Experts Matter. Find Yours.
Connect for media, speaking, professional opportunities & more.

Amid "Likes" and "Shares," Facebook Jeopardizes Children's Health and Safety
On February 4, 2004, a 19-year-old Mark Zuckerberg launched “TheFacebook.” Developed in his Harvard University residence hall, it began as a networking service for his roughly 7,000 classmates. Today, it is the most popular social media platform in existence, boasting over three billion monthly active users worldwide. Through two decades of “likes” and “shares,” Facebook has transformed how people connect, interact and think. Driving everything from dinner parties and concert outings to political campaigns and protest movements, it has frequently been celebrated for its ability to convey information, mobilize groups and galvanize change. However, it has also been criticized for its questionable content management choices, its suspect data collection practices and, perhaps most notably, its role in feeding an ever-growing mental health crisis among children and adolescents—a charge Zuckerberg refutes. Elizabeth Burgess Dowdell, PhD, RN, FAAN, is a professor in Villanova University’s M. Louise Fitzpatrick College of Nursing and an expert on the health and safety risks posed by social media. From her perspective, Facebook and platforms like it have undoubtedly played a part in heightening levels of emotional distress and physical harm among youths. “Statistically, it’s well-established in the literature that mental health issues and concerning behaviors among children have escalated tremendously,” said Dr. Dowdell. “They’re becoming sadder, more depressed and lonelier, even though they’re very connected.” To Dr. Dowdell’s point, mental health disorders began rising precipitously among young people in the years following Facebook’s launch. Per the Centers for Disease Control and Prevention (CDC), the percentage of children aged 6 to 17 years “ever having been diagnosed with either anxiety or depression” increased from 5.4% in 2003 to 8% in 2007 and 8.4% in 2011-2012. And just last year, in the era of Instagram and TikTok, Mental Health America found that 11.5% of children in the United States were struggling with severe depression, with 16% of youths aged 12 to 17 years having experienced a major depressive episode in the past 12 months. A contributing factor, according to Dr. Dowdell, is the way social media construes reality. Flooded with images, posts and videos that show hyper-idealized, rose-colored representations of life, impressionable young users can be made to feel isolated, inept or dissatisfied with their appearance. “I think adults understand that a ‘perfect’ picture is often preceded by a dozen other photos,” she said. “Kids don’t always see it like that. They focus on what makes them happy and what makes them sad—and what makes them feel sad about themselves.” Tragically, throughout the social media age, this sadness has been tied to increasing rates of suicide, self-harm and risky behavior among youths. A 2023 CDC study found that the suicide rate for children aged 10 to 14 years tripled from 2007 to 2018 (from 0.9 deaths per 100,000 to 2.9), and in 2021-2022, the National Center for Missing and Exploited Children noted a 35% year-over-year increase in reports of suspected child sexual exploitation. Amid these frightening statistics, Dr. Dowdell emphasizes the importance of caring, compassionate adults’ involvement in young people’s lives. She notes these individuals’ presence can not only shield youths from potentially hazardous situations but give them the tools to cope with traumatic episodes and feelings of despair. “The critical factor that helps children become resilient is having a support system—having family members, parents or trusted adults with whom they can talk,” Dr. Dowdell shared. “They might go down the rabbit hole, but they have someone to pull them out, someone to help them.” For adults concerned about their loved ones’ social media use, Dr. Dowdell stresses that empathy and understanding are key. In turn, she advocates for an approach that reflects the supposed purpose of Facebook and platforms like it: active conversation. “It all comes back to communication,” she said. “Parents and guardians need to role-model responsible behaviors. They need to talk about these things: ‘What did you look at today?’ ‘What was good?’ ‘What was bad?’ ‘What did you think?’ ‘How did you feel about that?’ “It’s much like, when children are little, reading them books. When we read to children, we engage them… Why not read the social media feeds, look at the Facebook posts or go through Instagram? These forms of engagement, the conversations we have, let them know they can come and talk.”

