Experts Matter. Find Yours.
Connect for media, speaking, professional opportunities & more.

Could Vitamin-A bring back your sense of smell after Covid?
Researchers at the University of East Anglia and James Paget University Hospital are launching a new project to see whether Vitamin A could help people regain their sense of smell after viral infections including Covid-19. Smell loss is a common symptom of Covid-19, but even before Covid, many viruses had been causing smell loss and distortion and while most people naturally regain their sense of smell within a couple of weeks, many have been left with on-going smell disorders. Previous research from Germany has shown the potential benefit of Vitamin-A, and the UEA team will explore how this treatment works to help repair tissues in the nose damaged by viruses. They hope that the study, which has been funded by the National Institute for Health Research (NIHR), could one-day help improve the lives of millions around the world who suffer from smell loss, by returning their fifth sense. Smell loss expert Prof Carl Philpott from UEA’s Norwich Medical School and James Paget University Hospitals NHS Trust, said: “The huge rise in smell loss caused by Covid-19 has created an unprecedented worldwide demand for treatment. “Even before the Covid-19 pandemic hit, smell loss was thought to affect an estimated five per cent of people, with viruses accounting for 1 in 10 of those. “And around one in ten people who experience smell loss as a result of Covid-19 report that their sense of smell has not returned to normal four weeks after falling ill. “It’s a big problem, and our previous research has shown the impact of smell loss – including depression, anxiety and isolation, as well as risk of danger from hazards such as gas and spoiled food, and changes in weight due to reduced appetite. “A key problem for patients and their clinicians is the lack of proven effective treatments. “A recent study from Germany showed that people treated with vitamin A nasal drops improved twice as much as those in the untreated group. “We want to find out whether there is an increase in the size and activity of damaged smell pathways in patients’ brains when they are treated with vitamin A nasal drops. “This would show recovery of the damage caused by common viral infections, including Covid-19, in the nose.” The research team will work with patients who have lost their sense of smell due to a viral infection. They will either receive a 12-week course of nasal vitamin A drops or inactive equivalent drops, and have their brains scanned before and after the treatment. The scans will be compared to those of a control group who have not been treated with vitamin A drops. Prof Philpott said: “The patients will be smelling distinctive odours - roses and rotten eggs - while special MRI brain scans are taken. “We will look for changes in the size of the olfactory bulb - an area above the nose where the smell nerves join together and connect to the brain. “We will also look at activity in areas of the brain linked to recognising smells,” he added. Duncan Boak, Founder and Chair of Fifth Sense, said: “At Fifth Sense we have engaged with thousands of people who have experienced changes in their ability to smell or taste as a result of the Covid 19 virus. They join an already large community of people with a smell disorder that pre-dates the pandemic. “The question we are most often asked is about available treatments to support recovery. Not being able to smell is not only physically distressing but can affect the enjoyment of social occasions and present hazards and risks that might never have been previously considered such as not being able to detect gas leaks or spoiled food. “Research into potentially successful interventions is vital to help people feeling the impact of smell disorders that affects the quality and enjoyment of their life.” To take part in this trial, patients need to be referred to The Smell and Taste Clinic at the James Paget University Hospital by their GP. Recruitment is expected to begin in December 2021. To find out more visit https://rhinology-group.uea.ac.uk/apollo-trial or contact apollo.trial@uea.ac.uk. The NIHR is the largest funder of research in the country, and is the research partner of the NHS and social care. To find out more about other NIHR research happening near you, visit www.bepartofresearch.uk.

