Experts Matter. Find Yours.
Connect for media, speaking, professional opportunities & more.

Covering Breast Cancer Awareness Month? Our experts are ready for your questions and coverage
October is Breast Cancer Awareness Month. Did you know that on average, every 2 minutes a woman is diagnosed with breast cancer in the United States. And according to the National Breast Cancer Foundation: In 2021, an estimated 281,550 new cases of invasive breast cancer will be diagnosed in women in the U.S. as well as 49,290 new cases of non-invasive (in situ) breast cancer. 63% of breast cancer cases are diagnosed at a localized stage (there is no sign that the cancer has spread outside of the breast), for which the 5-year survival rate is 99%. This year, an estimated 43,600 women will die from breast cancer in the U.S. Although rare, men get breast cancer too. In 2021, an estimated 2,650 men will be diagnosed with breast cancer this year in the U.S. and approximately 530 will die. 1 in 8 women in the United States will be diagnosed with breast cancer in her lifetime Breast cancer is the most common cancer in American women, except for skin cancers. It is estimated that in 2021, approximately 30% of all new women cancer diagnoses will be breast cancer. There are over 3.8 million breast cancer survivors in the United States. This year's theme is It's Time to Rise and the National Breast Cancer Foundation has a host of materials to watch and read for anyone looking to test themselves, find support or learn how they can help. If you're a journalist looking to know more about this topic or if you are covering Breast Cancer Awareness month - then let our experts help with your stories. Dr. Alicia Vinyard is a Board-Certified General Surgeon and Fellowship Trained Breast Surgical Oncologist at the Georgia Cancer Center and Medical College of Georgia at Augusta University. Dr. Vinyard is also an expert in breast cancer, cancer surgery and cancer survivorship. She is available to speak to media about Breast Cancer Awareness Month – simply click on her icon to now arrange an interview today.

GP guidance: Diet and weight loss to achieve type 2 diabetes remission
• Research finds diet and weight loss key to remission of type 2 diabetes • Experts conducted a critical narrative review of over 90 research papers including international clinical trials • Researchers advise on reducing blood sugar levels to manage negative effects of type 2 diabetes and reduce risk of complications Achieving ‘remission’ for people with type 2 diabetes through dietary approaches and weight loss should be the primary treatment goal of GPs and healthcare practitioners, concludes a large-scale review of clinical evidence led by researchers at UCL and Aston University. Type 2 diabetes (T2DM) is a serious condition caused when the body resists the insulin produced in the pancreas, and not enough insulin is made. This leads to high levels of sugar (glucose) in the blood and is associated with multiple health problems including increased risk of heart disease, blindness, and amputation. In the UK T2DM affects around 3.9 million people and 179 million globally. Care and treatment of T2DM costs the NHS around £10 billion a year. Corresponding author, Dr Duane Mellor, Aston University said: “Accounting for all the evidence, our review suggests remission should be discussed as a primary treatment goal with people living with type 2 diabetes. There are multiple dietary approaches that have been shown to bring about T2DM remission though at present meal replacements offer the best quality evidence. Low carbohydrate diets have been shown to be highly effective and should also be considered as a dietary approach for remission.” Lead author, Dr Adrian Brown, UCL Division of Medicine said: “Traditionally T2DM has focussed on managing a person’s blood glucose with medication, however the approach doesn’t address the underlying causes of T2DM. There is now a growing body of research that shows losing significant weight, 10-15kg, either through weight loss surgery or dietary approaches, can bring about type 2 diabetes remission (non-diabetic blood sugar levels).” For the study, published in the Journal of Human Nutrition & Dietetics, specialist dietitians and obesity experts conducted a critical narrative review of over 90 research papers covering international clinical trials and clinical practice data of dietary methods used to treat T2DM. The study found that meal-replacement diets helped around one in three (36%) people successfully achieve remission, while low carbohydrate diets were able to help around one in