Experts Matter. Find Yours.
Connect for media, speaking, professional opportunities & more.

COVID-19 Pandemic Increasing Substance Use Among Veterans with PTSD
Nine months into the pandemic, everyone has been affected by COVID-19 in some way. However, one group that needs special attention and support is U.S. veterans who were already struggling with symptoms of posttraumatic stress disorder (PTSD). A recently conducted survey by Jordan Davis, assistant professor at the USC Suzanne Dworak-Peck School of Social Work, and Eric Pedersen, associate professor at Keck School of Medicine of USC, found evidence that veterans with PTSD prior to the pandemic were now managing their symptoms with more frequent alcohol and cannabis use. “The pandemic has not been easy on folks, especially for those that have PTSD or an alcohol use disorder (AUD),” said Davis, who also is associate director of the USC Center for Artificial Intelligence in Society (CAIS). “Some of the stories I’ve heard [from study participants] have been heart-wrenching.” An extraordinary resource of veterans not affiliated with VA services Davis and Pedersen lead several efforts examining substance use among veterans. They have assembled a survey group of about 1,200 military veterans, a percentage of whom struggle with PTSD symptoms but have not yet sought professional help via the Department of Veterans Affairs (VA) to improve their wellbeing. “We’ve decided to focus on the population of veterans who, for one reason or another, say they don’t need mental health care,” Davis said. Attitudes about care, transportation barriers or perceived stigma from others may deter them from seeking care for PTSD symptoms, and some self-medicate with alcohol, cannabis, cigarettes, or more rarely, methamphetamine or cocaine. Davis cited larger studies 1,2 that found only about half of the veterans who need some sort of mental health care receive it. Many studies of veterans recruit subjects from the VA who are likely already receiving care. The unique sample group that Davis and Pedersen have created may offer fresh insights into how to motivate these veterans outside the VA system to seek care and how best to deliver it. Tracking pandemic effects on mental health It all began with a one-time survey of young adult veterans to measure drinking habits and willingness to seek help. Pedersen and others had developed a brief intervention that had yielded some success reducing drinking in the short-term, but he knew that sustaining those reductions would be difficult unless the veterans agreed to more formal care. The one-off survey, conducted in February 2020, would set a baseline that could be used to inform the brief intervention content. Then COVID-19 cases began multiplying. Affected cities and states began to impose restrictions on public gatherings and more. Pedersen and Davis soon obtained additional funding from the Keck School of Medicine of USC COVID-19 Funding Program and the National Institute of Alcohol and Abuse to follow up with their sample group and see how these veterans were coping with the unprecedented health crisis. “The result is that we can follow up with these veterans from a pre-COVID-19 time period for the next several years, tracking their depression, anxiety and PTSD symptoms and substance use,” Pedersen said. The researchers aim to understand how the veterans are sleeping, what their stress levels are like, and how things have changed as the pandemic wears on. They hope to gain new insights about what motivates some to seek care and how that can be replicated. So far, the results point to some unfortunate, but not unexpected, news. “We’re finding that those veterans who were struggling with PTSD prior to the pandemic are actually doing worse in terms of their substance use behaviors, drinking and cannabis use, as well as their stressful reactions to the pandemic,” Pedersen said. Pedersen and Davis will continue to follow up with these veterans through at least February 2022, surveying them every three months to see how they are progressing. In addition to the survey, they also conduct in-depth qualitative interviews with a subset of the group to enrich their understanding of what their lives are like now and how things have changed for