A missed opportunity - hospital doctors must stop 'risky' medicines
Hospital doctors and pharmacists should stop ‘risky’ medicines before patients leave hospital - according to researchers at the University of East Anglia. One in two older people are prescribed a medicine which over time has become inappropriate or unnecessary. In a recent National Overprescribing Review titled ‘Good for you, good for us, good for everybody’, the government called on doctors and pharmacists working in GP surgeries to tackle the problem of overprescribing. But research from UEA’s School of Pharmacy has found that nine out of 10 older hospital patients and their family believe that inappropriate or unnecessary medicines should also be spotted and stopped whilst they are in hospital. And the team say that by the time people are back under their GP care, a major opportunity has been missed. Prof Debi Bhattacharya, from UEA’s School of Pharmacy, said: “We know that half of older people admitted to hospital arrive having been prescribed a medicine that over time has become inappropriate for them. These medicines will have more risks than benefits. “And their side effects cause problems, like making them feel drowsy, nauseous or have trouble getting to sleep. These problems impact a person’s quality of life to the extent that they can cause re-hospitalisation. “Our research has shown that very few patients have one of these ‘risky’ medicines stopped whilst in hospital. “Continuing medicines when they are not needed unnecessarily harms people and wastes NHS money. “The time is right to undertake research into ways of safely increasing the number of inappropriate and unnecessary medicines that are stopped,” she added. To tackle the problem, Prof Bhattacharya is leading a £2.4 million trial to stop risky medicines in hospital - in collaboration with researchers at the Universities of York, Newcastle, Leeds and Leicester, the Norfolk and Norwich University Hospital and Addenbrooke’s Hospital in Cambridge. Patient and Public Engagement lead for CHARMER, Katherine Murphy, said: “We are working with hospitals and GP organisations across England to see whether the new strategy works, helps people, causes no harm, and is good value for the NHS. “And for this trial to be meaningful to people, we need to make sure that we look at the things that matter to them when testing whether stopping a medicine has had a positive outcome.” The research team recently surveyed 200 people including patients, informal carers, doctors, nurses, pharmacists, physiotherapists and researchers to find out what they should look at in the trial. On reviewing the results Katherine Murphy said: “It was good to see that what people really want us to look at is whether patients can do the things that they want to do, not how much patients can do. “Being able to walk up a flight of stairs, for example, may be important to some patients but not to others. We need to make sure that medicines are prescribed that support people to get the best quality of life. In the trial, we also need to make sure that the way that we stop risky medicines causes no harm and is good value for the NHS.” For more information about the CHARMER study visit https://www.uea.ac.uk/web/groups-and-centres/charmer/about-the-research The research has been funded by the National Institute of Health and Social Care research.
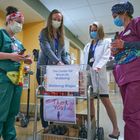
ChristianaCare recognized by American Medical Association with 2021 Joy in Medicine distinction
ChristianaCare one of only 44 nationwide to receive the distinction; one of only five to receive the highest level – Gold Recognition (WILMINGTON, Del. – Oct. 7, 2021) ChristianaCare has been named a recipient of the American Medical Association’s Joy in MedicineTM Health System Recognition Program. The distinction recognizes health systems that demonstrate a commitment to preserving the wellbeing of health care team members by engaging in proven efforts to combat work-related stress and burnout. The American Medical Association awarded ChristianaCare a “Gold Recognition” – the highest level within the program. Only 44 health systems nationwide received the Joy in Medicine distinction, with only four other health systems along with ChristianaCare achieving the Gold Recognition. “When caregivers feel supported and fulfilled in their work, the quality of both their experience and their patient’s experience improves,” said Heather Farley, M.D., MHCDS, chief wellness officer and head of ChristianaCare’s Center for WorkLife Wellbeing. “That’s why, when the COVID-19 pandemic struck, we deepened our investment of resources to support our caregivers. While there’s still a long way to go, we are grateful to receive this recognition as it affirms our commitment to helping our caregivers foster meaning, connection and joy in work and in life.” ChristianaCare received the “Gold Recognition” for achieving six criteria: An organization-wide commitment to improving physician wellbeing. An assessment of the costs of physician burnout. Evidence-based interventions to reduce and eliminate burnout. Leadership commitment to address areas for improvement. Interventions to improve teamwork. Structured programs that actively engage doctors to cultivate community at work. These criteria align with ChristianaCare’s commitment to support its caregivers in alignment with the organization’s core values of love and excellence. ChristianaCare has implemented structured ways of working that encourages leaders to create environments where their workers feel safe asking questions and feel empowered to identify and solve problems. ChristianaCare also uses numerous surveys and assessments to track progress in improving the wellbeing and experience of caregivers. ChristianaCare’s Unique Center for WorkLife Wellbeing ChristianaCare established the Center for WorkLife Wellbeing in 2016 to