Acute Care Nursing Goes Virtual
At ChristianaCare, our patients are our number one priority. That perspective keeps us thinking about new ways to deliver care, including those that allow our caregivers to put their knowledge, skills and focus to the best use. Video: ChristianaCare Virtual Acute Care Nursing Virtual acute care nursing is one way we are making sure our caregivers are working at the highest levels to care for our patients in our hospitals. What is virtual nursing? This program allows experienced nurses to practice virtually in another location. Nurses working virtually help nurses at the bedside by documenting health information, such as medication histories; providing patient education; monitoring patient lab work; completing patient admission documentation; and helping with discharge planning and care coordination. Podcast: Virtual Nursing in the Hospital with Michelle Collins and Melanie Ries By working virtually, these nurses help remove some of the documentation burden for our clinical staff while also improving our patient outcomes. For example, a virtual acute care nurse can take the time to explain to a patient what their at-home care plan will look like, when to take their medications or even understand more about their condition. That allows our bedside nurses to keep their focus on the immediate needs of their patients. How does virtual nursing work? If a patient has a question about their medicine or wants to know more about their impending discharge, they can use a computer tablet that’s placed next to their bed to contact their virtual nurse, who will answer the call. Patients want to feel that someone is available to talk with them, and that’s exactly what our virtual nurse program provides. While our bedside nurses work on a unit caring for multiple patients, our virtual nurses care for one patient at a time without distraction. How is ChristianaCare using virtual nursing? We are currently using a virtual nursing care delivery model in more than 500 of our acute care beds – that’s about 41% of all the beds we have in Wilmington and Christiana hospitals. Nearly 19,000 patients have received this kind of innovative care at ChristianaCare. Our patients and nurses have been involved in over 53,000 calls, spending between seven and nine minutes each time they talk. Why does this matter? It’s no secret that nurses have been overburdened with high patient volumes and labor shortages that have affected the entire health care industry. Given this, it’s imperative to think of new models to support our caregivers, ease their workload and make sure we are providing expert care. Improvements in patient care – along with our patient experience scores – show us the value of the program. Virtual nursing allows us to do that. There also are other advantages to virtual nursing. It can be an option for skilled nurses who aren’t able to handle the physical demands of the job since the interaction with patients is through a tablet. Virtual nursing also offers an opportunity to help early-career nurses learn from experienced caregivers. A virtual nurse can provide mentoring to the bedside nurse by acting as an extra set of eyes and ears to help assess a patient or talk through a challenge. This approach can also help retain more of our early-career nurses, which is good news for all of us. We see virtual nursing as another tool to help our caregivers serve with love and excellence. And let’s be honest — we all want good care to be as easy as pushing a button. Thanks to virtual nursing, it is.

Wilmington Hospital Emergency Department Earns Lantern Award for World-Class Excellence
ChristianaCare’s Wilmington Hospital Emergency Department is one of 53 emergency departments around the world to receive the Emergency Nurses Association (ENA) Lantern Award for 2023, recognizing the excellence of its caregivers in incorporating evidence-based practice and innovation. The ENA Lantern Award celebrates emergency departments that demonstrate exceptional leadership, practice, education, advocacy and research performance. It honors the late Florence Nightingale, who is credited as the founder of modern nursing and is referred to as the “Lady With the Lamp” for her round-the-clock care given to wounded soldiers during the Crimean War. “Every day, our caregivers bring to life the ChristianaCare values of love and excellence through the ways they care for our neighbors who come to the Wilmington Hospital Emergency Department,” said Danielle Weber, MSN, MSM, RN-BC, NEA-BC, chief nurse executive and chief nursing officer of Wilmington Hospital. “By putting the patient first and rethinking outdated models of care, we have created a better experience for patients at a time when they are often most in need. This recognition signifies the transformative effect of our commitment to being exceptional today and even better tomorrow.” Rooted in history, focused on the future Wilmington Hospital has served the community for nearly 125 years, meeting diverse medical needs and providing a safety net for people in underrepresented communities. The Wilmington Hospital Emergency Department is the second-busiest ED in the state, with 58,744 visits in fiscal year 2023. Combined, ChristianaCare’s emergency departments are ranked 12th in the United States and 7th on the East Coast in number of patient visits, according to the American Hospital Association. A highly engaged staff supports the high volume of work in the department, where nurses serve in collaborative decision-making, shared governance and nurse autonomy, “practicing in an environment of empowerment,” said ED nurse Christina Hoddinott, MSN, RN, FNP-BC, CEN, CPE, who helped work on the Lantern application for Wilmington ED. “The staff who perform the work participate in decision-making that directly affects their practice,” Hoddinott said. “When our patients walk through our emergency department doors in their unexpected and stressful moments of need, we do everything we can to see that they receive the highest level of care.” Doreen Nord, MSN, RN, CEN, NPD-BC, nurse manager for Wilmington Hospital ED, said the Lantern award reflects the greatness seen every day among its nursing caregivers. “Their commitment and compassion shine, and there is never a doubt about who is most important — our patients,” Nord said. “We are honored by this recognition, the highest available in emergency nursing.” A collaborative effort Wilmington Hospital ED and the other Lantern recipients were recognized in the Hall of Honor at Emergency Nursing 2023, ENA’s annual conference, Sept. 21-23, in San Diego, California. See the list of other award recipients here. “Each and every emergency department on this list has worked extremely hard implementing innovations to better their emergency department for staff and patients alike,” said ENA President Terry Foster, MSN, RN, CEN, CPEN, CCRN, TCRN, FAEN. “Hearing the excitement these EDs had when notified that they were a recipient was so heart-warming and reminded me of the commitment that ED nurses have to continuous improvement.” In Wilmington, the spirit of collaboration and support among caregivers creates an environment that ensures patients receive the highest level of care. Hoddinott likens her fellow caregivers to puzzle pieces — each one is dynamic and unique. “When the pieces come together, we have one big complete puzzle. We are a team that supports each other during stressful moments, happy occasions and all the in between,” she said. “Our team does not take for granted the ‘specialness’ we have here, and our patients can truly feel that when they come through our doors.”