them. The interviews last about an hour, sometimes more. “We talk about the positive and negative things that have happened and what their expectations are for the future,” Davis said. The details are confidential, of course, but it is clear that the pandemic has upended people’s lives and livelihoods across the United States. The toll on those who were already experiencing mental health issues and addiction has been heavy, but Davis and Pedersen are hopeful that their insights and findings will lead to better treatment and outreach in the future. Reducing barriers to care One bright spot over the past nine months has been the quick embrace of telehealth. The VA was already leading the way to telehealth as a way to improve access to its services, and following the stay-at-home orders of the pandemic, telehealth has grown in acceptance and use. Now, online counseling sessions, Alcoholics Anonymous meetings, and medical visits are commonplace. Pedersen and Davis don’t see that changing even when face-to-face gatherings become the norm once again. It has been a promising start to the research, and Pedersen and Davis are even more excited about what the future may hold. They plan on submitting for more grants to continue to track the mental health and substance use of this group of hundreds of veterans with the goal of understanding what factors lead individuals to seek care. Down the road, they hope to use this longitudinal data to help identify profiles of people more or less likely to seek care. “Then we can tailor interventions to increase their willingness to seek care for a problem like a substance use disorder or PTSD,” Davis said. Recognizing patterns in substance use and when to seek care is very important in helping that part of the veteran population that is trying to deal with symptoms of depression, anxiety, PTSD, or substance abuse on their own. “We know that things are bad now and we can expect that there will be lingering effects for years to come,” said Pedersen. “What we hope is that these findings and our future work will help the VA and others create more effective programs and outreach to address the unique needs of veterans.” 1 Veterans Health Administration Office of Patient Care Services, Analysis of VA Health Care Utilization Among Operation Enduring Freedom, Operation Iraqi Freedom, and Operation New Dawn Veterans. Washington, DC: U.S. Department of Veterans Affairs, 2017. www.publichealth.va.gov/epidemiology/reports/oefoifond/health-care-utilization/. 2 Tanielian, Terri and Lisa H. Jaycox, eds., Invisible Wounds of War: Psychological and Cognitive Injuries, Their Consequences, and Services to Assist Recovery. Santa Monica, CA: RAND Corporation, 2008. www.rand.org/pubs/monographs/MG720.html.

The Food and Drug Administration and the Centers for Disease Control and Prevention recently lifted the pause on the Johnson & Johnson COVID-19 vaccine. The agencies had shelved the vaccine after it was linked to cases of an extremely rare blood clotting disorder. Public health officials are now concerned that as news gets out about the potential side effects of the Johnson & Johnson vaccine, some members of the Black and Hispanic communities may opt out of what could be a life-saving act. “To the Black and Hispanic communities, there has been a long history of untrustworthy behavior by health care systems, and the current issue with Johnson & Johnson may have worsened some hesitancy,” said Dr. Justin X. Moore, an epidemiologist in the Department of Population Health Sciences at the Medical College of Georgia. “To overcome this barrier, companies must continue being open about side effects of the vaccine, and health care workers must be empathetic and listen to their patients’ concerns.” Vaccine safety and the importance of everyone being vaccinated is crucial as America looks to get to the light at the end of this pandemic. If you are a journalist covering COVID-19 and the issues surrounding vaccine hesitancy, then let our experts help. Dr. Justin Moore is an expert in spatial epidemiology and an associate professor at the Institute of Public and Preventive Health at Augusta University. He is available to speak with media regarding this topic – simply click on his name to arrange an interview.

