Experts Matter. Find Yours.
Connect for media, speaking, professional opportunities & more.
Survival analysis: Forecasting lifespans of patients and products
How long will you live? Should you spring for that AppleCare+ warranty for your iPhone? When will your buddy pay you back for that lunch? For centuries, soothsayers have striven to understand the lifespan of things – be they patient longevity, product lifecycles, or even time to loan default. Nowadays, scientists have turned away from reading tea leaves and toward survival analysis – a complex data science method for predicting not only whether an event will happen (the death of a patient, the failure of a product or machine, default on a payment, and so on) but when this event is likely to occur. But it’s problematic. Until now, the tools of survival analysis have only been applicable in certain settings. This is due to the inherent heterogeneity of what is being analyzed: differences in patient lifestyles, demographics, product usage patterns, and so on. New research by Goizueta Business School’s Donald Lee, associate professor of information systems and operations management and of biostatistics and bioinformatics, has yielded a new tool that greatly extends survival analysis to broader use cases. “Historically, scientists have used classic survival analysis tools to predict the lifespan of different things in different fields, from products to patients,” Lee said. “Since the 1950s, the Kaplan-Meier estimator has been the benchmark for analyzing lifetime data, particularly in clinical trials. The next breakthrough came in the 1970s when the Cox proportional hazards model was introduced, which allows researchers to incorporate variables that can affect the predictability of things like patient mortality.” The problem with the existing survival analysis tools, Lee said, is that they make certain assumptions that can skew the predictions if the assumptions are not met. “There are very few existing tools that can incorporate variables without imposing assumptions on how they affect survival, let alone when there are a lot of variables that can also change over time. For example, two iPhones will have different lifespans depending on the temperature at which they are stored, amongst many other factors. But it’s unlikely that storing your phone at 30 degrees will halve its lifespan compared to storing it at 60 degrees. This sort of linear relationship is commonly assumed by existing tools.” Lee’s team developed a new survival methodology based on something called gradient boosting: a machine learning technique that combines decision trees to yield predictions. The method, Lee said, is totally assumption-free (or nonparametric in technical parlance) and can deal with a large number of variables that can change continuously over time, making it significantly more general than existing methods. Nothing like it has been seen until now, he noted. “Calculating the survival rate of anything is super complex because of the variables. Say you want to create an app for a smart watch that monitors the wearer’s vitals and use this information to create a real-time warning indicator for stroke. Doing this accurately is difficult for two reasons,” Lee explained. “First, a large number of variables may be relevant to stroke risk, and the variables can interact in ways that break the assumptions central to existing survival analysis methods. And second, variables like blood pressure vary over time, and it is the recent measurements that are most informative. This introduces an additional time dimension that further complicates things.” The software implementation of Lee’s method, BoXHED, overcomes both issues and allows scientists to develop real-time predictive models for conditions like stroke. The trained model can then be ported to a watch app to tell its wearer if and when they’re likely to have a stroke, a process known as inferencing in machine learning lingo. The implications, Lee said, are huge. “BoXHED now opens the door for modern applications of survival analysis. In previous research, I have looked at the design of early warning mortality indicators for patients with advanced cancer and also for patients in the ICU. These use other methods to make predictions at fixed points in time, but now they can be transformed into real-time warning indicators using BoXHED.” He cited the case of end-stage cancer patients who are often better served by hospice care than by aggressive therapy. “Accurate predictions of survival are absolutely critical for care planning. In previous analyses, we have seen that using existing predictive models to inform end-of-life care planning can potentially avert $1.9 million in medical costs and 1,600 days of unnecessary inpatient care per 1,000 patient visits in the United States. BoXHED is likely to lead to even better results.” Lee’s research paper is forthcoming in the Annals of Statistics. He has also created an open-source software implementation of BoXHED, which can radically improve the accuracy of survival analysis across a breadth of applications. The paper describing BoXHED was published in the International Conference on Machine Learning, and the latest version of the BoXHED software can be found online. If you are a journalist or looking to speak with Donald Lee – simply click on his icon now to arrange an interview or appointment today.