As Popularity of Weight Loss Medicine Soars, Professionals Caution Against “Magic Pill” Mindset
A growing weight-loss fad has been dominating headlines this summer. No, it isn't a new type of trendy diet, exercise regimen or social media influencer-touted superfood. It's two medications—Ozempic and Wegovy—that have skyrocketed in popularity as more Americans turn to these once-weekly injections to aid in their weight loss efforts. But, while acknowledging the drugs' effectiveness, their intended patient populations and appropriate usage has become far more nuanced and situational, and the intended outcome of long-term weight loss and health is dependent on more than just taking either of these medications once a week. "While these medications can be helpful for some people who struggle with weight loss, it's important to remember that they are not a magic solution," said Rebecca Shenkman, MPH, RDN, LDN, director of the MacDonald Center for Nutrition Education and Research at Villanova University's M. Louise Fitzpatrick College of Nursing. First, it's important to understand the components and histories of both Ozempic and Wegovy. They are prescription medications of the same drug, semaglutide, which belong "to a class of drugs known as glucagon-like peptide-1 (GLP-1) receptor agonists, originally developed to treat type 2 diabetes," per Shenkman. It was discovered by researchers that significant weight loss was a side effect of semaglutide. Ozempic is the 2017 FDA-approved drug used to help treat diabetes. Currently, it is not FDA approved for weight loss and typically not covered by health insurance when used for that purpose, per Shenkman, but is often prescribed off label for "weight management in certain individuals who do not have diabetes, but struggle with obesity or [are] overweight." Wegovy was approved by the FDA in 2021 as an anti-obesity drug used for individuals living with obesity or individuals with excess weight, but not classified as living with obesity, who also have other associated health problems. "When used correctly, the drugs can have many benefits," Shenkman said. "[Semaglutide] is shown to improve diabetes and body weight in addition to seeing improvements in cardiovascular health and risk factors." However, "correct use" is what concerns Shenkman and other health and nutrition professionals. "Anti-obesity drugs are a valuable tool for people who have not experienced adequate benefit from self-directed or professionally directed lifestyle treatment," she said. "However, what we are seeing more and more of now is that people are requesting anti-obesity medications without meeting eligibility criteria for drug use, [such as] body mass index and weight criteria, [or] having the foundational knowledge and application of healthy lifestyle behaviors prior to medication use." To Shenkman's first point, there are several factors, especially in American society, driving those who may not meet the criteria for these medicines or even truly need them to request and ultimately receive the drugs. The media's portrayal of ideal body image is an enormous influence, which can lead to "body dissatisfaction and a desire for quick weight loss solutions," said Shenkman. Advertisements for these drugs often promote those ideas, and even downplay side effects, making them more appealing. Intrinsically tied to body image is the struggle many individuals have with psychological issues related to food, such as emotional or binge eating. "They feel that their self-worth is tied to their weight, and they will do almost anything to lose weight, whether it be five or 50 pounds." Shenkman said. "These individuals might believe that medication will help them control their eating habits more effectively." Identification of such issues prior to prescription approval is something that providers need to be aware of and screen for, Shenkman said. "It is so important for providers to complete a comprehensive pre-treatment assessment of their patients who start on weight loss medications. Unsupervised or improper use can lead to malnutrition, unhealthy weight loss or even a worsening of an undiagnosed or undertreated eating disorder or mental health condition." But even users who meet all pre-treatment criteria may be turning to the drugs in haste, or believe that they alone will solve their problems, and do so quickly. "Americans are known for having that 'quick-fix mentality' where people often seek quick solutions to their problems, including weight loss," Shenkman said. "Weight loss medications might promise faster results compared to lifestyle changes, which can take time and dedication." Compounding this "quick-fix mentality" is the frustration many feel when they fail to see results after multiple unsuccessful attempts at weight management. "The abundance of information on diets, exercise routines and weight loss programs can be overwhelming… Some may turn to medications as they seem more straightforward and require less effort to understand," explained Shenkman. But, as health care providers know, they are far from straightforward. All drugs, including Ozempic and Wegovy, come with the potential for side effects, which can vary with the individual. Headlines this summer focused on reports of users experiencing