five (17.6 %) people achieve and maintain remission for at least two years. People who lost the most weight and kept the weight off using both of these dietary approaches were able to stay in remission. Calorie restricted and Mediterranean diets were also able to help people achieve remission – but at much lower rates. Only around 5% of people on calorie restricted diets stayed in remission after one year, while only 15% of people on a Mediterranean diet stayed in remission after a year. In reaching their findings, the research team had to account for the fact there is no single definition of remission; it is typically defined as a return to non-diabetic blood sugar levels (glycated haemoglobin less than 48mmol/mol), without the use of diabetes drugs. Other definitions however say weight (especially fat around the midsection) must be lost to achieve remission, and others that medications can continue to be used. In addition, some reports suggest low-carbohydrate diets can normalise blood sugar levels even without weight loss. This happens as when carbohydrates are eaten, they are broken down into sugars which cause our blood sugar levels to rise. A low-carbohydrate diet means less blood sugar appears in the bloodstream, leading to improved blood sugar control. However, if weight loss is not achieved but individuals are able to achieve non-diabetic blood glucose, the authors are suggesting this should instead be called mitigation, as the underlying mechanisms of T2DM are not being addressed. Dr Brown said: “The evidence is clear that the main driver of remission remains the degree of weight loss a person achieved. Therefore, for those not achieving weight loss but achieving a non-diabetic blood glucose we are suggesting this isn’t remission per se, but rather “mitigation” of their diabetes.” The research concludes that while weight loss appears to be the best predictor of remission success, it assumes fat loss from the pancreas and liver. They note, that it will be important for future studies to compare how these diets work for different ethnic groups, as T2DM can happen at lower body weights in different ethnic groups, who may have less weight to lose. Dr Mellor added: “Not everyone will be able to achieve remission, but people who are younger (less than 50), male, have had type 2 diabetes for less than six years and lose more weight are more likely to be successful. “This could be because these people are able to address the causes of their diabetes, therefore recovering more of the pancreas’s ability to make insulin and the liver’s ability to use it. But this doesn’t mean others won’t be successful if they improve their diet and lifestyle and lose weight. “Whether or not a person achieves remission, reducing blood sugar levels is important in managing the negative effects of type 2 diabetes and reducing risk of complications. But when it comes to choosing a diet, the most important thing is to pick one that suits you – one that you’re likely to stick to long term.” The initial meeting which led to the writing of this paper was supported by the British Dietetic Association and Diabetes UK.

Type 2 diabetes: more than one type of diet can help people achieve remission
Until recently, type 2 diabetes has mainly been managed by controlling risk factors – such as high blood pressure, cholesterol and blood sugar (glucose) levels – usually by prescribing drugs. But this approach doesn’t address the underlying causes of type 2 diabetes – such as problems with the hormone insulin no longer effectively controlling blood sugar. While taking drugs can help to manage blood sugar levels, it won’t help unpick the biological causes behind type 2 diabetes. A growing body of research shows that losing weight, either through surgery or dieting, can help address some of the underlying causes of type 2 diabetes. It does this by helping the body control blood sugar levels. This is significant as controlling blood sugar by improving how insulin is made and works is key to bringing type 2 diabetes into remission. Most of this body of research so far has looked at using meal-replacement shakes to help people with type 2 diabetes, which is why this approach may be prescribed by a doctor. But, more recently, researchers have begun investigating other diets – such as low-carbohydrate diets – in achieving remission. Although research in this area is still emerging, study results have so far shown a low-carbohydrate diet to be promising. To better understand which diets are best at helping people achieve type 2 diabetes remission, our recent review looked at over 90 papers