Is hospital advertising actually good for our health?
Hospitals and healthcare organizations in the U.S. spend $1.5 billion on advertising every year. It’s a topic that provokes lively debate and a certain amount of controversy. Medical bodies, policy makers, and scholars alike question the ethics and efficacy of using (constrained) budgets to promote hospitals to patients. Diwas KC, professor of information systems & operations management at Emory University’s Goizueta Business School, and Tongil Kim, an assistant professor of management at Naveen Jindal School of Management in Texas, conducted a large-scale study of hospitals and patients in the state of Massachusetts to better understand the impact of hospital advertising. What they found is striking: Not only does television advertising work, it significantly drives demand, attracting patients living far from the hospital and beyond its regular area. And that’s not all. KC and Kim discovered that limiting hospital advertising or imposing an outright ban, as some groups have called for, might actually have serious negative effects on patient healthcare. “There has been a lot of discussion about banning advertising over recent years because of uncertainties around wasting money and resources,” KC said. In the paper “Impact of hospital advertising on patient demand and outcomes,” KC shows that there is a correlation between the amount spent on TV advertising and the quality of the hospital in question. Healthcare facilities that invest more in advertising tend to be “better” hospitals, he adds; they offer higher caliber care and services and, as such, they see much lower patient readmission rates—a key quality metric in healthcare. To get to these insights, KC and Kim looked at more than 220,000 individual patient visits to hospitals in the state of Massachusetts over a 24-month period. Among the data they collected were things like hospital type, location, and dollars spent on advertising. Patients were documented in terms of medical conditions, insurance, zip codes (to determine residence), and median household income. They were able to contrast those hospitals that invested in television advertising and those that did not. With the former, they uncovered a significant uptick in patient visits, with people coming from far further afield. This was particularly true of wealthier patients. Then there’s the question of patient outcomes. Here the data showed unequivocally that it’s the high-quality, low-readmission hospitals that advertise more—something that KC attributes to the natural tendency to get “more bang for the advertising buck when the quality of your product or service is better.” As for banning advertising, this would negatively impact these hospitals, he argues, limiting their ability to attract patients. It could also lead to an increase in population-level readmission rates. “Patient readmission rates are one of the key metrics along with mortality rates that tell us how well a healthcare facility is working,” said KC. “If a patient gets discharged but has to come back to a hospital in, say, 30 days, unless it’s a chronic condition or ongoing treatment, it’s a good indication that the patient didn’t get the level of care they should have the first time.” Indeed, “when we looked at all of the data, we found that the hospitals where there were fewest revisit rates were those that advertised more,” he said. KC finds that a blanket ban on hospital advertising could lead to an extra 1.2 readmissions for every 100 patients discharged. It’s a significant and “surprising” finding. And one that should inform the debate around healthcare advertising spend in the U.S. “There’s also the idea that this is a zero-sum game because if a patient doesn’t go to hospital A, they’re just going to go to hospital B—the one that advertises more—splitting the pie in different ways but not increasing that pie,” KC said. “What our study finds is that yes, advertising does draw patients away from one facility and towards another, but that the latter generally delivers better patient outcomes,” he said. “So, there is a social welfare benefit right there that suggests that you should not ban hospital advertising. There are real health benefits in allowing [advertising] to happen.” If you are a journalist looking to cover this topic - then let our experts help. Diwas KC is a Professor of Information Systems & Operations Management at Emory University’s Goizueta Business School. He is an expert in the areas of Data Analytics, Operations, and Healthcare. If you are interesting in arranging an interview - simply click on his icon to set up a time today.