New prostate cancer urine test shows how aggressive disease is and could reduce invasive biopsies
Researchers from the University of East Anglia have developed a new urine test for prostate cancer which also shows how aggressive the disease is. A new study shows how an experimental new test called ‘ExoGrail’ has the potential to revolutionise how patients with suspected prostate cancer are risk-assessed prior to an invasive biopsy. The research team say their new test could reduce the number of unnecessary prostate cancer biopsies by 35 per cent. Prostate cancer is the most common cancer in men in the UK. It usually develops slowly and the majority of cancers will not require treatment in a man’s lifetime. The most commonly used tests for prostate cancer include blood tests, a physical examination known as a digital rectal examination (DRE), an MRI scan or an invasive biopsy. However, doctors struggle to predict which tumours will become aggressive, making it hard to decide on treatment for many men. Lead researcher Dr Dan Brewer, from UEA’s Norwich Medical School, said: “While prostate cancer is responsible for a large proportion of all male cancer deaths, it is more commonly a disease men die with rather than from. “Therefore, there is a desperate need for improvements in diagnosing and predicting outcomes for prostate cancer patients to minimise over-diagnosis and overtreatment whilst appropriately treating men with aggressive disease, especially if this can be done without taking an invasive biopsy. “Invasive biopsies come at considerable economic, psychological and societal cost to patients and healthcare systems alike.” The research team developed the new ExoGrail urine test by combining two biomarker sources - measurements of a protein-marker called EN2 and the levels of gene expression of 10 genes related to prostate cancer risk. It builds on previously developed tests called PUR and ExoMeth. They tested it using urine samples from 207 patients who had been undergone a biopsy for prostate cancer at the Norfolk and Norwich University Hospital (NNUH). When the urine results were compared to biopsy results, the study showed that the test had successfully shown which patients had prostate cancer and which did not. The ExoGrail test also provided risk scores for patients and highlighted those for which an invasive biopsy would have been beneficial. The findings show that using information from multiple, non-invasive biomarker sources has the potential to greatly improve how patients with suspected prostate cancer are risk-assessed prior to an invasive biopsy. Dr Brewer said: “Our new urine test not only shows whether a patient has prostate cancer, but it importantly shows how aggressive the disease is. This allows patients and doctors to select the correct treatment. And it has the potential to reduce the number of unnecessary biopsies by 35 per cent.” The research team was led by Dr Shea Connell, Prof Colin Cooper, Dr Daniel Brewer and Dr Jeremy Clark, all from UEA’s Norwich Medical School, in collaboration with the Norfolk and Norwich University Hospital, the University of Surrey, the University of Bradford, The Earlham Institute, and The Movember GAP1 Urine Biomarker Consortium. The urine biomarker research was funded by the Movember GAP1 Urine Biomarker project, Prostate Cancer UK, The Masonic Charitable Foundation, The Bob Champion Cancer Trust, the King family, The Andy Ripley Memorial Fund, the Hargrave Foundation, Norfolk Freemasons and the Tesco Centenary Grant. Paul Villanti, executive director of programmes at Movember, said: “We are proud to have supported the development of the ExoGrail urine test as part of our Global Action Plan Urine Biomarker project. “Having non-invasive tests which can accurately show how aggressive a man’s prostate cancer is not only reduces the number of men having to undergo painful biopsies, but also ensures that the right course of treatment for the patient is selected more quickly.” ‘Integration of Urinary EN2 Protein & Cell-Free RNA Data in the Development of a Multivariable Risk Model for the Detection of Prostate Cancer Prior to Biopsy’ is published in the journal Cancers on Tuesday, April 27, 2021.

Smell training, not steroids, best treatment for Covid-19 smell loss
Steroids should not be used to treat smell loss caused by Covid-19 according to an international group of smell experts, including Prof Carl Philpott from the University of East Anglia. Smell loss is a prominent symptom of Covid-19, and the pandemic is leaving many people with long-term smell loss. But a new study published today shows that corticosteroids - a class of drug that lowers inflammation in the body – are not recommended to treat smell loss due to Covid-19. Instead, the team recommend ‘smell training’ – a process that involves sniffing at least four different odours twice a day for several months. Smell loss expert Prof Carl Philpott from UEA’s Norwich Medical School, said: “The huge rise in smell loss caused by Covid-19 has created an unprecedented worldwide demand for treatment. “Around one in five people who experience smell loss as a result