describing the effects of various diets on type 2 diabetes. We found that although the better quality research tended to focus on meal-replacement shakes used in clinical trials, other approaches (such as low-carbohydrate diets) were also shown to work well. Join our readers who subscribe to free evidence-based news Our review found that meal-replacement diets helped around one in three people successfully achieve remission, while low carbohydrate diets were able to help around one in five people achieve remission. People who lost weight using both of these diets were able to stay in remission for up to two years if they maintained their weight loss. Low calorie and Mediterranean diets were also able to help people achieve remission – but at much lower rates. Only around 5% of people on low-calorie diets stayed in remission after one year, while only 15% of people on a Mediterranean diet stayed in remission after a year. Defining remission One of the big challenges we faced when writing our review was defining what “remission” is. Knowing how to define it was important so we could understand which diets worked best in helping people achieve remission. The reason this was difficult is because the definition varies between different expert groups and research studies. Most define remission as a reduction of blood sugar levels below the range to diagnose diabetes – but some definitions state that this needs to be done without the use of drugs, while others do not. Other definitions say weight (especially fat around the midsection) must be lost to achieve remission. Another challenge we faced when defining remission was that some reports suggest low-carbohydrate diets can normalise blood sugar levels even without weight loss. This happens because when we eat carbohydrates, they’re broken down into sugars which cause our blood sugar levels to rise. A low-carbohydrate diet means less blood sugar appears in the bloodstream, leading to improved blood sugar control. For that reason, we initially defined remission using the definition each study used. Then, we compared the numbers of people whose blood sugar levels normalised without drugs for at least six months – which most consider to be true remission. Mitigation v remission While low-carbohydrate diets help people achieve remission, there’s concern that blood sugar levels could potentially rise again as soon as more carbohydrates are eaten. This is why we suggest in our review that rather than call this remission, it should perhaps be called “mitigation of diabetes”, as type 2 diabetes is still present – but the negative effects are being well managed. We think that remission can only be achieved if fat is lost from around the organs. This allows insulin to be made and used effectively again. But because carbohydrates are also a major energy source in our diet, eating less of these often results in consuming fewer calories – which typically results in weight loss. So if someone is able to maintain a low-carbohydrate diet long term, they will not only reduce blood sugar levels and risk of complications for their diabetes, but may also achieve remission. Regardless, the evidence that we looked at in our review made clear that there are many ways a person can significantly improve their blood sugar levels through diet – and that this can lead to remission in many cases. The key thing we found with each type of diet is that at least 10-15kg of body weight needed to be lost to achieve remission. However, although weight loss seems to be the best predictor of success, it assumes fat loss from the pancreas and liver. It will be important for future studies to compare how these diets work for different ethnic groups, as type 2 diabetes can happen at lower body weights in different ethnic groups, who may have less weight to lose. Not everyone may be able to achieve remission, but people who are younger (less than 50), male, have had type 2 diabetes for less than six years and lose more weight are more likely to be successful. This could be because these people are able to reverse the causes of their diabetes, recovering more of the pancreas’s ability to make insulin and the liver’s ability to use it. But this doesn’t mean others won’t be successful if they improve their diet and lifestyle, and lose weight. Whether or not a person achieves remission, reducing blood sugar levels is important in managing the negative effects of type 2 diabetes and reducing risk of complications. But when it comes to choosing a diet, the most important thing is to pick one that suits you – one that you’re likely to stick to long term.