Resilience in the Face of COVID-19
Brunswick Senior Advisor Paddy McGuinness, former UK Deputy National Security Adviser, on how businesses can chart a course amid the fear and uncertainty. We are all becoming more familiar with this disease than we care to be—and may become yet more so. Still uncertainty remains. It began even with the terminology. Coronavirus is a descriptor, a general term. Under the microscope, the virus has crown-like spikes, hence corona. The common cold and variances of it are coronaviruses. COVID-19 (as in Corona Virus Disease 2019) is the effect that this particular coronavirus has on the human being—that’s the disease the world’s grappling with. That’s the distinction between the two terms. We’ve now spoken to more than 150 clients about their situation. That has given us a broad view of the corporate response across affected geographies from Asia, through the Middle East and Europe to the Americas, a window into how those responses have played out and the challenges continually unfolding. Here’s what we’ve been advising our clients: First, develop a single view that’s grounded in professional, well-sourced information. In government we called this “a commonly recognized information picture.” That view has to be based on the responsible medical experts: the World Health Organization, the Center for Disease Control, Public Health England and similar bodies. You do not get it from the newspapers, from social media, from friends, or even your local medic. You operate on the basis of informed medical and public health advice. The current vocal challenge to that advice in Europe and the US is not reason to depart from it as your foundation for the actions you take. A leadership team needs to develop the discipline to clarify that generic narrative into a specific frame for their business context and then operate within it. It’s dangerous for leaders to start pretending they’re epidemiologists. Have a single view and stick to it. I’ve been on calls with leadership teams where there’s agreement on that view and then someone says, “But I read that the disease ...” Don’t go there. Don’t work on that basis. The uncertainty is difficult enough to deal with. Don’t add to it. You will be focused first on the safety—the human consequences—of your course of action and then on the resilience of your business. That may cause you to anticipate some of the “Non Pharmaceutical Interventions” that government makes. Brunswick has. Having established your position, think through how you’re going to communicate it to employees, customers, and investors. What about your suppliers and regulators? How might you engage with local public health officials and local authorities? Exaggeration and understatement are equally unhelpful. These engagements need to be tailored, yet aligned within your broader narrative. Leaders also need to plan for reasonable worst-case scenarios. Covid-19 has already spread in a way that we hoped wouldn’t happen, and in a way that standard business continuity planning doesn’t cover. Now, many in the workforce have to work from home. Among other considerations, that produces additional cyber and data vulnerability. What if schools close and your employees have children at home they have to look after? What will your IT capabilities be if 20 to 40 percent of your team is incapacitated at any one time during the peak period? Are your HR teams prepared to deal with the most unfortunate case, where employees or their close relatives pass away? In extreme times, it can be tempting to take extreme positions. A lesson of crises is never to enter into something without knowing how you’re going to get out of it, how to reverse it. If companies are going to start shutting down their operations, how are they going to open again? On what justification? Taking fixed positions amid great uncertainty can prove restrictive—or counterproductive—when circumstances change. Resilience is the ability to respond and recover to the state prior to the event, having learned the lessons of the event. Respond and recover—that’s the long-term goal here. Covid-19 will pass. We know from other pandemics that recovery does come. How can you position yourself to take advantage of that recovery, to get back with speed and strength? Because some companies will. Now more than ever senior leaders need to talk about how things will be the other side of the crisis and to describe signs of recovery. This is easiest for enterprises with transnational reach. They recount what is happening in Asia as the disease passes so that European and US stakeholders can see beyond the immediate demands of emergency response. On a personal level, stick close to the medical experts and the people who know what they’re talking about. I may well get Covid-19 here in the United Kingdom. I assume that, like the vast majority of healthy people who get it, I will experience mild to moderate symptoms and recover just fine. If I don’t, I want health services to be available. I want the spread to be managed at sustainable levels, so I am doing what Government asks of me and avoiding all but essential contact with others and unnecessary travel. I expect that more will be asked of me, my family and colleagues before we are through this. I wouldn’t let Covid-19 overwhelm you in your daily life, given what we know. That’s certainly my intention: carry on with as much normality as possible, support others and use the unexpected circumstances to prepare for the recovery phase which will come.