develop support systems to enable clinicians to reconnect with the joy and meaning in medicine. “We recognized the growing problem of stress and burnout in health care, and we made a decision to tackle it head-on,” said Janice E. Nevin, M.D., MPH, ChristianaCare president and CEO. “The work of our psychologists, researchers, clinicians and peer supporters in the Center for WorkLife Wellbeing is built on the understanding that when we care for ourselves, we are better able to care for others, resulting in decreased medical errors and a better experience of care for everyone involved.” The Center soon expanded its mission to support all of ChristianaCare’s caregivers, including those who don’t work in clinical roles. The Center also has received national recognition for its expertise and leadership in the field of workplace wellbeing. Throughout the pandemic, the Center for WorkLife Wellbeing has proactively shared a variety of resources to support caregivers as they work to provide safe, effective care and reduce the spread of COVID-19. This includes: The Care for the Caregiver program, which provides confidential individual peer support and group support to caregivers when they experience stress related to patient care or the workplace. Peer supporters and organizational leaders receive training so they can provide psychological first aid to caregivers whom they recognize are struggling as well as connect them to helpful resources if needed. Emotional support through mindfulness resources and regular rounds where the Center’s experts can check on staff wellbeing. OASIS Rooms, which are quiet sanctuaries inside the hospital where caregivers can go to take a break, de-stress, meditate or enjoy a chair massage. 24/7 mental health services and programs to help caregivers maintain healthy habits including proper exercise, sleep and nutrition. Fitness centers that are free for all caregivers to use and provide easy access to exercise and fitness programs. “I always use the analogy, you can’t take the canary out of the coal mine and teach it to be more resilient and then put it back in the same coal mine and expect it to survive,” Dr. Farley said. “You actually have to change the coal mine – the environment surrounding our caregivers and clinicians. That’s what we’re doing in the Center for WorkLife Wellbeing.” Solutions to a National Problem A national study examining the experiences of physicians and other health care workers who worked in health systems during the COVID-19 pandemic found that 38% self-reported experiencing anxiety or depression, while 43% suffered from work overload and 49% had burnout. “The COVID-19 pandemic has placed extraordinary stress on physicians and other health care professionals,” said American Medical Association President Gerald E. Harmon, M.D. “While it is always important for health systems to focus on the wellbeing of care teams, the imperative is greater than ever as acute stress from combatting the COVID-19 pandemic has contributed to higher rates of work overload, anxiety and depression. The health systems we recognize today are true leaders in promoting an organizational response that makes a difference in the lives of the health care workforce.” Launched in 2019, the Joy in Medicine Health System Recognition Program is a component of the American Medical Association’s practice transformation efforts, an ambitious initiative to advance evidence-based solutions to address the physician burnout crisis. Candidates for the program were evaluated according to their documented efforts to reduce work-related burnout through system-level drivers. Scoring criteria were based on demonstrated competencies in commitment, assessment, leadership, efficiency of practice environment, teamwork and support. About ChristianaCare Headquartered in Wilmington, Delaware, ChristianaCare is one of the country’s most dynamic health care organizations, centered on improving health outcomes, making high-quality care more accessible and lowering health care costs. ChristianaCare includes an extensive network of primary care and outpatient services, home health care, urgent care centers, three hospitals (1,299 beds), a freestanding emergency department, a Level I trauma center and a Level III neonatal intensive care unit, a comprehensive stroke center and regional centers of excellence in heart and vascular care, cancer care and women’s health. It also includes the pioneering Gene Editing Institute. ChristianaCare is nationally recognized as a great place to work, rated by Forbes as the 5th best health system to work for in the United States and by IDG Computerworld as one of the nation’s Best Places to Work in IT. ChristianaCare is rated by HealthGrades as one of America’s 50 Best Hospitals and continually ranked among the nation’s best by Newsweek and other national quality ratings. ChristianaCare is a nonprofit teaching health system with more than 260 residents and fellows. With its groundbreaking Center for Virtual Health and a focus on population health and value-based care, ChristianaCare is shaping the future of health care. #####