gastroparesis, described by Shenkman as the "the slowing down or 'paralysis' of the digestive system and gastric (or stomach) emptying." Though most often reported to cause nausea and vomiting, complications of gastroparesis can be quite serious. "If someone continues the medication and experiences chronic gastroparesis, complications to be aware of include malnutrition, dehydration, acid reflux, blood sugar control and even bowel obstruction," Shenkman said. The American Society of Anesthesiology also recently issued guidance on the use of such drugs prior to surgery, given potential life-threatening complications. "When prescribing anti-obesity medication, it is the responsibility of healthcare providers to inform patients about potential side effects and risks associated with the medication," Shenkman said. "It is also the right of the patient/consumer to ask questions and understand what they are putting in their body. A thorough discussion about benefits and possible adverse effects can help patients make informed decisions about their treatment." Many users may also not fully understand that these drugs are usually taken long-term, even after reaching a desired weight. Stopping without the knowledge of how to keep the weight off may lead to its return. Considering the pros and cons of the drugs, Shenkman's advice is simple. "Weight loss medications should always be used as part of a comprehensive weight management plan, which includes a balanced diet, regular physical activity and lifestyle changes. Relying solely on medications without addressing other aspects of weight management is not likely to lead to long-term success no matter how long you stay on a medication."

Analysis of evacuations and preparedness as deadly wildfires continue to rage in Hawaii
The University of Delaware's Disaster Research Center boasts several experts who can provide insight into preparedness, evacuation efforts and recovery in regards to the deadly wildfires that are ravaging Hawaii. Tricia Wachtendorf: Evacuation decision-making, disaster response and coordination, disaster relief (donations) and logistics, volunteer and emergent efforts, social vulnerability. James Kendra: Disaster response, nursing homes and hospitals, volunteers, response coordination. Sarah DeYoung: Pets in emergencies, infant feeding in disasters and decision-making in evacuation. Specifically related to Hawaii: "Hawaii is really unique with animals because they have more progressive policies than many mainland states but of course, limited space." Jennifer Trivedi: Challenges for people with disabilities during disaster, cultural issues and long-term recovery. If you'd like to set up an interview with any of these experts, simply click on their profile.

New Policy on BMI Use Will Change How Physicians Approach Diagnoses and Care
The Body Mass Index – or BMI – table was created in the mid-1800s, and for the last several decades has been viewed as the choice tool to diagnose obesity. However, the American Medical Association (AMA) recently issued a policy clarifying the role of BMI after taking a comprehensive look at both its benefits and limitations as a diagnostic tool. In short, the new policy urges physicians to use BMI only in conjunction with other measures of risk and recognizes the historical shortcomings of the oft-used formula. Lisa Diewald, MS, RDN, LDN, is the program manager of the MacDonald Center for Nutrition Education and Research with Villanova’s M. Louise Fitzpatrick College of Nursing. She applauds the AMA for embracing a more holistic approach to weight and health in individuals. “This is a huge step forward and I think it will ultimately lead to better health care and an improved practitioner-patient relationship,” Diewald said. To understand why, one must first understand the history of BMI’s use. The formula that spits out the number we have all come to understand as our BMI considers a person’s height and weight. It was developed in the mid-19th century by a Belgian sociologist to measure the socially ideal person. The modern term and application came about in the 1972 and has been a routine measurement ever since because it is easy, fast, costs nothing and in some cases, said Diewald, does correlate with body fat. But in recent years, large scale studies have exposed some of the limitations of the measure, building to the point where they needed to be weighed against the overt benefits. For starters, BMI does not measure body fat – or adiposity – directly. Adiposity, per Diewald, is more closely associated with health risk than BMI. “For this reason, health risk for some individuals with normal BMI but high body fat has been underestimated, and some with high BMI but normal body fat levels have been overestimated,” she said. Nor does it “differentiate between muscle, bone and body fat, or distribution of fat on the body,” Diewald said. “We know that all these factors can influence health and chronic disease risk.” Other comorbidities or chronic conditions that wouldn’t show up on a BMI chart alongside a number in the “normal” range can also impact health. Conversely, there are health conditions that might be incorrectly assumed just because a BMI is high. “Not every person with a high BMI experiences these chronic conditions, so