of Covid-19 report that their sense of smell has not returned to normal eight weeks after falling ill. “Corticosteroids are a class of drug that lowers inflammation in the body. Doctors often prescribe them to help treat conditions such as asthma, and they have been considered as a therapeutic option for smell loss caused by Covid-19. “But they have well-known potential side effects including fluid retention, high blood pressure, and problems with mood swings and behaviour.” The team carried out a systematic evidence-based review to see whether corticosteroids could help people regain their sense of smell. Prof Philpott said: “What we found that there is very little evidence that corticosteroids will help with smell loss. And because they have well known potential adverse side effects, our advice is that they should not be prescribed as a treatment for post-viral smell loss. "There might be a case for using oral corticosteroids to eliminate the possibility of another cause for smell loss actually being a confounding factor, for example chronic sinusitis – this is obviously more of a diagnostic role than as a treatment for viral smell loss. “Luckily most people who experience smell loss as a result of Covid-19 will regain their sense of smell spontaneously. Research shows that 90 per cent of people will have fully recovered their sense of smell after six months. “But we do know that smell training could be helpful. This involves sniffing at least four different odours twice a day every day for several months. It has emerged as a cheap, simple and side-effect free treatment option for various causes of smell loss, including Covid-19. “It aims to help recovery based on neuroplasticity - the brain’s ability to reorganise itself to compensate for a change or injury,” he added. The research was led by researchers at the Cliniques universitaires Saint-Luc in Brussels (Belgium) in collaboration with the Univeristé catholique de Louvain, Brussels (Belgium), the University of East Anglia (UK), Biruni University, Istanbul (Turkey), Aarhus University (Denmark), Université du Québec à Trois-Rivières (Canada), Geneve University Hospitals (Switzerland), Harvard University (USA), Aristotle University, Thessaloniki (Greece), University of Insubriae (Italy), University of Vienna (Austria), the University of Chicago (USA) and the University of Colorado (USA). ‘Systemic corticosteroids in COVID-19 related smell dysfunction: an international view’ is published in the journal International Forum of Allergy & Rhinology.

COVID expert: Prof Lawrence Young, UK
Professor Lawrence Young of the University of Warwick is one of the go-to experts in the UK on COVID-19. A Professor of Molecular Oncology at Warwick Medical School, he can comment on many aspects of the pandemic -- from the nature of the virus itself and its effects in patients, to its impacts on hospitals and wider society. He regularly features on TV, radio, and newspapers in the UK and worldwide, including: If you would like to book an interview with Prof. Young, contact press@warwick.ac.uk or L.Walton.1@warwick.ac.uk

Combating Vaccine Hesitancy Through Messaging
As vaccine hesitancy becomes a threat to Americans' decision to get the COVID vaccine, persuasive messaging is at the forefront of changing people's minds. Allyson Levin, PhD, a visiting assistant professor of communication, believes social media messaging plays a key role—and that post-vaccination selfies can actually help convince people to get the vaccine. "When we don't know what to do, we look to others to guide our behavior," stated Dr. Levin. "It is really important when we see people who share online that they were vaccinated—who are close to us, our friends or family and people we look up to like influencers and celebrities." Further, online communities create a world where it appears that people are getting vaccinated actively. "If we look around and see an environment where people are getting vaccinated, we will want to get vaccinated as well. That will encourage vaccination. At least if we trust those people around us," said Dr. Levin. Dr. Levin also contends that the social media platform TikTok can be extremely useful when information is "scientifically valid, evidence-based and coming from people who understand science like medical professionals." "A unique opportunity we have with TikTok is that users are receiving health information when they aren't looking for it," said Dr. Levin. In addition, she notes the incredible impact company advertisements endorsing COVID vaccinations have had on their wider acceptance. "At the end of the day, it is wonderful that brands are amplifying these messages, like Budweiser donating their airtime during the Super Bowl. There is an element of public relations, too: The brands look good for promoting these messages. But the more people that see these messages, the better." However, Dr. Levin pointed out that, while messaging is extremely important, vaccine availability is crucial. "Access is equally important. Unless people can actually have access to the vaccinations, the message is just one part of it," stated Dr. Levin.

