Experts Matter. Find Yours.
Connect for media, speaking, professional opportunities & more.

Assessing and Treating Heat-Related Illness in Children
Dangerously high global temperatures require an abundance of caution and preparation, especially when it comes to protecting the littlest members of society. Villanova University associate professor of nursing Michelle Kelly, PhD, CRNP, CNE, is an expert in pediatric healthcare, and she recently shared some tips for preventing and treating heat-related illness in children. Q: First, what is heat exhaustion? Dr. Kelly: Heat exhaustion is a slowly progressing condition that begins as one is exposed to increased temperatures for extended periods of time without the proper precautions. Ultimately, heat exhaustion can become heatstroke, which always requires immediate intervention. Q: What are the signs of heat exhaustion? DK: Signs of heat exhaustion include increased thirst, nausea, vomiting, irritability, headache, increased sweating, fainting, weakness, extreme tiredness and muscle cramps. The child will have cool and clammy feeling skin, with an elevated body temperature, but it will be below 105 degrees Fahrenheit (40.5 degrees Celsius). Q: When does heat exhaustion become heatstroke? DK: With heatstroke, the above symptoms progress to severe headache, weakness, dizziness, confusion, fast breathing and increased heart rate. The child will feel flushed—hot, with dry skin, little to no sweating—and may pass out or have a seizure, due to the body temperature exceeding 105 degrees Fahrenheit. This child needs immediate intervention aimed at decreasing the child’s body temperature. Q: What should caregivers do when a child experiences heat-related illness? DK: Interventions that a family can begin while getting the child emergency treatment include getting the child to lie down with feet elevated indoors or in shade. Remove excess clothing. Apply lukewarm water to the skin either with a wet cloth or spray bottle. If the child is awake, give sips of cool clear fluids. If the child is vomiting, keep the child on their side to prevent choking. Emergency treatment will include continuing to decrease the child’s body temperature, giving fluids (by mouth or with intravenous fluids), and monitoring for seizures. Q: Any tips for prevention? DK: Plan ahead if you and your children will be outside during this extreme heat. Wear light colors and plan for some sort of shade if possible. Try to arrange outdoor activities to take place in the early morning or evening, not during the heat of the day. Or better yet, spend time in a pool or indoors in air conditioning. If your child will be participating in sports during a heatwave, start hydrating 24 hours before to prevent the risk of dehydration. This means making sure they have had adequate fluids before competing, during the competition and afterward to recover. Water is the best liquid, but an alternative would be low-sugar-containing electrolyte solutions designed for children (such as Pedialyte). Stay safe!

VANCOUVER IMAGING TO IMPLEMENT REALTIME MEDICAL AI
ORIGINALLY PUBLISHED IN CHT MAGAZINE VANCOUVER – Vancouver Imaging, a group of over 70 radiologists, has signed on to use RealTime Medical’s smart workload-balancing, physician skills development and error-avoidance platform. Vancouver Imaging, which provides reading services for hospital and out-of-hospital imaging centres, will implement the system in the first half of 2020 at its non-hospital clinics. Vancouver Imaging offers a wide variety of sub-specialty readings across all disciplines, including specialized expertise in emergency trauma radiology. The organization is the only group of radiologists in Canada offering around-the-clock, on-site, sub-specialty emergency reading services. “Emergency radiology is itself a sub-specialty and requires a unique set of skills,” said Dr. Savvas Nicolaou (pictured), the CEO of Vancouver Imaging and director of Emergency & Trauma Imaging at Vancouver General Hospital. “It’s unpredictable, with frequent interruptions. You often have to work with a limited amount of information from clinicians, and it can include everything from head-to-toe, including mass casualty situations that require proactive decision-making.” He added, “You’re always on, and never off.” The Emergency & Trauma sub-specialty requires “appropriate, patient-centered judgement in a matter of seconds.” Vancouver Imaging will deploy RealTime Medical’s AICloudWorks and AICloudQA platforms within their clinics. Collectively, the offerings encompass several AI applications, including high throughput workload balancing. RealTime Medical holds the U.S. and Canadian patents for its workload balancing algorithms and is one of only two patent holders for diagnostic workload balancing, along with the U.S. company, Virtual Radiologic. The cases are assigned to the appropriate radiologists based on sub-specialty, current workload and other parameters, creating an intelligent, diagnostic operations platform that is “context-aware,” a term originally coined by RealTime Medical to describe the capabilities of the platform. For example, radiologists with expertise in neurology will be the first to receive neuro cases, while thoracic or pediatric experts will be the first to receive cases of that type. The system also “balances” the work, to ensure that radiologists are receiving equal caseloads, subject to the case-specific service levels and business parameters established by the group. “The AI additions to this proven platform make it even more advantageous for us as a group as we pursue the delivery of Emergency Radiology services globally,” said Dr. Nicolaou, a world-renowned expert in Emergency & Trauma radiology, often referred to as the Founder and Pioneer of Emergency/Trauma Radiology in Canada. Dr. Nicolaou noted that AICloudWorks is vendor-neutral and can work with any HL7 and DICOM-based HIS, RIS and PACS solutions. “PACS integration can be very problematic,” said Dr. Nicolaou. “Being vendor-neutral is important to our flexibility as a group.” Vendor neutrality is important to Vancouver Imaging as their current environment includes workflows across multiple PACS solutions. Download CHT Reprint of Full Article

The health and safety of their children is the top priority of every parent. And after more than a year and a half of enduring a pandemic, mothers and fathers across America have been inundated with news, information and debate about what’s best for all of our health and how to avoid contracting COVID-19. And now, as America is seeing vaccines approved for children five and over, parents and the media are relying on leading experts to provide honest guidance, advice, and clarity on what parents need to know about what’s best for the health of America’s kids. It’s why Dr. Jody Terranova, a physician at UConn Health and the president-elect for the Connecticut chapter of the American Academy of Pediatrics, is getting the word out to parents: The state of Connecticut is already rolling out vaccinations for children ages five to eleven. This move comes on the heels of the CDC's formal recommended emergency use authorization. Within hours of the announcement, children here have rolled up their sleeves. One UConn School of Medicine pediatrician says she understands why parents have questions and hopes to clarify a few important details. Not only is Dr. Jody Terranova the president-elect for the Connecticut chapter of the American Academy of Pediatrics, she was also a member of the scientific sub-group of the state of Connecticut governor’s COVID-19 vaccine advisory group. “At this point, we are really recommending that all five to eleven-year-olds get vaccinated. There are very few children that should not get vaccinated right now," Dr. Terranova explained. Dr. Terranova admits the topic of vaccines for children ages five to eleven is a sensitive issue. That’s why in order to make an informed decision for your family, it's critical to ask important questions, like how does the vaccine work to protect the pediatric population from COVID-19? “The vaccine that we are giving for COVID works very similar to other vaccines, where it’s really activating your immune system to mount a response to recognize that virus when it invaded your body and create antibodies that will attack it so that it can’t replicate and infect you or your child," continued Dr. Terranova. November 4 - Eyewitness News If you are a journalist looking to know more about the COVID vaccine for children and the important information parents need to know, let us help with your coverage. Dr. Terranova is available to speak with media – simply click on her icon to arrange an interview today.
