction grows, researchers like those in the school of social work and the IAS strive to bridge the gap between science, practice and policy to positively impact outcomes for those affected by addiction.

Self-Built Protein Coatings Could Improve Biomedical Devices
Fouling is a natural phenomenon that describes the tendency of proteins in water to adhere to nearby surfaces. It’s what causes unwanted deposits of protein to form during some food production or on biomedical implants, causing them to fail. Using her expertise in developing bio-inspired materials for use in human health, R. Helen Zha, an assistant professor of chemical and biological engineering will harness this process found in nature to develop a versatile and accessible approach for modifying solid surfaces. With the support of a more than $592,000 National Science Foundation Faculty Early Career Development (CAREER) grant, Zha will use silk fibroin — a protein that naturally assembles itself — to grow a nanoscale film on the surface of an object. This approach only requires a beaker, water, salt, and the protein, which Zha said makes it biocompatible, safe, ecofriendly, and accessible beyond the walls of a lab. Zha has demonstrated that this approach can work and, in some cases, even increase the therapeutic benefits of an implant. In research published in ACS Biomaterials Science & Engineering, Zha collaborated with Ryan Gilbert, a professor of biomedical engineering at Rensselaer, to modify the surface of a fibrous scaffold that was developed by Gilbert’s lab in order to encourage the growth of neurites at the site of nerve damage. The importance of this research could expand beyond the protein Zha and her lab are working with. This approach, she explained, could be applied to any number of proteins and macromolecules.

New prostate cancer urine test shows how aggressive disease is and could reduce invasive biopsies
Researchers from the University of East Anglia have developed a new urine test for prostate cancer which also shows how aggressive the disease is. A new study shows how an experimental new test called ‘ExoGrail’ has the potential to revolutionise how patients with suspected prostate cancer are risk-assessed prior to an invasive biopsy. The research team say their new test could reduce the number of unnecessary prostate cancer biopsies by 35 per cent. Prostate cancer is the most common cancer in men in the UK. It usually develops slowly and the majority of cancers will not require treatment in a man’s lifetime. The most commonly used tests for prostate cancer include blood tests, a physical examination known as a digital rectal examination (DRE), an MRI scan or an invasive biopsy. However, doctors struggle to predict which tumours will become aggressive, making it hard to decide on treatment for many men. Lead researcher Dr Dan Brewer, from UEA’s Norwich Medical School, said: “While prostate cancer is responsible for a large proportion of all male cancer deaths, it is more commonly a disease men die with rather than from. “Therefore, there is a desperate need for improvements in diagnosing and predicting outcomes for prostate cancer patients to minimise over-diagnosis and overtreatment whilst appropriately treating men with aggressive disease, especially if this can be done without taking an invasive biopsy. “Invasive biopsies come at considerable economic, psychological and societal cost to patients and healthcare systems alike.” The research team developed the new ExoGrail urine test by combining two biomarker sources - measurements of a protein-marker called EN2 and the levels of gene expression of 10 genes related to prostate cancer risk. It builds on previously developed tests called PUR and ExoMeth. They tested it using urine samples from 207 patients who had been undergone a biopsy for prostate cancer at the Norfolk and Norwich University Hospital (NNUH). When the urine results were compared to biopsy results, the study showed that the test had successfully shown which patients had prostate cancer and which did not. The ExoGrail test also provided risk scores for patients and highlighted those for which an invasive biopsy would have been beneficial. The findings show that using information from multiple, non-invasive biomarker sources has the potential to greatly improve how patients with suspected prostate cancer are risk-assessed prior to an invasive biopsy. Dr Brewer said: “Our new urine test not only shows whether a patient has prostate cancer, but it importantly shows how aggressive the disease is. This allows patients and doctors to select the correct treatment. And it has the potential to reduce the number of unnecessary biopsies by 35 per cent.” The research team was led by Dr Shea Connell, Prof Colin Cooper, Dr Daniel Brewer and Dr Jeremy Clark, all from UEA’s Norwich Medical School, in collaboration with the Norfolk and Norwich University Hospital, the University of Surrey, the University of Bradford, The Earlham Institute, and The Movember GAP1 Urine Biomarker Consortium. The urine biomarker research was funded by the Movember GAP1 Urine Biomarker project, Prostate Cancer UK, The Masonic Charitable Foundation, The Bob Champion Cancer Trust, the King family, The Andy Ripley Memorial Fund, the Hargrave Foundation, Norfolk Freemasons and the Tesco Centenary Grant. Paul Villanti, executive director of programmes at Movember, said: “We are proud to have supported the development of the ExoGrail urine test as part of our Global Action Plan Urine Biomarker project. “Having non-invasive tests which can accurately show how aggressive a man’s prostate cancer is not only reduces the number of men having to undergo painful biopsies, but also ensures that the right course of treatment for the patient is selected more quickly.” ‘Integration of Urinary EN2 Protein & Cell-Free RNA Data in the Development of a Multivariable Risk Model for the Detection of Prostate Cancer Prior to Biopsy’ is published in the journal Cancers on Tuesday, April 27, 2021.