It is in the news daily the awareness campaigns are everywhere – but for Spanish-speaking Americans, a lot of the information on COVID-19 and vaccination efforts against the disease weren’t reaching home. That was leaving a large swath of the population unprotected against the virus. Pastor Angel Maestre takes to the airwaves for his radio show, 97 Oasis, each week, speaking about faith to his Spanish-speaking audience. When COVID-19 vaccines rolled out, he began including teachings about health and science. “It was my duty as a leader,” Maestre says. Vaccination rates among the Hispanic population were extremely low at the time. In Richmond County, less than 10 percent of this community was vaccinated. Maestre partnered with Dr. Jose Vaszquez, an infectious diseases physician at Augusta University Health. Vazquez began appearing on Maestre’s radio show. He also spoke and answered questions at Maestre’s church, Centro Cristiano Oasis de Bendicion. “The Hispanic community has been one of the toughest communities to get vaccinated,” Vasquez says. “They’re not anti-vaxxers. But, most of the education put out there is in English. A lot of it is not in Spanish. So, they didn’t understand.” According to Vazquez, the top three concerns among the Hispanic community were that the COVID-19 vaccine contained fetal tissue, caused infertility and could result in undocumented immigrants encountering problems with immigration authorities. “They thought if we took their name and number, that ICE or immigration would come and take them, which is not true.” Vazquez eased concerns, and vaccination rates increased quickly. “I’m proud to say because of our outreach programs with some of our partners, specifically going through the churches, that it has actually increased to 30 to 35 percent.” Are you a journalist looking to know more about how COVID-19 is impacting Hispanic communities and what else can be done to ensure every person in America has access to vaccines? That’s where Augusta University can help. Dr. Jose Vazquez, division chief and professor of medicine in the Medical College of Georgia, is an expert in the realm of infectious diseases. He studies and treats infectious diseases, including antibiotic-resistant superbugs and fungal infections. He has been a reliable source for local, statewide and national media regarding the coronavirus outbreak. Dr. Vazquez is available to speak with media regarding this topic – simply click on his icon to arrange an interview.

Social media ‘likes’ found to positively influence healthy food choices – new research
Social media users who view images of healthy foods that have been heavily endorsed with ‘likes’ are more likely to make healthier food choices, a new study has found. The research, by psychologists from Aston University’s College of Health and Life Sciences, found that study participants who viewed highly liked mock Instagram posts of fruit and vegetables ate a significantly higher proportion of grapes than cookies, with consumption of grapes increasing by 14 per cent more calories, compared to those who viewed highly liked high calorie foods. The study, which is published in the scientific journal Appetite, investigated the acute effect of socially endorsed social media posts on participants’ eating behaviour. The 169 participants, who had an average age of 21 years old (but total ages across the group ranged from 18 to 48), were asked to look at mock Instagram posts of different types of food, that either had a few or a lot of ‘likes’, and later given access to grapes and cookies to consume. As well as viewing images of fruit and vegetables, participants also looked at less nutritious foods such as cakes and biscuits, and non-food images such as stylish interior designs. However, the researchers found that the participants went on to consume a larger proportion of grapes after viewing highly liked images of fruit and vegetables, compared to the other images. Aston University psychology PhD student Lily Hawkins, who led the study alongside supervisor Dr Jason Thomas, said: “The findings of the study suggest that not only exposure to healthy food images on social media, but those that are also heavily endorsed with ‘likes’, may nudge people to choose to eat more healthy foods, in place of less nutritious foods.” “What we see others approve of eating and post about eating on social media can affect our actual eating behaviour and could result in a greater consumption of healthier meals and snacks.” “One reason for this may be because thinking that others ‘like’ and eat fruit and vegetables nudges participants to alter their behaviour in order to fit in with what they perceive to be the norm.” The most recent figures from the NHS’s Health Survey for England showed that in 2018 only 28 per cent of adults were eating the recommended five portions of fruit and vegetables per day. In Wales, this was 24 per cent, in Scotland 22 per cent and in Northern Ireland around 20 per cent. Children and young people across the UK had even lower levels of fruit and vegetable consumption. The study findings suggest that social media could be used in future as a way to encourage healthier eating - by encouraging users to follow more social media accounts which have highly liked nutritionally balanced posts, also containing healthier foods. The researchers said the next stage of their work will trial an intervention using real Instagram accounts, to test whether asking people to actively follow more social media accounts posting images of highly liked nutritionally rich foods, can encourage people to consume more fruit and vegetables over a sustained period of time. Professor Claire Farrow, Director of Aston University’s Applied Health Research Group, whose work has contributed to the national Child Feeding Guide resource, added: “We know that social interactions can strongly shape what, when and how much we eat. These findings highlight the important role that social media has in shaping those influences online.” “The findings suggest that people do not simply passively view information about what other people are eating online, but that this digital information can shape our food preferences and choices, particularly when we think lots of other people like certain foods. It is promising that exposure to healthy foods, and likes of those foods, was related to greater intake of healthy foods.” “Further research is needed to explore whether and how these findings can be translated into digital interventions to help support individuals who want to make healthier food choices, and to understand how social media platforms can be used as a tool to support healthy eating behaviour.”