/cloudfront-us-east-1.images.arcpublishing.com/gray/EQ34NHJNIVCAVDO6SOO4FDJHRE.jpg)
As America continues down the long road of adapting, adjusting, and advancing safety efforts in order to overtake COVID 19 – vaccinations have now been approved for children five and older. It’s welcome news for health care experts and epidemiologists – but there’s no doubt this most recent development has parents concerned about the safety and potential consequences children could face if they roll up their sleeves to get immunized. Since this next step was announced, it’s gotten the attention of media and parents from across the country. Augusta University experts have been front and center to help with the messaging. The vaccine rollout for kids ages 5 to 11 starts now. Right now, local hospitals and pediatric offices are working to get doses to the river region. For the past nine months, we’ve seen different rollouts for different age groups come through Augusta University Health’s mass vaccination site. AU Health says it’s still up in the air right now whether this will be the main site you’ll bring your kids to get vaccinated. But what we do know is that 1,200 doses are on the way. “Every single individual has been paramount in this response,” said Dr. Joshua Wyche, AU vaccine coordinator. AU Health officials say they aren’t even close to accomplishing their mission to get everyone vaccinated. “We’re very fortunate to have caregivers that care so much about their community that want to make this impact and continue to push through during this pandemic,” Wyche said. November 03 - WRDW/WAGT Augusta An update from the CDC: kids can start rolling up their sleeves to get their COVID-19 vaccine. This means nearly 30 million American children ages five to 11 are now eligible for the vaccine. That's a little under 1 million in Georgia and 450,000 in South Carolina. But some parents still have concerns about the vaccine's safety. “For the vast majority of people and for parents as they’re looking for how they can protect they’re children best from COVID-19, having access to the vaccine now gives them another tool to protect their child,” says Augusta University Strategic Planning & Pharmacy VP Dr. Joshua Wyche. November 03 – Fox News Child vaccinations are an important topic – and it is essential that accurate details and information are shared with media and parents across the country, and that’s where Augusta’s experts can help. Dr. Joshua Wyche is accomplished pharmacist with an extensive background in business management. He is an expert in strategic planning and pharmacy services. Dr. Wyche is available to speak with media regarding this important topic – simply click on his icon now to arrange an interview today.
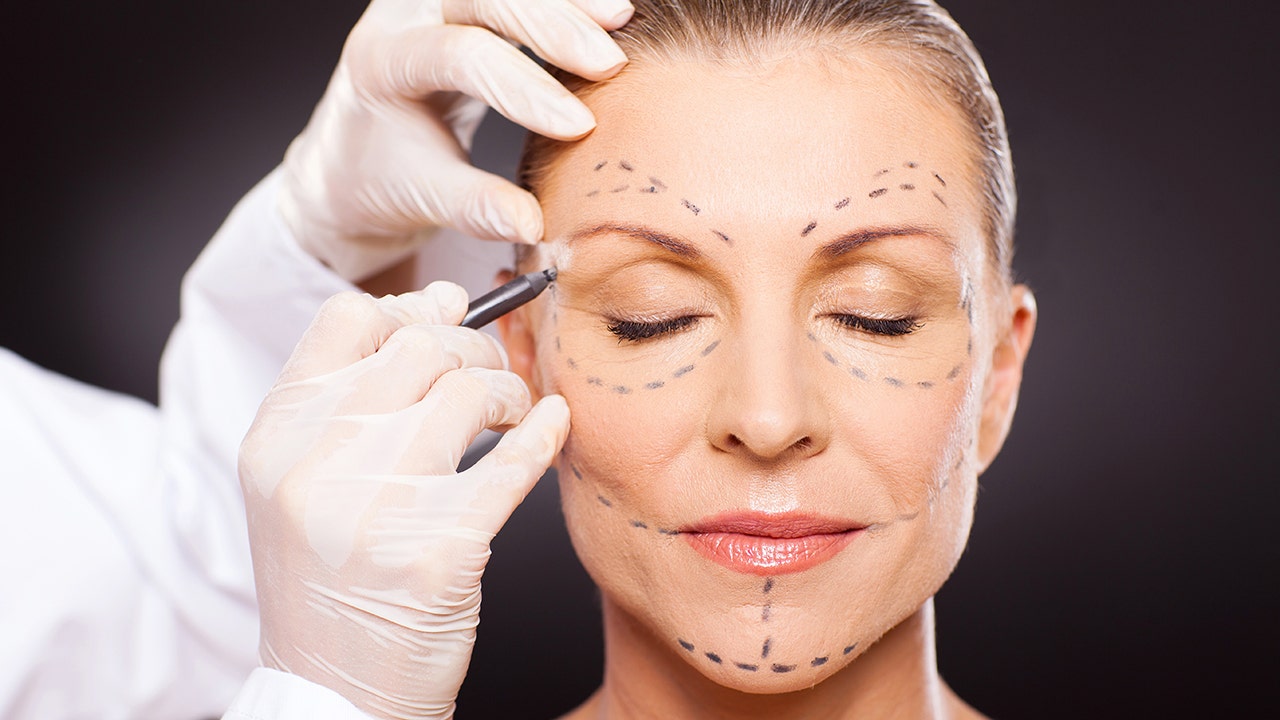
The Zoom Boom? More and more Americans are getting plastic surgery – let our expert explain why