developing a more holistic approach can lead to better assessment, treatment and outcomes,” Diewald said. Another shortfall she pointed out was its failure to factor in gender, race, body composition, ethnicity or physical activity level. Think back to the origins of the chart, intended to be a social standard created in Europe nearly two hundred years ago. “BMI tables were originally designed in the 1800’s using a population of white men,” Diewald said. “Understandably, at one point in time it was all we had to evaluate weight status, but it may not be accurate to use this standard alone with all groups of people.” These societal, gender and racial/ethnic factors led the AMA to explicitly cite “historical harm, use for racist exclusion and because BMI is based primarily on data collected from previous generations of non-Hispanic white populations” in the new policy on its clinical use. Additionally, the policy addressed the differences in body composition across genders, races and ages that were not being considered. There is also an ignored mental component in its use to diagnose obesity, which can lead to avoidance of doctor visits and, in turn, further physical issues. “Obesity is a multifactorial, complex condition and addressing it with individuals needs to be done with empathy and sensitivity, beginning with how it is measured,” Diewald said. “There are numerous factors influencing weight well beyond simply food intake, physical activity level and BMI, so it is important for practitioners to recognize that and communicate this to patients. “It is extremely difficult for people with higher weight to be told that they have a high BMI and simply need to eat less and move more. When BMI is used as the sole indicator of weight status, this can be psychologically damaging. We know that many who have been told to lose weight simply based on a high BMI may avoid going to the doctors for routine medical visits and skip necessary preventive care.” It will not be easy, she said, to move away from a method used for so long that has been ingrained as a part of a routine medical visit, but Diewald thinks utilization of the tool in conjunction with other assessments is the best way put this new policy to practice. She advocates for measures such as “Using BMI as only one of several indicators of chronic disease risk, asking permission to discuss weight and health risk, [and] using shared decision-making between practitioners and patient to determine course of treatment.” Education is also paramount to proper assessment of weight-related health risks. “Education cannot stop with physicians, however,” she said. “I think this provides an excellent launching pad for enhanced collaboration among health professionals such as dietitians, nurses, nurse practitioners, physician’s assistants and others involved in providing care, nutrition counseling and lifestyle modification support to patients… Doing this can better fine tune recommendations for treatment, leading to improved outcomes.”

Richard G. Cuming Appointed Chief Operating Officer of ChristianaCare
(WILMINGTON, Del. – June 26, 2023) Richard G. Cuming, Ed.D., MSN, RN, NEA-BC, FAAN, has been named ChristianaCare’s chief operating officer (COO). Cuming has been serving as interim COO since the beginning of this calendar year. He joined ChristianaCare in 2016 as the system’s first Chief Nurse Executive. In his role as COO, Cuming oversees the delivery of efficient and fiscally responsible system operations. He also works with other leaders to ensure high-quality and safe patient care. “Ric has been an invaluable asset to ChristianaCare over the past seven years, especially in navigating the many challenges of the COVID-19 pandemic” said Janice E. Nevin, M.D., MPH, ChristianaCare president and chief executive officer. “As leader of our extraordinary, Magnet®-designated nursing staff and president of ChristianaCare HomeHealth, he has improved the lives of patients and caregivers alike. I look forward to him flourishing in this new role.” Prior to coming to ChristianaCare, Cuming oversaw the operations and strategic direction of nursing services, perioperative and emergency services at Einstein Medical Center Philadelphia, Einstein Medical Center Elkins Park, MossRehab, Einstein Center One and Willowcrest, a skilled nursing center. Ric also previously worked at Jackson Health System in Miami as senior vice president and chief nursing executive, and he served as senior vice president and chief administrative officer at Jackson South Community Hospital. Cuming serves on the board of directors of the DAISY Foundation and board of trustees of the Association of Perioperative Registered Nurses Foundation. He was inducted into the American Academy of Nursing and is an alumnus of both the Robert Wood Johnson Foundation Executive Nurse Fellowship Program and the Wharton School of Business General Management Program. Cuming earned his diploma of collegial studies in nursing at John Abbott College in Montreal, his Bachelor of Science in nursing from the University of Ottawa, his Master of Science in nursing at the University of Miami and his doctorate in adult education and human resource development with a minor in advanced nursing administration from Florida International University.