Clinical trials to combat short sightedness in children underway at Aston University
Clinical trials to treat myopia - or short sightedness - in children are now underway. They are being conducted by researchers from Aston University in partnership with industry and in collaboration with the Universities of Queens, Ulster, Glasgow Caledonian, Anglia Ruskin, Waterloo and TU Dublin, with one of the trials funded by the National Institute for Health Research (NIHR). The myopia research team in the College of Health and Life Sciences at Aston University is recruiting children between the ages of six to 15 years old, to take part in the clinical studies, which involve a range of different interventions that aim to slow the progression of myopia in children. The interventions under trial include low dose atropine eye drops, contact lenses and spectacle lenses. Myopia is an eye condition where distant objects appear blurry. It typically occurs in childhood and progresses through the teenage years. It can lead to eye disease in later life, as the eye grows longer with myopia, it causes stretching in parts of the eye. Myopia is becoming increasingly prevalent throughout the world and it has been predicted to affect approximately 50 per cent of the world's population by 2050, based on trending myopia prevalence figures. Myopia is an overlooked but leading cause of blindness, particularly among the working age population. At present, different designs of soft contact lenses, orthokeratology contact lenses (lenses worn overnight to correct the myopia), novel spectacle lenses and eye drops are all being used to slow eye growth and myopia progression in children. The aim in this trial is to manage myopia with an intervention at a young age in order to maximise the impact on slowing down the progression of myopia. Lead researcher professor, Nicola Logan, said: “Myopia is often considered benign because the blurred vision is easily corrected with glasses, contact lenses or refractive surgery. Higher levels of myopia are associated with increased risk of pathological complications, but it is important to note that there is no safe level of myopia. Even low levels of myopia increase the risk of sight-threatening eye conditions. “We are at an exciting time whereby we now have interventions based on research evidence that can be used in clinical practice that will help to slow down the rate of progression of myopia. “In these trials we want to find out the impact of different interventions on myopia progression in UK children, as well as look at why myopia develops and how it progresses in children, to see if we can enhance the current interventions. New information may be used to make the myopia control interventions more effective.” The researchers are aiming to recruit around 200 children aged between six and 15 years old across the three trials by 2021. If you are a parent or guardian of children who have myopia and feel this may be suitable for your children, then you can contact the research team at myopia@aston.ac.uk or (+44)121 204 4100 for further information.

New CBS Sitcom "United States of Al" Taps Experience of Social Work Student and Veteran
On April 1, 2021, CBS premiered United States of Al - a new comedy from producer Chuck Lorre (Two and a Half Men, Big Bang Theory) about a Marine combat veteran struggling to readjust to civilian life and the interpreter who served with his unit in Afghanistan and has just arrived to start a new life in America. The show explores the relationship between these two men and how they help each other adjust to their new lives. So, what does a CBS sitcom have to do with the USC Suzanne Dworak-Peck School of Social Work? Enter Master of Social Work (MSW) student Josh Emerson, who landed in the right place at the right time through his field internship at No One Left Behind. No One Left Behind (NOLB) is an all-volunteer, national nonprofit organization that supports recipients of the Special Immigrant Visa (SIVs), and those pursuing an SIV. The founders of No One Left Behind believe the U.S. has a moral obligation to protect these interpreters, and their families, who served side-by-side with American soldiers. Emerson, a veteran of the U.S. Army who deployed to Iraq and Afghanistan, is very familiar with Iraqi and Afghan interpreters. “I went on missions with these interpreters, got to know them, built relationships with them,” he said. “I was so very happy to be able to work with them in this capacity. In addition to providing resources for SIV ambassadors living in the United States, NOLB advocates on behalf of the SIV population to the executive and legislative branches of government provides subject matter expertise to the media, and partners with U.S. businesses to provide opportunities for what they call “this next generation of Americans.” Alea Nadeem, MSW ’15, is a board member of NOLB and reached out to USC with a field internship opportunity for social workers to do macro-level clinical work in a nonprofit setting. Nadeem became Emerson’s field instructor. “What Josh has brought to No One Left Behind has never been brought to the board before,” Nadeem said. “They now see the value in social work.” Bringing the issue to a larger audience Chase Millsap, a consultant and writer on United States of Al, is a former board member of No One Left Behind. “I am still very supportive, impressed and proud of all the work the NOLB team does on a daily basis,” he said. A veteran of the U.S. Marine Corps and U.S. Army Special Forces, he holds a master’s degree from USC