ChristianaCare also ranks as No. 1 overall employer for diversity and inclusion in Delaware, No. 14 among U.S. health systems (WILMINGTON, Del. – April 23) magazine ranked ChristianaCare as one of the best employers for diversity and inclusion in the United States in its list of Best Employers for Diversity 2021. ChristianaCare also ranked as the No. 1 employer for diversity in Delaware and the No. 14 health system for diversity in the nation. ChristianaCare ranked 121st out of the 500 employers that were recognized. “At ChristianaCare, our mission is simple, but profound – we take care of people,” said Janice Nevin, M.D., MPH, president and CEO of ChristianaCare, which is Delaware’s largest private employer. “And caring for people means that we work together, guided by our values of love and excellence, to bring equity and inclusion to everyone we serve, including our own caregivers. We are committed to building a workforce that reflects the diverse communities we serve, as we aspire to deliver high-quality, accessible care and achieve health equity.” ChristianaCare has committed to being an anti-racism organization and works to ensure that commitment is reflected through the organization’s policies, programs, and practices. (Read more about ChristianaCare’s anti-racism commitment here.) ChristianaCare’s inclusion efforts also include the launch of 10 employee resource groups, which connect caregivers who have a common interest or bond with one another. Formed by employees across all demographics – such as disability, gender, race, military status, national origin, sexual orientation, etc. – these voluntary grassroots groups work to improve inclusion and diversity at ChristianaCare. More than 750 caregivers at ChristianaCare participate in employee resource groups. ChristianaCare also recently launched LeadershipDNA, a new leadership development program that is specifically targeted to underrepresented, diverse populations and is designed to foster professional and career development. “We are grateful for this recognition, which affirms that our organization is committed to taking on the meaningful work to help our caregivers be exceptional today and even better tomorrow,” said Pamela Ridgeway, chief diversity officer and vice president of Inclusion and Diversity at ChristianaCare. “The fact that our caregivers can see the value and feel the impact of our inclusion and diversity efforts illustrates the importance for us to continue to push onward.” Forbes’ Best Employers for Diversity were identified from an independent survey of more than 50,000 U.S. employees working for companies employing at least 1,000 people in their U.S. operations. The employees were asked to give their opinion on a series of statements surrounding the topic of age, gender equality, ethnicity, disability, LGBTQ+, and general diversity concerning their own employer. The survey also gave survey participants the chance to evaluate other employers in their respective industries that stand out with regard to diversity. Only the recommendations of minority groups were considered. Also factored in was diversity engagement amongst managers and diversity among leadership. About ChristianaCare Headquartered in Wilmington, Delaware, ChristianaCare is one of the country’s most dynamic health care organizations, centered on improving health outcomes, making high-quality care more accessible and lowering health care costs. ChristianaCare includes an extensive network of primary care and outpatient services, home health care, urgent care centers, three hospitals (1,299 beds), a freestanding emergency department, a Level I trauma center and a Level III neonatal intensive care unit, a comprehensive stroke center and regional centers of excellence in heart and vascular care, cancer care and women’s health. It also includes the pioneering Gene Editing Institute. ChristianaCare is nationally recognized as a great place to work, rated by Forbes as the 5th best health system to work for in the United States and by IDG Computerworld as one of the nation’s Best Places to Work in IT. ChristianaCare is rated by HealthGrades as one of America’s 50 Best Hospitals and continually ranked among the nation’s best by U.S. News & World Report, Newsweek and other national quality ratings. ChristianaCare is a nonprofit teaching health system with more than 260 residents and fellows. With the unique CareVio™ data-powered care coordination service and a focus on population health and value-based care, ChristianaCare is shaping the future of health care. ####