Experts in the Media – UConn’s Dr. David Banach is the go-to voice on COVID boosters
As COVID continues to wreak havoc across the globe, health systems in America are overwhelmed. And as the debate about a third shot continues, the FDA is prepared to allow Pfizer vaccine boosters as early as this week to those over 65 and to people at a higher health risk if exposed to the virus. UConn epidemiologist Dr. David Banach offered his expert perspective and insight on the need and effectiveness for those looking to learn more about booster shots and COVID vaccines: Booster shots of Pfizer’s COVID-19 vaccine may be administered as early as Friday, but who will get one is still up for discussion. “What the FDA review showed was in the general population, at this date and time, there wasn’t sufficient data to support booster doses,” said Dr. David Banach, hospital epidemiologist at UConn Health. Last week, the FDA’s advisory committee voted overwhelmingly not to recommend a third shot for people 16 and up. However, they did vote to authorize a booster dose at least six months after full vaccination for people who are 65 and older as well as individuals who are at high risk for severe COVID. “In older populations, there seems to be some potential benefit to giving a third dose within the Pfizer group,” said Dr. Banach. Dr. Banach said more information is expected in the days to come as this matter heads to the CDC’s independent advisory panel this week. “It’s going to provide more granular recommendations on how to proceed with that 65 and older group and potentially other groups as well,” said Dr. Banach. He added one of the groups up for discussion is healthcare workers. There continues to be an enormous amount of coverage and questions about vaccines and COVID-19, and if you are a journalist looking to know more and include an expert in your story, then let us help. Dr. David Banach is one of the lead experts on COVID-19 in America. He is available to speak with media regarding vaccination and what the future holds with COVID-19. To book an interview, simply click on his icon today.

Children Face Type 2 Diabetes Health Concerns After a Year at Home
Some children are facing health concerns after a year of attending school online. During the pandemic, research found cases of type 2 diabetes among children more than doubled. Lisa Diewald, MS, RD, LDN, Program Manager for the MacDonald Center for Obesity and Education weighed in on causes and potential prevention methods going forward. “We know that physical activity level, eating habits, weight status and other lifestyle factors play a significant role in the development of type 2 diabetes in adults and in children,” said Diewald. “Because of disruptions for many children in all four factors during the pandemic, (on top of pre-existing challenges), we are starting to see trickle-down health effects involving lifestyle-related chronic diseases, such as type 2 diabetes and children are not immune to these health effects.” Type 2 diabetes is related to obesity, exercise habits and diet. Children who struggle with weight may also have many social, genetic and environmental factors impacted by the accelerated risk seen through the pandemic. For example, the absence of healthy school meals while learning from home negatively impacted some children, as processed foods became replacements. Eating habits are also largely impacted by one’s mental state. “Like adults, children learn to cope with stress and anxiety in different ways. For some, this means reaching for comfort foods, which are often high in refined carbohydrates, saturated fat and sugar-all risk factors for T2 diabetes if consumed in excess,” said Diewald. “These foods can contribute to unhealthy weight gain, especially when physical activity is limited as well. The bad news is that it does not take a lot of weight gain to put a child who is already at risk at greater risk for diabetes.” But families should be aware of the good news that small changes can make a big difference and that prevention is possible. Diewald recommends a few small changes to alter a sedentary routine for parents and schools: • Build 1 minute brain breaks during the day for activity such as stretching or running up and down the stairs • Keep healthy snacks available and sugar sweetened snacks and drinks less visible • Create safe and walkable opportunities for children to add physical activity • Look for outdoor community sponsored activities that encourage physical activity that can provide safe and accessible physical activity opportunities Additional measures for parents to prevent the unhealthy coping with foods including working with children to make a list of fun alternative activities (unrelated to food) to do when boredom kicks in and posting in an accessible place in the home. Parents can act as role models and let children see that parents are working on more effective ways to cope as well. Though the risk of type 2 diabetes has been increasing during the past year, many factors can continually increase a person’s risk. These tips can provide the valuable tools for prevention in the future. “Teaching children healthier ways to cope with boredom and depression than eating are skills that can help for a lifetime, well beyond the pandemic,” said Diewald. To speak with Diewald, email mediaexperts@villanova.edu.