Earlier this week, President Joe Biden proclaimed that April 11 thru 17 would be Black Maternal Health Week in America. In Georgia, the state has consistently been ranked as one of the most dangerous places in this country to be a new mother. Approximately 26 Georgia women die from pregnancy complications for every 100,000 live births, compared to the national average of about 17 women. But even more devastating is the fact that about 60% of the state’s maternal deaths between 2012 and 2016 were found to be preventable, according to the Georgia Department of Public Health. And the mortality rates are much more tragic for Black women in Georgia. African American women are almost three times more likely to die from a pregnancy-related cause than white women in Georgia. Black mothers in rural areas of Georgia are at an even higher risk. “Maternal and infant mortality are really significant indicators of the quality of health in any area, so my colleagues around Georgia really felt challenged to do something that we hadn’t done in a long time in our state, which was to get the data,” says Dr. Chad Ray. “Because you can’t really fix something unless you know who and why. And then you assemble the stakeholders to formulate a plan to make a dent and to move the needle on something that is just so important.” This is an important topic that impacts mothers in Georgia and across the entire United States. And if you are a journalist looking to cover this topic – then let us help. Dr. Chad Ray is the Interim Section Chief of the Department of Obstetrics and Gynecology at the Augusta University Medical Center. He is an expert in the areas of maternal mortality & global women's health initiatives. Dr. Ray is available to speak with media about Black Maternal Health Week - simply click on his icon now to arrange an interview today.

Toolkit is easily incorporated into any laboratory science course Wilmington, Del., April 1, 2021 – St. Georges Technical High School in southern New Castle County, Delaware is the first high school in the United States to use ChristianaCare Gene Editing Institute’s innovative CRISPR in a Box Educational Toolkit™ in a science class. CRISPR in a Box brings to life the much-heralded CRISPR gene editing technology – the “genetic scissors” that allow scientists to edit DNA. The toolkit is designed for educational sessions in secondary and post-secondary schools and is suitable for remote learning. “Gene editing is the future of medicine,” said Eric Kmiec, Ph.D., director of ChristianaCare’s Gene Editing Institute. “Our partnership with the Delaware Department of Education will help cultivate the next generation of genetic scientists and enhance Delaware’s position as a leader in the biosciences.” “We are thrilled that students at St. Georges Technical High School will be the first In the United States to experience a live demonstration of CRISPR gene editing using our Innovative CRISPR in a Box educational toolkit,” said Siobhan Hawthorne, Education and Community Outreach leader at ChristianaCare’s Gene Editing Institute. “This toolkit will provide STEM students with a visual understanding of how the exciting CRISPR technology can unlock medical treatments to improve lives.” Delaware Secretary of Education Susan Bunting praised her department's partnership with ChristianaCare's Gene Editing Institute to develop the “Seeds of STEM” course that teaches high school students about gene editing. “Gene editing approaches diseases in new ways and will have significant impact in the health care and agriscience fields,” Bunting said. “This is a great example of an industry and education partnership investing in youth by providing hands-on knowledge and skills around emerging technology.” “We are so fortunate that ChristianaCare’s Gene Editing Institute reached out to our program to plan a high school ‘first’ opportunity with this new CRISPR experiment,” said Danya Espadas, one of the St. Georges biotech teachers. “Giving students the chance to