Criminals are opportunists, and the COVID-19 global onslaught has brought with it not just health threats but cybersecurity risks, too. Within weeks of the COVID-19 outbreak, hackers have already commandeered the virus to unleash cyberattacks, sending emails purporting to provide coronavirus guidance laced with cyberattack software. In one more alarming case, they appear to have attacked a hospital and forced it to cancel operations and take key systems offline. As the outbreak continues to intensify, the UK National Cyber Security Centre (NCSC) warned that the volume of these attacks will likely increase, pointing to the increased registration of coronavirus-related webpages. Criminals are opportunists, and the COVID-19 global onslaught has brought with it not just health threats but cybersecurity risks, too. As companies move to protect the health of their workforce, it’s also important to protect the systems they’re using to run their businesses. It’s especially important for hospitals to shore-up their cyber defenses. If they don’t, just as they are racing to respond to COVID-19, they could face situations like University Hospital Brno in the Czech Republic, which earlier this month was forced to divert patients and cancel planned operations while it worked to address an attack. The most likely cyber threats are email “phishing” campaigns that use the coronavirus as a lure to get the recipient to open an attachment that contains malware. According to the NCSC, such “phishing” attempts are happening on a global scale in multiple countries, which has led to both a theft of money and sensitive data. Similarly, known hacker groups have been launching websites purporting to sell masks or other safety-related measures for coronavirus, possibly to use them as another vector for cyberattacks. The NCSC has also cautioned that these attacks are “versatile and can be conducted through various media, adapted to different sectors and monetized via multiple means, including ransomware, credential theft, bitcoin or fraud.” The cybersecurity firm ProofPoint has seen a rise in these cyberattack emails with COVID-19 themes since January. Both ProofPoint and IBM’s X-Force cybersecurity unit identified a campaign that targeted users in Japan with an email masquerading as a coronavirus information email that carries with it a potent type of cybercrime software. In the US, the Secret Service recently warned of scams from online criminals posing as sellers of high-demand medical supplies to prevent coronavirus. They’ll require payment upfront and not send the products. Cyber criminals have also been posing as the World Health Organization and the US Centers for Disease Control and Prevention (CDC), sending fraudulent emails from the former and “creating domain names similar to the CDC’s web address to request passwords and even bitcoin donations to fund a vaccine” for the latter. In addition to the use of the coronavirus as a cyberattack vector, the growing need for working remotely to mitigate the spread of COVID-19 has increased companies’ exposure to cyber threats. The increase in remote work creates more opportunities for hackers to make inroads from less secure locations. Companies should also ensure they can provide adequate security when their whole workforce is remote. They should quickly work through the security implications of workers choosing to switch to insecure personal devices. With national-level pressures on home broadband, staff will also resort to mobile hotspots, which are often less secure. And enabling remote connectivity at scale, with the right security configurations, can be a challenge even with months of preparation time. A recent US Department of Homeland Security COVID-19 cybersecurity notice pointed to the importance of making sure that security measures are up to date for companies’ remote access systems. Additional measures to consider include enabling multifactor authentication—which can require two or more steps to verify a user’s identity before granting access to corporate networks. The NCSC is also working to identify malicious sites responsible for phishing and cyberattack software. A final looming cyberthreat related to Covid-19 is disinformation. The World Health Organization and other agencies have for months been combatting disinformation campaigns spreading false information about the origins of and treatments for COVID-19—reports that seed more confusion and increase risks to society. All of that means that computer virus risks are emerging as the biological virus spreads—and both are a threat to business. Cyber risk mitigation efforts should account for the different ways that a company can be affected, including impacts on the technical, operational, legal and reputational aspects of a business. Often, the reputational effects of a cyberattack are more significant than direct the business or technical impact. To mitigate all of the potential impacts of cyberattacks taking advantage of the Covid-19 outbreak, companies should: Review and update crisis and cybersecurity response plans, and ensure internal and external communications response plans are robust. Confirm that members of the crisis management team understand their roles and responsibilities. Make sure all communications channels have the latest security patches. Review and update access controls, particularly when remote access is used heavily, to make sure that only those who require access to sensitive systems to do their jobs have it. Take extra care when handling medical information. For companies managing employees who have contracted Covid-19, it’s important that personal health information is handled with strong security measures, including encryption. Educate employees about the cyber risks that may attempt to capitalize on fear of the Covid-19 virus—whether it be phishing email or disinformation. Covid-19 poses a number of short- and long-term challenges to business resilience, and the virus’s trajectory is quick and unpredictable. But it’s possible to anticipate and mitigate a number of the cyber threats that will try to ride the virus’s coattails. The companies that do will be more resilient and better positioned to withstand the direct health and operational effects of the virus.