Toolkit is easily incorporated into any laboratory science course Wilmington, Del., April 1, 2021 – St. Georges Technical High School in southern New Castle County, Delaware is the first high school in the United States to use ChristianaCare Gene Editing Institute’s innovative CRISPR in a Box Educational Toolkit™ in a science class. CRISPR in a Box brings to life the much-heralded CRISPR gene editing technology – the “genetic scissors” that allow scientists to edit DNA. The toolkit is designed for educational sessions in secondary and post-secondary schools and is suitable for remote learning. “Gene editing is the future of medicine,” said Eric Kmiec, Ph.D., director of ChristianaCare’s Gene Editing Institute. “Our partnership with the Delaware Department of Education will help cultivate the next generation of genetic scientists and enhance Delaware’s position as a leader in the biosciences.” “We are thrilled that students at St. Georges Technical High School will be the first In the United States to experience a live demonstration of CRISPR gene editing using our Innovative CRISPR in a Box educational toolkit,” said Siobhan Hawthorne, Education and Community Outreach leader at ChristianaCare’s Gene Editing Institute. “This toolkit will provide STEM students with a visual understanding of how the exciting CRISPR technology can unlock medical treatments to improve lives.” Delaware Secretary of Education Susan Bunting praised her department's partnership with ChristianaCare's Gene Editing Institute to develop the “Seeds of STEM” course that teaches high school students about gene editing. “Gene editing approaches diseases in new ways and will have significant impact in the health care and agriscience fields,” Bunting said. “This is a great example of an industry and education partnership investing in youth by providing hands-on knowledge and skills around emerging technology.” “We are so fortunate that ChristianaCare’s Gene Editing Institute reached out to our program to plan a high school ‘first’ opportunity with this new CRISPR experiment,” said Danya Espadas, one of the St. Georges biotech teachers. “Giving students the chance to use a cutting-edge, 21st century tool for medicine in their own high school lab – to have that technology at their fingertips – transcends what they see in a textbook or a video. By being able to do it themselves, it makes it real for them.” Espada said the experiment focuses on editing a gene of a non-infectious E.coli bacteria to become resistant to an antibiotic, thereby allowing researchers to create a new class of antibiotics that cannot be overcome by bacteria that are gene resistant. “We’re talking about eventually saving lives, here,” she said. “What can be more important than that?” The tools in CRISPR in a Box have been designed based on the pioneering discoveries of the Gene Editing Institute that are currently being used to explore next-generation medical therapies and diagnostics for diseases, including lung cancer and sickle-cell anemia. Component items in the toolkit include the CRISPR/Cas complex, a target DNA molecule, a mammalian cell free extract and a synthetic DNA molecule. All materials in the kit are safe, synthetic materials. There are no live cultures or viruses involved. The kit is meant to provide a hands-on demonstration of CRISPR’s capabilities, and not allow for manipulations of living organisms. “The kit is easy and fun to use,” said Kristen Pisarcik, research assistant at the Gene Editing Institute who has taught students at Delaware Technical Community College which first used the toolkit. “In a short period of time students will reliably and successfully complete the laboratory activity and be able to see the results of gene editing,” she said. Since the foundations of the kit touch upon key themes in biology, it can be readily incorporated into practically any science or biology course with a laboratory component, “One of the beauties of CRISPR in a Box is that there is no need to purchase specialized equipment. If a teaching lab can support bacterial cultivation, it can perform the in vitro gene editing lab activity,” Pisarcik said. CRISPR in a Box is the evolution of a partnership between the Gene Editing Institute, Delaware Technical Community College and Rockland Immunochemicals that began in 2017 with a National Science Foundation grant to develop the first-ever gene editing curriculum for community college students. Video and photo collection of first class in U.S. to use CRISPR in a Box™ educational gene editing toolkit. About ChristianaCare’s Gene Editing Institute The Gene Editing Institute, a worldwide leader in CRISPR gene editing technology and the only institute of its kind based within a community health care system, takes a patient-first approach in all its research to improve the lives of people with life-threatening disease. Since 2015, researchers at the Gene Editing Institute have been involved in several ground-breaking firsts in the field, including the development of the first CRISPR gene editing tool to allow DNA repairs outside the human cell which will rapidly speed therapies to patients and a unique version of CRISPR called EXACT that reduces the number of off-target edits to other areas of the genome, which is vital for further research and patient applications. Its researchers are currently developing a patient trial for lung cancer using CRISPR and employing the technology to combat the COVID-19 pandemic. About the biotech program St. Georges Technical High School The Biotech career program of study at St. Georges Technical High School is the first such program offered in a Delaware high school. With two teachers and approximately 100 students in grades 10-12, the program presents advanced content in biology and chemistry with opportunities for students to learn basic laboratory techniques and procedures and to maintain and operate common instruments and equipment used in a biotechnology laboratory. St. Georges is a comprehensive career and technical high school with 1,100 students who study in one of 16 different career pathways.