Sol Price School of Public Policy. "USC helped me to learn the tools about how to connect entertainment and policy,” Millsap said. “United States of Al is a perfect example of those two worlds coming together in a powerful (and funny) way.” Millsap’s idea was to bring the issues around SIVs into America's living rooms, in a way that would make them relatable. Emerson’s experience as a veteran, his clinical and project management skills obtained through his social work studies and his stellar ability to work one-on-one with SIV recipients and applicants allowed him to inform the show’s stories with a wide breadth of knowledge. Emerson joined James Miervaldis, chairman of the NOLB board, in helping the writers and actors on the show understand the SIV issues, the ways in which NOLB provides assistance and advocacy, and sharing funny stories of cultural differences between Afghans and Americans. Emerson and Miervaldis have also been able to include some of NOLB’s SIV ambassadors in the process, those with an SIV who have already established themselves in the U.S. and are contracted by NOLB to help others assimilate. “They’re talking to the exact people they're portraying,” Emerson said. Nadeem sees Emerson’s contribution to the show as another platform through which to educate. “There are a lot of different tentacles to social work, and it may not seem like the most obvious place in TV and film, but it is,” she said. The show itself touches on everything social workers value ― service, challenging social injustice, dignity and worth of a person, the importance of human relationships and integrity. “This just makes so much sense that a social worker would be involved in this show because that's what we're always trying to communicate to a larger audience,” Nadeem said. “Through this show, you can make a greater impact for these folks to sort of assimilate them to be American citizens, and then also have the whole world appreciate their culture and appreciate what they've done for our nation to keep U.S. service members safe.” A valued member of the team Emerson, a father of five who resides in New Hampshire, knew he wanted to work with veterans after leaving military service. He felt that an MSW was the most versatile degree for this and chose the USC Suzanne Dworak-Peck School of Social Work because of its military social work track. “I think to be a good social worker you need to have experience in life,” Emerson said. “To have seen some things, or been through some things, to understand the population you're dealing with and what they're going through.” When Emerson began his internship at NOLB in 2020, Miervaldis immediately began working with him to focus on SIVs who recently had come to the United States. The first case Miervaldis assigned to Emerson was an SIV family with two young children who needed emergency surgery at a specialty hospital in Washington D.C. “This SIV packed up his family, his pregnant wife and the two kids, used up all his money to take them by bus from Texas to D.C. in the middle of a pandemic and ended up in a bad part of town,” Miervaldis said. As the SIV’s assigned caseworker, Emerson established a relationship and trust with the SIV, helped him obtain safe housing and a job interview, and coordinated details for the children’s surgery with the hospital. “He’s gone and done everything,” Miervaldis said. “We are very proud of Josh’s initiative and empathy for a family in such need. No One Left Behind is the safety net for our allies.” Last year, NOLB helped over 600 families with visas and resettlement. “Josh has exceeded all our expectations and done so while communicating with clients who speak in broken English, Dari and Pashtu, struggling during a pandemic,” Miervaldis said. “His professionalism and empathy are great credits to USC. We would not be where we are today without him. That is not hyperbole.” Miervaldis hopes NOLB will have more social work interns from USC to continue Emerson’s work. For him, Emerson’s project management skills have been the greatest asset, creating a new process for how NOLB provides help for SIV families. “We told Josh, you're a pathfinder, you're a pioneer,” Miervaldis said. “We need to figure out very quickly what works, what doesn't work, and he took it and said, ‘okay, point me in the right direction.’ He’s very much valued as a member of the team.” From advocacy to TV No One Left Behind gets about 20 messages every day from Iraqi or Afghan interpreters who served with U.S. forces in their countries, and who now receive daily death threats from the Taliban. “They're not allowed to live in their homes or their neighborhoods anymore because they helped the U.S.,” Emerson said. “Now the U.S. is withdrawing from all these countries, and the Taliban and terrorist activities in general are picking up, and these people are getting pressured and killed. NOLB has over 300 cases of SIVs who have been killed waiting for their visas.” Emerson hopes that the added exposure from United States of Al will bring awareness particularly to service members about what these interpreters are experiencing and how they can help. One of the requirements for an SIV is a letter of recommendation from the U.S. service member with whom they served, and those have been the most difficult items for SIV applicants to secure. “I have been able to provide some input to what should be addressed in the show,” Emerson said. “It's interesting to see how advocacy on an issue can turn into something this large scale.” See more news from USC Suzanne Dworak-Peck here.