Anti-mask ordinances amount to disability discrimination
University of Rochester health policy expert Mical Raz says anti-mask ordinances amount to disability discrimination for individuals with compromised immune systems—that includes people who have cancer and autoimmune disease, as well as those who have received organ transplants. As Dr. Raz explained in a recent Washington Post essay, immunocompromised individuals—even those who are vaccinated—may now find themselves inadequately protected in workplaces where mask requirements are legally banned and there are no vaccine requirements. Dr. Raz also co-authored a piece in the JAMA Health Forum discussing the implications of some states banning attempts to mandate masking. As she points out, vaccines have been less effective in individuals with different categories of immunosuppression. Dr. Raz concludes that allowing mask requirements is an important form of disability accommodation.

UCI scholars discuss how 9/11 changed America
In recognition of the 20th anniversary of the Sept. 11, 2001, terrorist attacks in the U.S., we asked UCI scholars a single question: How did 9/11 change America? They responded according to their expertise – which ranges from collective trauma, media, air travel, foreign relations, false narratives, political divisiveness, and the war on terror. Contact Tom Vasich at 949-285-6455, tmvasich@uci.edu, to arrange interviews. Roxane Cohen Silver, Distinguished Professor of psychological science, public health and medicine E. Alison Holman, professor of nursing Topic: Media and collective trauma Quote: “The Sept. 11 terrorist attacks – which hijacked our television screens that Tuesday morning as people who sought to do us harm hijacked four airplanes – captured people’s attention throughout the days and weeks that followed. It also ushered in 24/7 media attention to what has become known as a “collective trauma,” transmitting the horrible events of that day throughout the country and, indeed, throughout the world in a matter of seconds. …The 9/11 attacks were tragic for American residents, but they also taught us that the media can broadcast distress alongside the news it’s covering.” Jan K. Brueckner, Distinguished Professor of economics Topic: Air travel Quote: “In response to the revenue shock of 9/11 and to new competition from low-cost carriers, the major airlines behaved conservatively in adding back capacity as traffic returned, so that the carriers eventually offered fewer seats to an ultimately larger number of passengers, leading to fuller flights and today’s less comfortable flying experience. Even though 9/11 is long past, the airline industry continues to operate in a climate of fear of terrorism from the air.” Erin Lockwood, assistant professor of political science Topic: U.S. foreign policy Quote: “The attacks – and the U.S. response – set in motion decades of war, anti-Arab and anti-Islamic bias and violence, and a willingness to sacrifice military and civilian lives and civil liberties for the perception of security. As we mark the withdrawal of U.S. forces from Afghanistan this month, it’s all too apparent that many of those trends continue to reverberate today.” David Kaye, clinical professor of law Topic: National security Quote: “Despite my hopes for something better that might emerge, the attacks reinforced a cult of national security that the United States transformed into the torture of terrorism suspects, drone warfare, the invasion of Iraq, Guantanamo Bay’s indefinite detentions, anti-Muslim discrimination at home and the emergence of the contemporary surveillance state. … The predominance of national security as an ideology and apologia remains among the most significant legacies of that day, a feature of American political life that continues to constrain creativity and a return to normalcy in American law and policy.” Matthew Beckmann, associate professor of political science Topic: War on terror Quote: “To understand the legacy of 9/11 is to define the legacy of George W. Bush. For after the deadliest terrorist attacks on U.S. soil in our nation’s history, American citizens and lawmakers gave President Bush broad support and broader authority to wage the “war on terror” as he saw fit. … Twenty years after the attacks, having seen those lofty aspirations dashed in Afghanistan and Iraq, disregarded in Guantanamo Bay and black site prisons, and discounted even by our staunchest allies, the biggest legacy of Sept. 11 for the United States is that the “shining city on a hill” has less luster and a shorter reach.” David Theo Goldberg, professor of comparative literature Topic: Rise of false narratives Quote: “The events of 9/11 lent themselves to make-believe. The smoke hadn’t yet cleared when conspiracies began to abound, from “weapons of mass destruction” to “the deep state.” That the Trump administration adopted this as its own playbook while insisting on “draining the swamp” required cooking the rules. … Fabrication had become the rule book of the game. Invention and inventedness, disruption and innovation fueled the movement. The “truth” was, well, oh so yesterday.”