use a cutting-edge, 21st century tool for medicine in their own high school lab – to have that technology at their fingertips – transcends what they see in a textbook or a video. By being able to do it themselves, it makes it real for them.” Espada said the experiment focuses on editing a gene of a non-infectious E.coli bacteria to become resistant to an antibiotic, thereby allowing researchers to create a new class of antibiotics that cannot be overcome by bacteria that are gene resistant. “We’re talking about eventually saving lives, here,” she said. “What can be more important than that?” The tools in CRISPR in a Box have been designed based on the pioneering discoveries of the Gene Editing Institute that are currently being used to explore next-generation medical therapies and diagnostics for diseases, including lung cancer and sickle-cell anemia. Component items in the toolkit include the CRISPR/Cas complex, a target DNA molecule, a mammalian cell free extract and a synthetic DNA molecule. All materials in the kit are safe, synthetic materials. There are no live cultures or viruses involved. The kit is meant to provide a hands-on demonstration of CRISPR’s capabilities, and not allow for manipulations of living organisms. “The kit is easy and fun to use,” said Kristen Pisarcik, research assistant at the Gene Editing Institute who has taught students at Delaware Technical Community College which first used the toolkit. “In a short period of time students will reliably and successfully complete the laboratory activity and be able to see the results of gene editing,” she said. Since the foundations of the kit touch upon key themes in biology, it can be readily incorporated into practically any science or biology course with a laboratory component, “One of the beauties of CRISPR in a Box is that there is no need to purchase specialized equipment. If a teaching lab can support bacterial cultivation, it can perform the in vitro gene editing lab activity,” Pisarcik said. CRISPR in a Box is the evolution of a partnership between the Gene Editing Institute, Delaware Technical Community College and Rockland Immunochemicals that began in 2017 with a National Science Foundation grant to develop the first-ever gene editing curriculum for community college students. Video and photo collection of first class in U.S. to use CRISPR in a Box™ educational gene editing toolkit. About ChristianaCare’s Gene Editing Institute The Gene Editing Institute, a worldwide leader in CRISPR gene editing technology and the only institute of its kind based within a community health care system, takes a patient-first approach in all its research to improve the lives of people with life-threatening disease. Since 2015, researchers at the Gene Editing Institute have been involved in several ground-breaking firsts in the field, including the development of the first CRISPR gene editing tool to allow DNA repairs outside the human cell which will rapidly speed therapies to patients and a unique version of CRISPR called EXACT that reduces the number of off-target edits to other areas of the genome, which is vital for further research and patient applications. Its researchers are currently developing a patient trial for lung cancer using CRISPR and employing the technology to combat the COVID-19 pandemic. About the biotech program St. Georges Technical High School The Biotech career program of study at St. Georges Technical High School is the first such program offered in a Delaware high school. With two teachers and approximately 100 students in grades 10-12, the program presents advanced content in biology and chemistry with opportunities for students to learn basic laboratory techniques and procedures and to maintain and operate common instruments and equipment used in a biotechnology laboratory. St. Georges is a comprehensive career and technical high school with 1,100 students who study in one of 16 different career pathways.
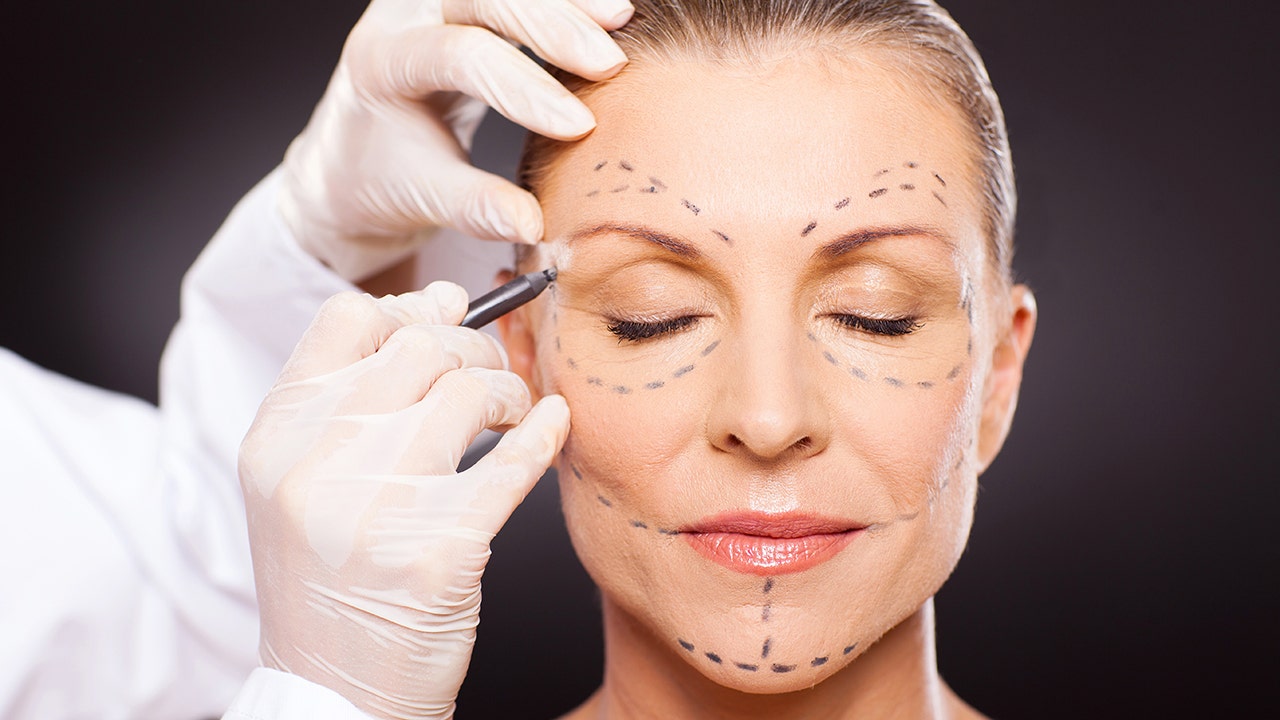