After almost a year where most American offices went unused, experts are noticing an unexpected side effect from all those online meetings. It appears that prolonged exposure to seeing yourself in that tiny box during video calls is inspiring a sudden uptick in plastic surgery. The plastic surgery industry is booming during the coronavirus pandemic, largely due to the increase in the number of virtual meetings offered through Zoom and other video web services. Call it the “Zoom boom.” The interest in cosmetic surgery is boosting appointments for Botox, lip fillers and other plastic surgery procedures that help people feel more attractive on computer screens, according to Dr. Maria Helena Lima, an assistant professor of Surgery for the Section of Plastic and Reconstructive Surgery in the Medical College of Georgia at Augusta University. “In the last few months, there has been a jump in the number of patients wanting plastic surgery procedures,” said Lima. “We have discovered that when people are in Zoom meetings, they should be listening to the content and paying attention to what’s going on, but they’re not.” Lima says participants are oftentimes looking at themselves on the screen and wondering what could be done to alter their image. It is a trend that offers up some interesting questions: • Along with the Zoom boom, are there other reasons people are opting to go under the knife for an elective procedure? • Are there long-term consequences to these decisions? • What do patients need to know first to avoid any safety or health issues? There’s a lot to know about this topic, and if you are a journalist looking to learn more, then let us help with your coverage. Dr. Maria Helena Lima is one of the nation’s leading plastic surgeons with 12 years of experience specializing in aesthetic plastic surgery, facial reconstruction and craniofacial pediatric plastic surgery. She is available to speak with media about this emerging trend. Simply click on her name now to arrange an interview today.

As battle-weary Americans struggle to emerge from the anxiety and worry of COVID-19, there might be even more bad news around the corner this fall for parents of young children. The U.S. Centers for Disease Control and Prevention (CDC) is sounding the alarm now about increased cases of acute flaccid myelitis (AFM) in the coming fall. It is of a rare but serious polio-like condition that surfaces every two years and children under five are its main target. On average, patients during the last outbreak in 2018 were aged 5 years old. Limb weakness and paralysis is the most common symptom of the condition which affects the nerve cells in the gray matter of the spinal cord. Others include a fever, pain, or numbness in one or more limbs, problems walking normally, a headache, back or neck pain, issues with swallowing or talking, and weakness in the face or neck. Patients may also have had a recent or current respiratory illness. August 05 - Newsweek In what has already been a harrowing year, it looks like there may be another serious health concern on the horizon. And if you are an expert covering children’s health the potential for acute flaccid myelitis to peak in 2020 – then let our experts help. Dr. Elizabeth Sekul is a highly acclaimed pediatric neurologist specializing in electrodiagnostic medicine and neuromuscular diseases. She also works as an associate professor at the Medical College of Georgia's Department of Neurology and the Department of Pediatrics and Child Neurology. If you are a journalist looking to book an interview – simply click on Dr. Sekul’s icon and arrange a time today.