Type 2 diabetes: why treatment plans may need to be different for older adults
Around 6% of the world’s population suffer from type 2 diabetes. People of any age can develop the condition, but the number of older adults with type 2 diabetes is rapidly increasing worldwide. In fact, adults over the age of 65 now account for almost half of all adult cases. There are many ways type 2 diabetes can be managed – including controlling weight through diet and exercise, or taking a drug to manage blood sugar levels. But many people may not realise that type 2 diabetes in older adults can be more complicated to manage. This means people over 65 may need to be managed differently when it comes to type 2 diabetes. There are a number of reasons why type 2 diabetes may be more difficult to manage in older adults. First, ageing can affect blood sugar control, as the body’s organs (such as the pancreas, which controls insulin and blood sugar levels) lose their ability to work as well as they used to. On top of this, some research has shown that diabetes may cause people to age faster. It’s thought that this is due to high levels of sugar in the blood stream prematurely ageing the body’s cells. This premature ageing could lead to diseases associated with age-related decline (such as arthritis or dementia) happening sooner. Frailty – a state of health that is associated with reduced physical and mental resilience in older adults – also affects more people with type 2 diabetes than the rest of the population. In fact, an estimated 25% of older adults with type 2 diabetes are also frail. People who are frail and have type 2 diabetes have poorer health and increased risk of death from all causes compared to those who are not frail. Frailty is associated with reduced physical and cognitive functions and increased risk of low blood sugar. Both of these factors can make treating type 2 diabetes more complicated. Dementia, which is more common in older adults, may also make it more difficult to manage type 2 diabetes. This is because the memory problems this condition causes may make it harder for patients to remember to take their medication, or take the proper medication dosage. What’s more, type 2 diabetes in older adults is actually a risk factor for developing dementia – including Alzheimer’s disease. While the link between the two isn’t fully understood, elevated blood sugar levels and insulin not working properly have been suggested as causes. Having other health conditions can also make it more difficult to treat diabetes. Up to 40% of older adults with type 2 diabetes have four or more co-existing diseases – such as heart disease or dementia. These conditions can make it impossible to achieve normal treatment targets and the drugs used to treat them can interact with those used to treat diabetes – which could lead to harm if not managed carefully. Alongside this, poor access to proper medical care, and being more susceptible to low blood sugar in older age are also reasons why treating diabetes can be so difficult in this age group. Managing type 2 diabetes Most medical treatments for type 2 diabetes work to keep blood sugar levels low, and prevent them from spiking. But older adults with type 2 diabetes may actually have an increased risk of developing dangerously low blood sugar levels. This usually happens if the medication is not used at the correct dose, or in people who have had diabetes for a long time. Older adults can also be susceptible to low blood sugar levels. Syda Productions/ Shutterstock Having very low blood sugar levels is dangerous as it can increase the risk of falls – a serious and sometimes life-threatening problem in older adults. Very low blood sugar levels also increase the risk of heart problems. This means that healthcare professionals need to be careful they aren’t being too aggressive in treatment plans for older adults to avoid causing other health problems. Ageing may also alter the body’s response to low blood sugar. This is significant, as when blood sugar falls too low it is extremely dangerous and can even be fatal. Older adults may also be less able to recognise the symptoms of low blood sugar compared to young adults. This is because symptoms such as dizziness and confusion are often less specific in older adults, and can be confused with dementia. Older adults may also take longer to recover from low blood sugar. Given that repeated bouts of low blood sugar can mean that older people are less able to sense when it’s happened in the future, it’s important that drugs prescribed to older adults for type 2 diabetes are given at the correct doses. Care especially needs to be taken prescribing insulin, the body’s blood sugar control hormone, to very old adults as this significantly increases the risk of low blood sugar. Given our ageing population, it is projected that more older adults will have type 2 diabetes in the future. This makes it especially important to improve how we treat diabetes in this age group. Though specific treatment guidelines have been developed, some evidence suggests that care approaches need to be more cautious and personalised to each patient, taking into account their other health conditions, and that treatments consider quality of life for each patient. This article was co-written by Dr James Brown and Dr Srikanth Bellary