As battle-weary Americans struggle to emerge from the anxiety and worry of COVID-19, there might be even more bad news around the corner this fall for parents of young children. The U.S. Centers for Disease Control and Prevention (CDC) is sounding the alarm now about increased cases of acute flaccid myelitis (AFM) in the coming fall. It is of a rare but serious polio-like condition that surfaces every two years and children under five are its main target. On average, patients during the last outbreak in 2018 were aged 5 years old. Limb weakness and paralysis is the most common symptom of the condition which affects the nerve cells in the gray matter of the spinal cord. Others include a fever, pain, or numbness in one or more limbs, problems walking normally, a headache, back or neck pain, issues with swallowing or talking, and weakness in the face or neck. Patients may also have had a recent or current respiratory illness. August 05 - Newsweek In what has already been a harrowing year, it looks like there may be another serious health concern on the horizon. And if you are an expert covering children’s health the potential for acute flaccid myelitis to peak in 2020 – then let our experts help. Dr. Elizabeth Sekul is a highly acclaimed pediatric neurologist specializing in electrodiagnostic medicine and neuromuscular diseases. She also works as an associate professor at the Medical College of Georgia's Department of Neurology and the Department of Pediatrics and Child Neurology. If you are a journalist looking to book an interview – simply click on Dr. Sekul’s icon and arrange a time today.

VCU Engineering researchers are working to make clean energy easier and cheaper
Lane Carasik, Ph.D., assistant professor in VCU’s Department of Mechanical and Nuclear Engineering, is developing methods to make clean energy more cost-effective. He’s motivated by a simple principle. “The cheaper we make renewable and clean energy, the easier it is to implement it,” he said. With $100,000 in seed funding from the Jeffress Trust Awards Program, Carasik and his Fluids in Advanced Systems and Technology (FAST) research group are designing efficient, low-cost enhancements to equipment used in solar, nuclear and geothermal energy systems. Jeffress Trust awards support high-impact, one-year projects that integrate computational and quantitative scientific methodologies across a broad range of scientific disciplines. These energy systems use heat exchangers, which take energy from heat generation components and convert it to electricity. Heat exchangers usually comprise two working substances such as water, steam or air separated by tubes or plates. The FAST research group is optimizing a specialty insert that can be placed inside a heat exchanger’s tubes to improve performance. To visualize the insert’s form, imagine holding a piece of metal tape in both hands and gently twisting it. See the FAST Lab and examples of the heat transfer enhancements being designed there. “A liquid running through a tube is relatively undisrupted by the geometry of the tube or the shape of the fluid,” Carasik said. “But this twisted tape component spins the fluid. This increases turbulence, which increases heat transfer.” While “twisted tape” inserts are already in use in some advanced energy systems, the process of fabricating them has been limited by mechanical constraints. Typically, the inserts are placed inside a tube and tack welded at either end. But because of the metal’s limited tensile strength, these inserts can only be twisted a little before they break down and cause manufacturing defects. 3D printing, on the other hand, allows for a more complex — and effective — insert that can be used to characterize heat transfer performance. “With additive manufacturing, you can actually print tighter, ‘twistier’ versions of them,” Carasik said. “You can also add your own intentional defects to find out how to make the heat transfer better and improve the performance of the whole system.” Each geometric form the research group prints and tests starts with a world of calculations: thermal-hydraulics design calculations, solid geometry, material properties and more. From there, components are computer-designed, then printed in the Mechanical and Nuclear Engineering Innovation Lab. Finally, they are tested in the FAST research group’s Modular Separation Effects Testing Facility (MSEFT), a scaled testing loop that emulates the operating conditions experienced by these components. Undergraduates — even first-year students — participate in each step of the process, alongside Carasik, postdoctoral research associate Cody Wiggins, Ph.D., and doctoral student Arturo Cabral. “I really like getting students into research early on, Carasik said. “By the time they’re three years in, they’re working at a level I would expect from bachelor’s level