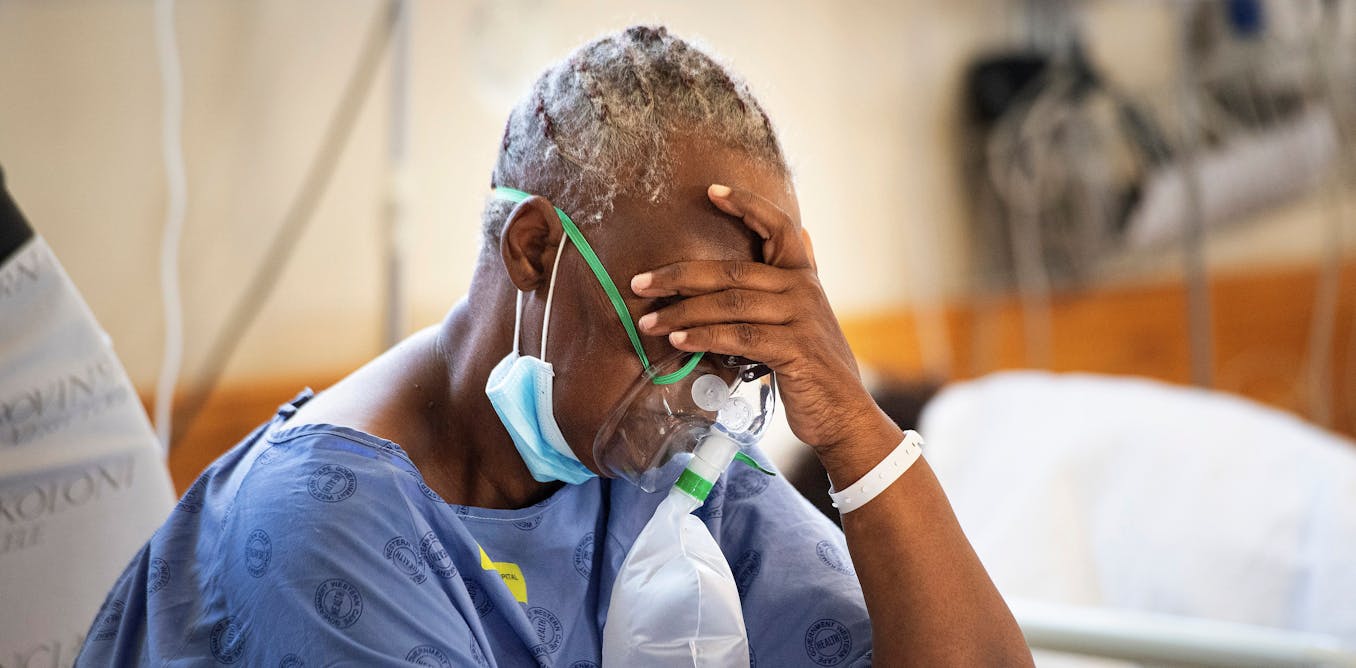
How worried should you be about coronavirus variants? A virologist explains his concerns
Paulo Verardi, Associate Professor of Virology and Vaccinology at UConn, was asked to lend his expertise and opinion to The Conversation about coronavirus variants and just how concerned Americans should be about the emergence of variants and the speed at which they are spreading across the country and the globe. Spring has sprung, and there is a sense of relief in the air. After one year of lockdowns and social distancing, more than 171 million COVID-19 vaccine doses have been administered in the U.S. and about 19.4% of the population is fully vaccinated. But there is something else in the air: ominous SARS-CoV-2 variants. I am a virologist and vaccinologist, which means that I spend my days studying viruses and designing and testing vaccine strategies against viral diseases. In the case of SARS-CoV-2, this work has taken on greater urgency. We humans are in a race to become immune against this cagey virus, whose ability to mutate and adapt seems to be a step ahead of our capacity to gain herd immunity. Because of the variants that are emerging, it could be a race to the wire. April 08 - The Conversation Dr. Verardi discusses the the five SARS-CoV-2 variants we all need to be watching, the rates of transmission and the severity of symptoms, and why we all need to remain on guard and get vaccinated. It is a great article, and if you are a journalist looking to cover this topic, then let us help with your stories. Dr. Paulo Verardi is a virologist who specializes in vaccine research and development and is a member of the Center of Excellence for Vaccine Research. Dr. Verardi is available to speak with media regarding variants and COVID-19 – simply click on his icon now to arrange an interview today.