The Loneliness Epidemic: Fathoming Feelings and Emotions
Last month, United States surgeon general Vivek Murthy released an advisory to address a budding "public health crisis." The culprit is not immediately visible, like the shutdown-spurring COVID-19 pandemic, but it is currently affecting nearly half of all adults in the U.S. It's our widespread senses of loneliness and isolation, and Murthy says addressing these feelings is "critical" to addressing issues of mental health in America. Assistant professor Guy Weissinger, PhD, MPhil, RN, is a nurse, scientist and educator focusing on mental health and health systems at Villanova University's M. Louise Fitzpatrick College of Nursing. Dr. Weissinger believes, despite the difficult nature of navigating unseen nemeses, there are ways to quell this epidemic and save lives. Q: Why is the feeling of loneliness now seen as a crisis? Dr. Weissinger: It's important to understand that loneliness is not just a person not having friends or not having good relationships. Loneliness is a feeling, the sense that one is distant from others while yearning to feel connected. These two sides make loneliness hard to understand sometimes because there are people who are happy with low amounts of social engagement and there are people who feel lonely even when they are surrounded by friends. Like hunger saying it's time to eat, loneliness is a message that we are not fulfilling a social and psychological need—and it's a big problem because so many parts of our mental and physical health are tied to having active social engagement. Q: In an increasingly connected world, why are these feelings of isolation also increasing? DW: Interacting with other people doesn't actually make us less lonely, especially through things like social media. A sense of being emotionally close to others—reciprocity of attention and care—is what makes people less lonely. It's clear that people are spending less time focused on social relationships than in the past. The "connection" that we have through social media is not the connection that addresses our deeper psychological needs. Upvotes and clicks feel good, but they do not make us feel understood and appreciated for our whole selves. In-depth conversations, shared projects and laughing about inside jokes—the kind of things that happen over extended interactions—are what actually make us feel less lonely. This isn't to say that people don't connect and get less lonely when they engage digitally. It's about the quality and depth of interactions, not the modality. Q: What are some ways loneliness and isolation can be addressed? DW: If you are lonely, reach out to someone. Often, we wait for others to initiate because we don't want to be a bother or fear rejection. If they say no, move on to another person. It's hard not to take it personally, but if you are feeling lonely, the worst thing to do is to dwell on why it's hard to schedule with "Friend A" and instead focus on finding another person to connect with. And when you are with people, try to focus your attention on them. Put away your phone or other distractions and ask open-ended questions like, "What's the best thing that happened this week?" or "How has [thing you know they enjoy] been recently?" Even if it's not a person that you are super close to, both listening to them and opening up yourself helps you feel more connected. If you are worried that someone else is lonely, ask them to do something, especially if it's something you know they like. Asking a person who loves movies to go see a movie with you will make them feel like you care more than asking them to a yarn festival, even if you'd prefer the yarn festival. Dr. Weissinger says people who report that they have a regular social connection with others, especially in person, are more physically active, less likely to be depressed and are better able to better navigate difficult circumstances. "While we often talk about resilience as being an individual trait, having good social support is one of the most powerful kinds of resilience," mentions Dr. Weissinger. "When times are hard, we can rely on our friends, family and larger social network to help with problem solving, resources, emotional support and even just simple distraction." Dr. Weissinger says that a crisis as large as loneliness and isolation can't be solved through the recommendations of one person, but says connection and unity are key to fighting back against this epidemic. "People with more and more varied connections don't have simpler lives or less bad things happen to them, but they get through them easier because they can rely on others to help them manage in the ways they need."

Health Professions Academic Building on the Armstrong Campus in Savannah Georgia’s only public medical school has received funding approval to open a new four-year campus in Savannah, an expansion that will provide greater access to education and training for medical students and ease the state’s ongoing shortage of physicians. The new campus of Augusta University’s Medical College of Georgia (MCG) is expected to enroll its first students on the Armstrong Campus of Georgia Southern University by Fall 2024, pending approval by the Liaison Committee on Medical Education, the accrediting body for medical schools in the U.S. and Canada. The campus will be located in the existing Armstrong Center and the Health Professions Academic Building of Georgia Southern’s Waters College of Health Professions. Located down the street from Savannah’s St. Joseph’s Hospital, it would be MCG’s third four-year campus in Georgia. The MCG educational experience is anchored at its main campus in Augusta, with another four-year campus located in Athens in partnership with the University of Georgia. “Georgia ranks 40th in the nation for both the number of active physicians and the number of primary care doctors,” Georgia House Speaker Jon Burns said. “Georgians experience this reality every day. Increasing opportunities within the University System of Georgia allows Augusta