The global pandemic of COVID-19 is no longer just daily news, it is pretty much the only news happening right now across America and most of the globe. Reporters and journalists are working hard to cover this story that is changing and progressing almost exponentially by the day. There are multiple angles to consider, and each storyline is just as important as the other when it comes to informing the public and ensuring that the correct and proper facts are relayed to an audience that is concerned, curious and waiting for answers. If you are a journalist covering COVID-19 – then let our team of experts help. Our experts can assist with and answer your questions about transmission, vulnerable populations and age groups, prevention and how the medical system is handling this outbreak. Emi Minejima is an Assistant Professor of Clinical Pharmacy at USC School of Pharmacy and an expert in infectious diseases pharmacotherapy and antimicrobial stewardship. She is an infectious diseases specialist at LAC+USC Medical Center. Irving Steinberg is the Associate Dean for Faculty Affairs & Associate Professor of Clinical Pharmacy and Pediatrics at USC School of Pharmacy and Keck School of Medicine. He is a pediatric pharmacist at LAC+USC Medical Center and an expert in the areas of predictive performance of pharmacokinetic models for dosing in children. Annie Wong-Beringer is the Associate Dean for Research and Graduate Education & Professor of Clinical Pharmacy at USC School of Pharmacy and an expert in bacterial resistance and virulence, host microbial interactions and host immune response. All three experts are available and ready to speak with reporters – simply click on an individual's icon to make contact and arrange an interview.

Pharmaceutical aerosols are painless, fast-acting and less likely to cause side effects than medicines delivered via pills or injections. Yet inhaled therapies are often avoided because of the challenges associated with targeting how aerosol particles are deposited within the lung. “Current inhalers produce fairly large particles, so approximately 90 percent of the medication gets lost in the mouth and throat. It’s swallowed and wasted. This prevents many medications from being delivered through the inhalation route, even though there are a number of advantages to be gained, such as improved efficacy and reduced side effects,” said Worth Longest, Ph.D., the Louis S. and Ruth S. Harris Exceptional Scholar Professor in the Department of Mechanical and Nuclear Engineering in the VCU College of Engineering. Simply making the particles smaller isn’t a solution. “The problem with making the particles smaller is that they go in really well — but they also come straight back out during exhalation,” said Michael Hindle, Ph.D., the Peter R. Byron Distinguished Professor in the VCU School of Pharmacy. With three National Institutes of Health R01 grants totaling more than $7 million, Longest and Hindle are applying a combined engineering and pharmaceutical approach to make inhaled medications more effective and available. In “High-Efficiency Aerosol Delivery Using the Excipient Enhanced Growth Concept: A Human Proof of Concept Study,” Longest and Hindle have created a novel platform that produces particles that are tiny when they enter the lungs — but grow in size as they travel down the warm, humid airways. This platform comprises a device that uses a mixer-heater to produce tiny particles, about one-fifth the size of those from conventional inhalers. With this delivery concept, a pharmaceutical powder or liquid is enhanced with a hygroscopic excipient, essentially a substance that attracts water. “Your lungs are full of water,” Hindle said. “So if you put something inside your lungs that likes water, it’s going to swell and grow in size and not be expelled.” Using sodium chloride — salt — as the hygroscopic excipient, they have tested their system in vitro. The results have been promising. “We’ve flipped the needle,” Longest said. “Previously, only 10 percent of the initial dose would reach the lung, and that 10 percent was poorly targeted within