UConn Researcher Develops Successful Zika Virus Vaccine in Preclinical Studies
UConn researcher Paulo Verardi, associate professor of pathobiology and veterinary science in the College of Agriculture, Health and Natural Resources, has demonstrated the success of a vaccine against Zika virus and recently published his findings in Scientific Reports, a Nature Research publication. He has also filed provisional patents with UConn’s Technology Commercialization Services for the novel vaccine platform technology used to generate the vaccine, as well as genetic modifications made to the vaccine that significantly enhance expression of the vaccine antigen. Verardi, a Brazilian native, was in Brazil visiting family in the summer of 2015 when the Zika outbreak first began to make waves and soon reached epidemic status. Back in the United States, Verardi kept tabs on the Zika epidemic and its emerging connection to microcephaly, a serious birth defect that causes babies to be born with small heads and underdeveloped brains. In October of that year, Verardi called then-Ph.D.-student Brittany Jasperse (CAHNR ‘19) into his office and told her he wanted to apply their newly developed vaccine platform and start developing a vaccine for Zika virus. It’s an impressive achievement and there’s a full article attached for those looking to know more. Verardi emphasizes that developing vaccines for viruses, in this case Zika, help the world be better prepared for outbreaks of novel and emerging viruses by having vaccine development frameworks in place. “Emerging viruses are not going to stop popping up any time soon, so we need to be prepared,” Verardi says. “Part of being prepared is to continue the development of these platforms.” If you’re a journalist looking to know more about Zika virus and this emerging news about a vaccine – then let us help. Dr. Paulo Verardi is a virologist who specializes in vaccine research and development. He is an Associate Professor at UConn and a member of the Center of Excellence for Vaccine Research. Dr. Verardi is available to speak with media regarding this emerging development – simply click on his icon now to arrange an interview today.

What Can A Forgotten Piece of Our Opioid Addiction and Treatment History Teach Us?
As the nation struggles with the third wave of a continuing opioid epidemic, a newly republished book co-authored by Nancy Campbell, the head of the Department of Science and Technology Studies at Rensselaer Polytechnic Institute, offers insight into present-day drug addiction and treatment by exploring a complex chapter from the nation’s past. Written with JP Olsen and Luke Walden, The Narcotic Farm: The Rise and Fall of America’s First Prison for Drug Addicts details the history of the United States Narcotic Farm, a federal institution that opened in 1935 outside of Lexington, Kentucky. Jointly operated from 1935 to 1975 by the U.S. Public Health Service and the Federal Bureau of Prisons, the Narcotic Farm was a combination prison, hospital, working farm, rehabilitation center, and research laboratory. “All of our scientific knowledge about human opioid addiction comes from that time, comes from that place,” said Campbell, a leading figure in the social history of drugs, drug policy, and harm reduction, on an episode of the Landmark Recovery Radio podcast. The facility, which was also the subject of a 2009 documentary featuring Campbell, has a complicated legacy. It revolutionized treatment methods commonly accepted today, such as using methadone to medically manage heroin detox and the development of drugs like naloxone and buprenorphine. But it fell under a cloud of suspicion in 1975, when Congress learned that researchers had recruited patients as test subjects for CIA-funded LSD experiments as part of the notorious MK-Ultra project. “With the ongoing opioid epidemic worsening this past year in the midst of the COVID-19 pandemic, the lessons learned in this book continue to be relevant today,” Campbell said. Campbell is also the author of Using Women: Gender, Drug Policy, and Social Justice and Discovering Addiction: The Science and Politics of Substance Abuse Research, as well as the co-author of Gendering Addiction: The Politics of Drug Treatment in a Neurochemical World. Her most recent book, OD: Naloxone and the Politics of Overdose, was published in 2020. “Nobody should die of overdose. A high overdose death rate signals that we have not cared for the people who have been hurt most by the war on drugs, first pursued by President Dwight D. Eisenhower in 1954,” Campbell said in a recent “Academic Minute” segment. Campbell is available to discuss a wide range of topics relating to drug policy and history, including the Narcotic Farm.