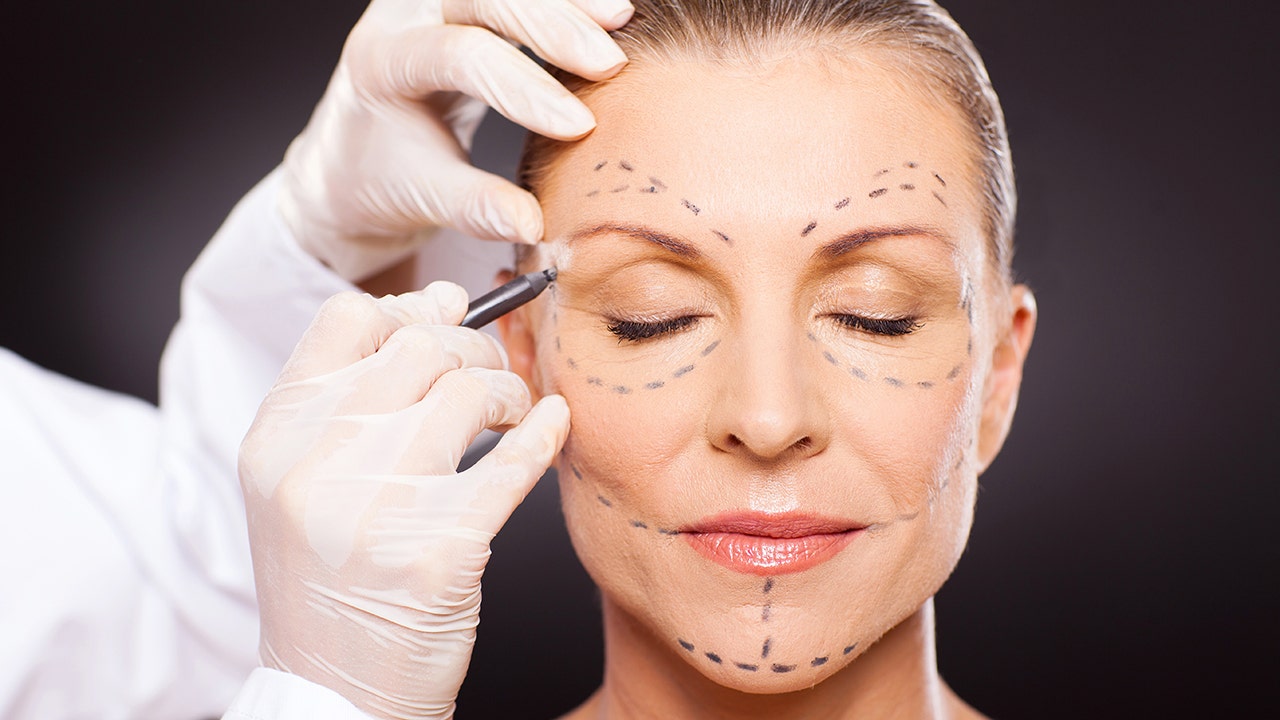
The Zoom Boom? More and more Americans are getting plastic surgery – let our expert explain why
After almost a year where most American offices went unused, experts are noticing an unexpected side effect from all those online meetings. It appears that prolonged exposure to seeing yourself in that tiny box during video calls is inspiring a sudden uptick in plastic surgery. The plastic surgery industry is booming during the coronavirus pandemic, largely due to the increase in the number of virtual meetings offered through Zoom and other video web services. Call it the “Zoom boom.” The interest in cosmetic surgery is boosting appointments for Botox, lip fillers and other plastic surgery procedures that help people feel more attractive on computer screens, according to Dr. Maria Helena Lima, an assistant professor of Surgery for the Section of Plastic and Reconstructive Surgery in the Medical College of Georgia at Augusta University. “In the last few months, there has been a jump in the number of patients wanting plastic surgery procedures,” said Lima. “We have discovered that when people are in Zoom meetings, they should be listening to the content and paying attention to what’s going on, but they’re not.” Lima says participants are oftentimes looking at themselves on the screen and wondering what could be done to alter their image. It is a trend that offers up some interesting questions: • Along with the Zoom boom, are there other reasons people are opting to go under the knife for an elective procedure? • Are there long-term consequences to these decisions? • What do patients need to know first to avoid any safety or health issues? There’s a lot to know about this topic, and if you are a journalist looking to learn more, then let us help with your coverage. Dr. Maria Helena Lima is one of the nation’s leading plastic surgeons with 12 years of experience specializing in aesthetic plastic surgery, facial reconstruction and craniofacial pediatric plastic surgery. She is available to speak with media about this emerging trend. Simply click on her name now to arrange an interview today.