engineers in industry.” Senior Meryem Murphy was curious about undergraduate research but had never really participated. “One day, I was arguing with Arturo about something and Dr. Carasik said, ‘If you’re like this all the time, you should work for the lab.’” She took him up on it and spent her junior year working on an MSEFT redesign and running an experiment to see if 3D-prototyped concepts can be replicated with test metals. Over the summer, Murphy interned with Atomic Alchemy, a medical radioisotope startup in Boise, Idaho. She said the position built on the hard, and soft, skills she gained in the lab. “Sometimes in class, you’re required to collaborate,” she said. “But in research, it’s just ‘what you do’ to get it done.” Rising sophomore Ryan McGuire is also looking forward to starting his second year in the lab. During his freshman year, McGuire helped develop a 3D printing technology to duplicate sequences of 3D-printed parts for the FAST research group. It’s called Retrospective Additive Manufacturing Sequencing — RAMS for short. McGuire said the thrill of solving problems in the lab has made him reassess his own goals. “When I was younger, I wanted to be [famous],” he said. “But now I no longer want to be famous. Research seems like more fun.” Upon hearing about McGuire’s change in priorities, Carasik said, “Researchers can be famous too, and for good reason.”

Chatbots can ease medical providers' burden, offer trusted guidance to those with COVID-19 symptoms
COVID-19 has placed tremendous pressure on health care systems, not only for critical care but also from an anxious public looking for answers. Research from the Indiana University Kelley School of Business found that chatbots -- software applications that conduct online chats via text or text-to-speech -- working for reputable organizations can ease the burden on medical providers and offer trusted guidance to those with symptoms. Researchers conducted an online experiment with 371 participants who viewed a COVID-19 screening session between a hotline agent -- chatbot or human -- and a user with mild or severe symptoms. They studied whether chatbots were seen as being persuasive, providing satisfying information that likely would be followed. Their results showed a slight negative bias against chatbots' ability, perhaps due to recent press reports. When the perceived ability is the same, however, participants reported that they viewed chatbots more positively than human agents, which is good news for health care organizations struggling to meet user demand for screening services. "The primary factor driving user response to screening hotlines -- human or chatbot -- is perceptions of the agent's ability," said Alan Dennis, the John T. Chambers Chair of Internet Systems at Kelley and corresponding author of the paper, "User reactions to COVID-19 screening chatbots from reputable providers." "When ability is the same, users view chatbots no differently or more positively than human agents." Other authors on the paper, forthcoming in the Journal of the American Medical Informatics Association, are Antino Kim, assistant professor of operations and decision technologies at Kelley; and Sezgin Ayabakan, assistant professor of management information systems, and doctoral candidate Mohammad Rahimi, both at Temple University's Fox School of Business. Even before the pandemic, chatbots were identified as a technology that could speed up how people interact with researchers and find medical information online. "Chatbots are scalable, so they can meet an unexpected surge in demand when there is a shortage of qualified human agents," Dennis, Kim and their co-authors wrote, adding that chatbots "can provide round-the-clock service at a low operational cost. "This positive response may be because users feel more comfortable disclosing information to a chatbot, especially socially undesirable information, because a chatbot makes no judgment," researchers wrote. "The CDC, the World Health Organization, UNICEF and other health organizations caution that the COVID-19 outbreak has provoked social stigma and discriminatory behaviors against people of certain ethnic backgrounds, as well as those perceived to have been in contact with the virus. This is truly an unfortunate situation, and perhaps chatbots can assist those who are hesitant to seek help because of the stigma." The primary factor driving perceptions of ability was the user's trust in the provider of the screening hotline. "Proactively informing users of the chatbot's ability is important," the authors wrote. "Users need to understand that chatbots use the same up-to-date knowledge base and follow the same set of screening protocols as human agents. ... Because trust in the provider strongly influences perceptions of ability, building on the organization's reputation may also prove useful."