University’s Medical College of Georgia to educate and train more students and meets a clear need to make sure our communities receive better health care. Georgia needs more doctors, and I’m proud we are making this investment in our future.” The Board of Regents of the University System of Georgia (USG) on Tuesday approved $1.7 million for renovations at Georgia Southern’s Armstrong Campus to help make the new campus a reality. The money was included in the fiscal year 2024 state budget passed earlier this year by the Georgia General Assembly and signed by Gov. Brian Kemp on May 5. “We’re grateful to Governor Kemp, Speaker Burns, Lt. Gov. Jones and the General Assembly for their support in helping MCG and the university system expand one of the best public medical colleges in the nation and help get more doctors into our local communities,” USG Chancellor Sonny Perdue said. Four-year campuses provide the full spectrum of medical education, from basic sciences to clinical experiences. “This campus expansion is a momentous milestone for Augusta University and the Medical College of Georgia, standing as a testament to the unwavering support we have received from Speaker Burns, state Rep. Butch Parrish, Governor Kemp, the entire General Assembly and Chancellor Perdue,” said Augusta University President Brooks A. Keel, PhD. “Through this collaboration, we are forging a brighter future for health care in Georgia and fulfilling our shared commitment to producing more doctors for our state. I extend my deepest gratitude to all those who have championed this vision, including St. Joseph’s/Candler Health System, whose exceptional partnership has provided invaluable clinical experiences for our students. Together, we are bolstering the state’s medical community and strengthening Southeast Georgia’s access to quality health care.” MCG’s statewide educational model also has students learning at two-year, clinically focused regional campuses in every corner of the state, including the Southeast Campus, established in 2011 and based at St. Joseph’s/Candler in Savannah, and Southeast Georgia Health System in Brunswick. Other regional campuses include the Southwest Campus based in Albany and the Northwest Campus based in Rome. “This partnership with Augusta University and the Medical College of Georgia is another example of how together, the governor, our legislators, the University System of Georgia and Georgia Southern University are collaborating to meet the growing needs of Southeast Georgia,” added Georgia Southern University President Kyle Marrero. “These programs on our Savannah campus further Armstrong’s history of being a leader in training health care professionals and complement our efforts to expand nursing education and develop our future physician assistant program.” Through this partnership, Georgia Southern is providing approximately 23,000 square feet of instructional and lab space in its Armstrong Center and the Waters College of Health Professions’ Health Professions Academic Building. This includes 10,000 square feet of dedicated student group workspace and faculty and staff offices and 13,000 square feet of shared anatomy lab and large classroom space. The renovations include the creation of a new anatomy lab within the Health Professions Building, as well as minor renovations and new furniture, fixtures and equipment for the student group workspace and faculty and staff offices. The new campus would allow MCG to accept 40 more students per year, increasing its class size, already one of the nation’s largest, to 304 students per class. “As the state’s only public medical school, it is both our responsibility and commitment to produce more doctors for Georgia, and this growth in our class size is one way we can fulfill what I consider to be our most critical mission” said MCG Dean David Hess, MD. “This expansion would not be possible without the support of Governor Kemp, the Georgia Legislature, the University System of Georgia, Augusta University President Brooks Keel, and our colleagues at Georgia Southern University. I am also thankful for the unwavering support of St. Joseph’s/Candler Health System, including its CEO Paul Hinchey and chief medical officer Dr. Julia Mikell, a 1976 MCG graduate. Physicians and staff at St. Joseph’s/Candler have been exceptional educational partners, serving as a home base for our Southeast Campus, and providing rich clinical experiences for our third- and fourth-year students, for well over a decade. I know that commitment will extend to students at this new four-year campus.” “This is a sentinel event not only for the future of health care in Georgia, but also for Savannah and the region,” added Paul P. Hinchey, president and CEO of St. Joseph’s/Candler. “We have had a great relationship with MCG for more than a decade and our physicians have been instrumental as faculty in teaching third- and fourth-year students in Savannah. SJ/C has also served as a longstanding clinical site for nursing students from Georgia Southern and from the Armstrong campus. Creating a four-year medical school campus in Savannah will strengthen the medical community in Savannah and throughout Southeast Georgia. I want to thank Speaker Burns, Dr. Hess and the University System of Georgia for making this great vision a reality.” “I am excited to help build a campus that will continue MCG’s mission of educating the next generation of physicians,” said Elizabeth Gray, MD, associate dean at MCG’s Southeast Campus, based in Savannah and Brunswick. “I am confident that Georgia Southern will be an exceptional educational partner, and am excited to continue working with the leadership, physicians and staff at our longtime partners St. Joseph’s/Candler to help increase the number of physicians in this area of the state and beyond.” Interested in learning more? For more information about this exciting new development — simply reach out to Georgia Southern's Director of Communications Jennifer Wise at jwise@georgiasouthern.edu to arrange an interview today.