different lung regions. With our approach, you can get 90 percent in and distribute that 90 percent evenly, or target a specific lung region.” The researchers will begin testing their method on adults in two human proof-of-concept trials beginning in late 2019 and early 2020. In two separate, but related, NIH studies, Longest and Hindle are adapting this concept for patients ranging in age from newborn to six. Each project proposes a device approximately the size of a lipstick tube that contains a pediatric formulation (liquid or powder) enhanced with a hygroscopic excipient. There are currently no inhalers on the market specifically designed for children or infants, even though their inhaling patterns and volumes differ from those of adults. Pediatric patients therefore must use adult-sized devices. One study focuses on targeted lung delivery of the antibiotic tobramycin to children with cystic fibrosis, a population prone to respiratory infection because of overproduction of mucus in the lungs. Pediatric cystic fibrosis patients with lung infections usually receive the medication via, 20-minute nebulizer treatments daily, sometimes up to four per day. Longest and Hindle’s proposed alternative is a pediatric dry powder inhaler that is fast and easy to use. Because its particles are engineered to reach the deep lung, it is expected to eradicate infection more efficiently because there is less risk of resistant strains of bacteria forming in undertreated regions of the lung. The other study focuses on delivery of surfactant aerosols to premature infants. Surfactant is a substance found in healthy lungs that keeps the tissue supple enough to expand and contract properly. The respiratory system is among the last to develop in utero, so in newborns and preemies, this substance is sometimes not fully developed — or not present at all. When these infants experience severe respiratory distress, the current protocol is to intubate and administer large doses of liquid surfactant to the lung by way of the throat. This highly invasive and potentially dangerous procedure causes distress and blood pressure fluctuations. In this third NIH-funded study, the researchers are also developing a tiny, small volume nebulizer and a dry powder inhaler for efficient, noninvasive respiratory support for infants.

August is National Breastfeeding Month – Let our Experts Help with Your Coverage
It’s August…a month that celebrates breastfeeding and all the benefits that come with it. Breastfeeding is natural, healthy and cost-effective – and the American public is beginning to recognize a mother’s right to feed her child wherever and whenever she wants. Breastfeeding is a great benefit to the environment and society, according to the American Academy of Pediatrics. Breastfeeding families are sick less often and the parents miss less work. It does not require the use of energy for manufacturing or create waste or air pollution. There is no risk of contamination and it is always at the right temperature and ready to feed. A new website developed by researchers in Canada and Asia showed that the world could have saved $341 billion each year if mothers breastfeed their children for longer, helping prevent early deaths and various diseases, according to a July 12 article from Reuters. Known as the “Cost of Not Breastfeeding,” the online tool used data from a six-year study supported by the U.S.-based maternal and child nutrition initiative, Alive & Thrive. According to Augusta University Health’s Dr. Kathryn Strickler McLeod, breastfeeding protects against a variety of diseases and conditions in the infant, including diarrhea, respiratory tract infection, childhood obesity and much more. Additionally, there are also maternal health benefits to breastfeeding, including a decreased risk of breast and ovarian cancers. If you are covering this topic – let us help with your stories and questions. Dr. Kathryn Strickler McLeod is a nationally recognized expert in pediatric general and adolescent medicine. McLeod is available to speak with media – simply click on the icon to arrange an interview.