The Zoom Boom? More and more Americans are getting plastic surgery – let our expert explain why
After almost a year where most American offices went unused, experts are noticing an unexpected side effect from all those online meetings. It appears that prolonged exposure to seeing yourself in that tiny box during video calls is inspiring a sudden uptick in plastic surgery. The plastic surgery industry is booming during the coronavirus pandemic, largely due to the increase in the number of virtual meetings offered through Zoom and other video web services. Call it the “Zoom boom.” The interest in cosmetic surgery is boosting appointments for Botox, lip fillers and other plastic surgery procedures that help people feel more attractive on computer screens, according to Dr. Maria Helena Lima, an assistant professor of Surgery for the Section of Plastic and Reconstructive Surgery in the Medical College of Georgia at Augusta University. “In the last few months, there has been a jump in the number of patients wanting plastic surgery procedures,” said Lima. “We have discovered that when people are in Zoom meetings, they should be listening to the content and paying attention to what’s going on, but they’re not.” Lima says participants are oftentimes looking at themselves on the screen and wondering what could be done to alter their image. It is a trend that offers up some interesting questions: • Along with the Zoom boom, are there other reasons people are opting to go under the knife for an elective procedure? • Are there long-term consequences to these decisions? • What do patients need to know first to avoid any safety or health issues? There’s a lot to know about this topic, and if you are a journalist looking to learn more, then let us help with your coverage. Dr. Maria Helena Lima is one of the nation’s leading plastic surgeons with 12 years of experience specializing in aesthetic plastic surgery, facial reconstruction and craniofacial pediatric plastic surgery. She is available to speak with media about this emerging trend. Simply click on her name now to arrange an interview today.

This week’s shocking news of golf legend Tiger Woods rolling his vehicle and sustaining serious injuries to his right leg have sports fans, journalists and most of the world watching and waiting for word of whether he’ll play again. According to ESPN, the injuries are extensive: Tiger Woods is recovering from a lengthy surgery to repair what a doctor said Tuesday night were "significant orthopaedic injuries to his right lower extremity" suffered in a single-car rollover crash hours earlier on a steep roadway in a Los Angeles suburb. As part of a statement on Woods' official Twitter account, Dr. Anish Mahajan of Harbor-UCLA Medical Center updated the famed golfer's condition, saying in part that Woods had multiple "open fractures" to his lower right leg, and he had a rod placed in his tibia and screws and pins inserted in his foot and ankle during an emergency surgery. "Comminuted open fractures affecting both the upper and lower portions of the tibia and fibula bones were stabilized by inserting a rod into the tibia," said Mahajan, the chief medical officer and interim CEO at Harbor-UCLA. "Additional injuries to the bones of the foot and ankle were stabilized with a combination of screws and pins. Trauma to the muscle and soft-tissue of the leg required surgical release of the covering of the muscles to relieve pressure due to swelling." ESPN – February 23 If you’re a journalist looking to know more about this type of injury, what the recovery process usually involves and what the long-term prognosis may be – then let us help. Dr. Monte Hunter serves at Augusta University as the Satcher Distinguished Chair of the Department of Orthopedic Surgery and director of the Sports Medicine Program. Dr. Hunter is an expert in reconstruction and sports injury prevention – and he is available to speak with media about this topic. Simply click on his icon now to arrange an interview today.