This week’s shocking news of golf legend Tiger Woods rolling his vehicle and sustaining serious injuries to his right leg have sports fans, journalists and most of the world watching and waiting for word of whether he’ll play again. According to ESPN, the injuries are extensive: Tiger Woods is recovering from a lengthy surgery to repair what a doctor said Tuesday night were "significant orthopaedic injuries to his right lower extremity" suffered in a single-car rollover crash hours earlier on a steep roadway in a Los Angeles suburb. As part of a statement on Woods' official Twitter account, Dr. Anish Mahajan of Harbor-UCLA Medical Center updated the famed golfer's condition, saying in part that Woods had multiple "open fractures" to his lower right leg, and he had a rod placed in his tibia and screws and pins inserted in his foot and ankle during an emergency surgery. "Comminuted open fractures affecting both the upper and lower portions of the tibia and fibula bones were stabilized by inserting a rod into the tibia," said Mahajan, the chief medical officer and interim CEO at Harbor-UCLA. "Additional injuries to the bones of the foot and ankle were stabilized with a combination of screws and pins. Trauma to the muscle and soft-tissue of the leg required surgical release of the covering of the muscles to relieve pressure due to swelling." ESPN – February 23 If you’re a journalist looking to know more about this type of injury, what the recovery process usually involves and what the long-term prognosis may be – then let us help. Dr. Monte Hunter serves at Augusta University as the Satcher Distinguished Chair of the Department of Orthopedic Surgery and director of the Sports Medicine Program. Dr. Hunter is an expert in reconstruction and sports injury prevention – and he is available to speak with media about this topic. Simply click on his icon now to arrange an interview today.
Virtual Reality-Based Surgical Simulations Could Make Patients Safer
Suvranu De, the director of the Center for Modeling, Simulation, and Imaging in Medicine at Rensselaer, has dedicated more than a decade of research to making surgery safer by developing virtual reality-based surgical training simulations that closely mimic the optics and haptics a surgeon may encounter in the operating room. A new $2.3 million grant from the National Institute of Biomedical Imaging and Bioengineering of the National Institutes of Health will further his research in this space, by supporting the development of a collaborative virtual reality-based surgical simulation environment that allows medical professionals to practice technical, cognitive, and interpersonal skills as a team. “People will be wearing head-mounted displays, and they will be immersed in a virtual operating room working on a virtual patient as a team,” De said. “We want to have an expert team in the operating room focused on the treatment of a patient, and not just a team of experts.” Conceptually, this approach is similar to crew resource management practiced by aviation pilots, which has led to a significant reduction in aircraft accidents. The Virtual Operating Room Team Experience (VORTeX) simulation system will provide realistic distractions, interruptions, and other stressors that medical professionals may encounter in an operating room. Traditionally, this type of simulation training has required mannequins, instructors, and a dedicated space, as well as significant coordination and resources. In contrast, the VORTeX system will be both distributed and asynchronous – allowing participants to join the simulation from different locations, and instructors to review the simulation and provide feedback at their convenience. Machine learning algorithms will be used to crunch the data and provide feedback to participants, who will be able to return to the virtual environment to review their performance. De is available to discuss how this type of virtual training is developed and implemented.