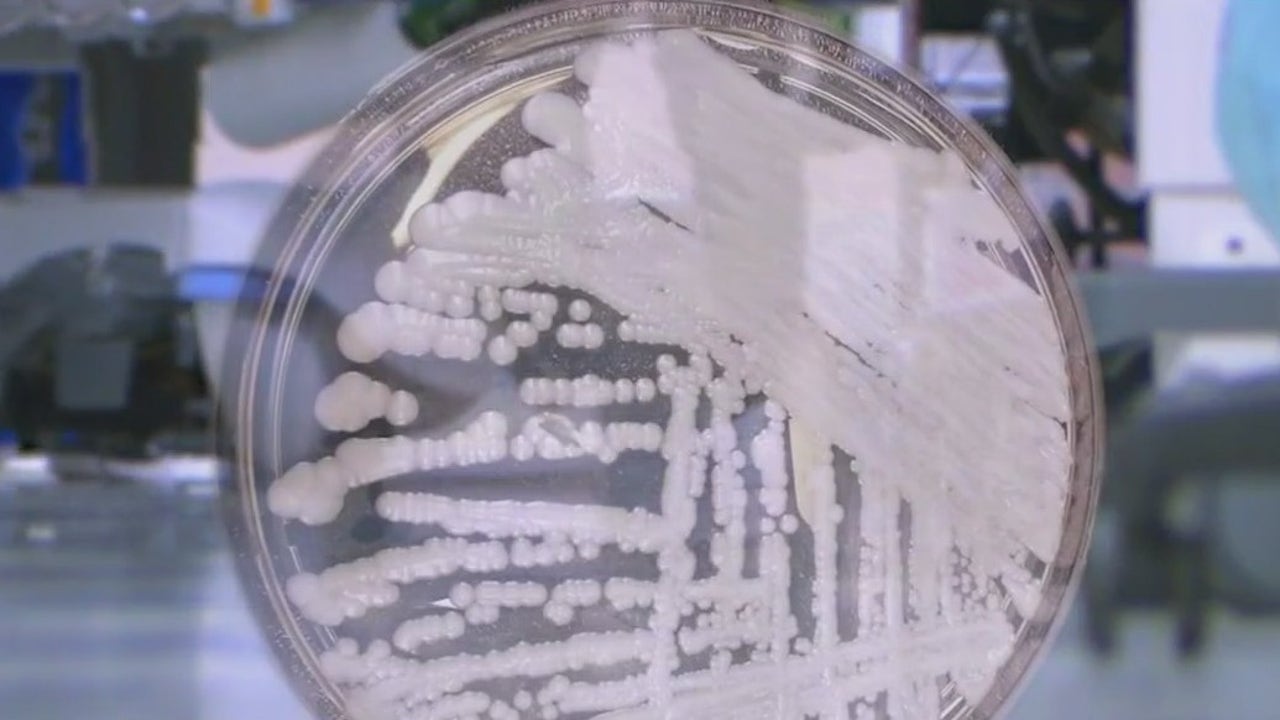
Candida auris: The deadly fungus is spreading and proving difficult to fight
Candida auris is making headlines - and for all the wrong reasons. The fungus can lead to severe infections causing long term health issues and even death. Recently, Fox News in Los Angeles was covering this emerging threat and reached out to Augusta University's Dr. Jose Vazquez for his expert insight and opinion. Here's the piece: The Centers for Disease Control & Prevention says Candida auris, or C. auris, is an emerging health threat, a type of fungus can cause severe, potentially life-threatening infections in people hospitalized with compromised immune systems. Dr. Jose Vasquez, chief of infectious diseases at the Medical College of Georgia at Augusta University, says there are several reasons for concern about this fungus. "The biggest fear is that it is multi-drug resistant," he says. "So, it is resistant to many different drugs." The CDC says most C. auris infections respond to antifungal medication, but some do not. Vasquez says C. auris is also hard to detect without highly specialized lab equipment that many hospitals do not have. And, he says, it is hard to stop the fungus once it gets into a hospital setting, such as an ICU or nursing care facility. C. auris can live on a person's skin without causing symptoms, allowing it to be transmitted from one person to another, or to get into a patient's body through contaminated surfaces or medical equipment like mechanical ventilators, feeding tubes and central lines. 'It is one of the Candidas that lives the longest on a surface, and we're talking about weeks," he sys. "So it can live there, dry and desiccated. Once it gets there, it kind of sets up shop, and it is very, very difficult to eradicate." The rest of the news story is attached: Looking to know more? That’s where Augusta University can help. Dr. Jose Vazquez, division chief and professor of Medicine at the Medical College of Georgia, is an expert in the realm of infectious diseases. He studies and treats infectious diseases, including antibiotic-resistant superbugs and fungal infections. He has been a reliable source for local, statewide and national media regarding the coronavirus outbreak. Dr. Vazquez is available to speak with media regarding this topic – simply click on his icon to arrange an interview.