‘The surprise, and the up side, is that episodic memories from before the children’s treatment were spared,’ Baylor researcher says Children with certain types of brain tumors who undergo radiation treatment are less likely to recall the specifics of events they experienced after radiation than to remember pre-treatment happenings, according to a Baylor University study comparing them to children with healthy brains. The finding is significant because children after treatment had less volume in the hippocampus — a part of the brain that plays an important role in memory. But while such a decrease usually is associated Alzheimer’s disease, dementia, brain injury, epileptic amnesia, encephalitis and aging, with those conditions both remote and recent memories are impaired, said lead author Melanie Sekeres, Ph.D., director of Sekeres Memory Laboratory at Baylor University. “The surprise, and the up side, is that episodic memories from before the children’s treatment were spared,” Sekeres said. For the study, published in The Journal of Neuroscience, researchers focused on “autobiographical memory,” which is linked to unique personal events and involves the recollection of emotional and perceptual details that allow a person to mentally re-experience the event, said Sekeres, assistant professor of psychology and neuroscience in Baylor’s College of Arts & Sciences. Radiotherapy and chemotherapy are used to treat the most common malignant brain tumor in children — a medulloblastoma. The reduced volume of the hippocampus is likely associated with radiation’s impact on the development of new cells in the nervous system, including the growth of new neurons in the hippocampus, or neurogenesis. “We know that these new cells play crucial roles in regulating memory and spatial learning, which is required to navigate. These treatments limit the brain’s ability to produce these new cells, which, in turn, limits the ability to form new memories,” Sekeres said. Research participants were 13 child survivors of brain tumors who had previously received radiotherapy and chemotherapy treatment at least one year before the study. Twenty-eight healthy youths of similar ages (ranging from 7 to 18) also were recruited for the study, conducted with The Hospital for Sick Children in Toronto, Ontario, Canada. All the youths completed the Children’s Autobiographical Interview — a standardized memory test — and underwent magnetic resonance imaging (MRI) of the brain. In individual interviews, children in both groups also were asked to recall memories from personal events that occurred at a specific time and place. Children were asked to recall a very old memory from an event before their radiation treatment (or an equally old memory for the healthy children) and a recent memory from within the past month. They were offered a list of events such as a birthday party, family trip, graduation and getting a pet but were told that they could choose another happening. The interview allowed children to freely recall without prompting before being asked general and specific questions about the event. “They have a hard time forming new, detailed memories,” Sekeres said. For example, when talking about a recent birthday party for a friend, they might tell how they met the friend and what that individual likes to do, but few specifics such as what they wore, the type of cake, what friends were there and what activities they did at the party, she said. “Such specific details might seem trivial, but these are precisely the kinds of details that allow us to vividly replay important events in our lives,” Sekeres said. “For most events, though, even healthy people forget a lot of specific details over time because we typically don’t need to retain all that incidental information. Some forgetting is normal and adaptive, and what we remember is the gist of an older event.” The patients were just as capable as healthy children of recalling these older memories, she said. But for children with brain tumors who have undergone radiation, the study suggested “deficits in their ability to either encode and/or retrieve highly detailed memories for personal events,” Sekeres said. “And those are the kind of memories that allow us to understand who we are and give us rich personal lives. “The study identifies an area of cognition that is inadvertently impacted by standard treatment, which has real consequences for the quality of life of the survivors. The physicians’ ultimate goal is to allow their patients to survive and to live as well as possible,” Sekeres said. “Although these treatments are often crucial in the effective management of the cancer, if the physicians and the family know there are these unintended side effects, that may be an additional factor to consider when exploring the treatment options.” ABOUT THE STUDY The study — “Impaired recent, but preserved remote, autobiographical memory in pediatric brain tumor patients” — was conducted with the Brain Tumor Program and the Program in Neurosciences and Mental Health at The Hospital for Sick Children in Toronto, Ontario, Canada. Funding was provided through the Canadian Institutes of Health Research. ABOUT BAYLOR UNIVERSITY Baylor University is a private Christian University and a nationally ranked research institution. The University provides a vibrant campus community for more than 17,000 students by blending interdisciplinary research with an international reputation for educational excellence and a faculty commitment to teaching and scholarship. Chartered in 1845 by the Republic of Texas through the efforts of Baptist pioneers, Baylor is the oldest continually operating University in Texas. Located in Waco, Baylor welcomes students from all 50 states and more than 80 countries to study a broad range of degrees among its 12 nationally recognized academic divisions. ABOUT BAYLOR COLLEGE OF ARTS & SCIENCES The College of Arts & Sciences is Baylor University’s oldest and largest academic division, consisting of 25 academic departments and seven academic centers and institutes. The more than 5,000 courses taught in the College span topics from art and theatre to religion, philosophy, sociology and the natural sciences. Faculty conduct research around the world, and research on the undergraduate and graduate level is prevalent throughout all disciplines. Visit College of Arts & Sciences.