Gene therapy and the next frontier of medicine
Genetic testing today is mainstream, marketing to consumers who want to know where in Europe they came from or what types of hereditary diseases they could develop. For around $200 you can trace your family tree to learn your origins or identify genetic abnormalities that could signal disease. James Dahlman, assistant professor in the College of Engineering’s biomedical engineering department, specializes in genetics and believes these genotyping services can be helpful, as long as they are used responsibly. “If you’re going to start making medical predictions, you have to be careful,” said Dahlman. “Most people are not equipped to interpret statistics correctly, which can lead to negative predicting and ethical dilemmas. In a few years, genetic counselors will be in high demand so folks can make better decisions about their health.” Dahlman is fascinated by genetics, citing gene therapy as the most interesting field in the world. And it’s a field that he is revolutionizing through his research. Gene therapy is an experimental technique that uses genes to treat or prevent diseases, including hemophilia, Parkinson’s, cancer and HIV. It can help manage a number of diseases by leveraging genes instead of drugs or surgery. Although gene therapy shows promise, there are still risks involved, including unwanted immune system reactions or the risk of the wrong cells being targeted. That’s where Dahlman’s research comes in. Dahlman’s lab focuses on drug delivery vehicles, which are nanoparticles. The nanoparticle delivers gene therapies to the right place in the body to fight disease. It’s critical that the gene therapies only target the unhealthy cells to avoid damaging healthy ones. Dahlman is laser focused on ensuring the nanoparticles know what paths to take to reach the correct organ to start the healing process. “The issue with genetically-engineered drugs is that they don’t work unless they get to the right cell in the body,” said Dahlman. “You can have the world’s best genetic drug that's going to fix a tumor or eradicate plaque, but it’s not going to be effective unless it travels to the right organ. In my lab, we design different nanoparticles to deliver the genetically-engineered drugs to the correct location.” The field of genetic therapy is fascinating – and if you are a journalist looking to cover this topic or have questions for upcoming stories – let our experts help. James Dahlman is an Assistant Professor in the Georgia Tech BME Department. He is an expert in the area of biomedical engineering and uses molecular biology to rationally design the genetic drugs he delivers. This research is redefining the field of genetic therapy. Dr. Dahlman is available to speak with media – simply click on his icon to arrange an interview.

October is Breast Cancer Awareness Month – Let our experts help with your coverage
October is Breast Cancer Awareness Month and if you are a reporter looking to know more or considering covering this topic, here are a few key facts to get started according to Breastcancer.org: About 1 in 8 U.S. women (about 12%) will develop invasive breast cancer over the course of her lifetime. In 2019, an estimated 268,600 new cases of invasive breast cancer are expected to be diagnosed in women in the U.S., along with 62,930 new cases of non-invasive (in situ) breast cancer. About 2,670 new cases of invasive breast cancer are expected to be diagnosed in men in 2019. A man’s lifetime risk of breast cancer is about 1 in 883. About 41,760 women in the U.S. are expected to die in 2019 from breast cancer, though death rates have been decreasing since 1989. For women in the U.S., breast cancer death rates are higher than those for any other cancer, besides lung cancer. Besides skin cancer, breast cancer is the most commonly diagnosed cancer among American women. In 2019, it's estimated that about 30% of newly diagnosed cancers in women will be breast cancers. In women under 45, breast cancer is more common in African-American women than white women. A woman’s risk of breast cancer nearly doubles if she has a first-degree relative (mother, sister, daughter) who has been diagnosed with breast cancer. Less than 15% of women who get breast cancer have a family member diagnosed with it. At Augusta University, we have leading experts who can help with any of your questions, assist with your coverage and ensure your story has all the facts and details it requires to be a compelling and effective piece. Dr. Alicia Vinyard is a Board-Certified General Surgeon and Fellowship Trained Breast Surgical Oncologist at the Georgia Cancer Center and Medical College of Georgia at Augusta University. Dr. Vinyard is also an expert in breast cancer, cancer surgery and cancer survivorship. She is available to speak to media about Breast Cancer Awareness Month – simply click on her icon to arrange an interview.