Overshadowed by COVID – The opioid pandemic is still taking its toll across America
For more than two decades opioids have been ravaging American cities, towns, and communities. It prompted national attentions and official commissions advising the President. But lately, as the world has turned almost all its focus on COVID-19, the opioid issue has been sitting in the shadows. Not necessarily idle or waiting, but just no longer the topic of a national conversation to find a cure. Before COVID-19 turned our nation upside-down, policymakers were taking steps to help patients access evidence-based treatment for opioid use disorder. This included focusing on removing health insurers’ barriers to medication and requiring insurers to provide parity for mental illness and substance use disorders — and holding them accountable for violations of the law in Massachusetts, Pennsylvania and New Hampshire, to name a few recent examples. While we continue to take steps to address COVID-19 to help keep the public safe, the American Medical Association has seen reports from more than 30 states concerning increases in opioid-related mortality, mental health crises, suicide and addiction-related relapse. Reports are from every region in the nation. This includes a 20 percent increase in calls to the Jacksonville, Fla., fire department concerning overdoses; an “unusual spike” in overdoses in DuPage County, Ill.; increased emergency department visits in coastal North Carolina and spikes in fentanyl-related overdoses in Seattle. Georgia, too, has not been spared, causing increased concern for many. - Dr. Patrice A. Harris is the immediate past president of the American Medical Association and chair of the AMA Opioid Task Force. So – at what cost or how far back have efforts been set by COVID-19? And how much harder will it be for America to regroup and take on its addiction to opioids? There are a lot of questions to be asked – and if you are a journalist covering this topic or looking to learn more about the state of the opioid epidemic in America – then let our experts help. Justin Cole is an expert in clinical pharmacy, Pharmacogenomics, and the pharmacy industry. Justin has been following this issue closely and is available to speak with media. Simply click on his icon to arrange an interview today.
Virtual Reality-Based Surgical Simulations Could Make Patients Safer
Suvranu De, the director of the Center for Modeling, Simulation, and Imaging in Medicine at Rensselaer, has dedicated more than a decade of research to making surgery safer by developing virtual reality-based surgical training simulations that closely mimic the optics and haptics a surgeon may encounter in the operating room. A new $2.3 million grant from the National Institute of Biomedical Imaging and Bioengineering of the National Institutes of Health will further his research in this space, by supporting the development of a collaborative virtual reality-based surgical simulation environment that allows medical professionals to practice technical, cognitive, and interpersonal skills as a team. “People will be wearing head-mounted displays, and they will be immersed in a virtual operating room working on a virtual patient as a team,” De said. “We want to have an expert team in the operating room focused on the treatment of a patient, and not just a team of experts.” Conceptually, this approach is similar to crew resource management practiced by aviation pilots, which has led to a significant reduction in aircraft accidents. The Virtual Operating Room Team Experience (VORTeX) simulation system will provide realistic distractions, interruptions, and other stressors that medical professionals may encounter in an operating room. Traditionally, this type of simulation training has required mannequins, instructors, and a dedicated space, as well as significant coordination and resources. In contrast, the VORTeX system will be both distributed and asynchronous – allowing participants to join the simulation from different locations, and instructors to review the simulation and provide feedback at their convenience. Machine learning algorithms will be used to crunch the data and provide feedback to participants, who will be able to return to the virtual environment to review their performance. De is available to discuss how this type of virtual training is developed and implemented.
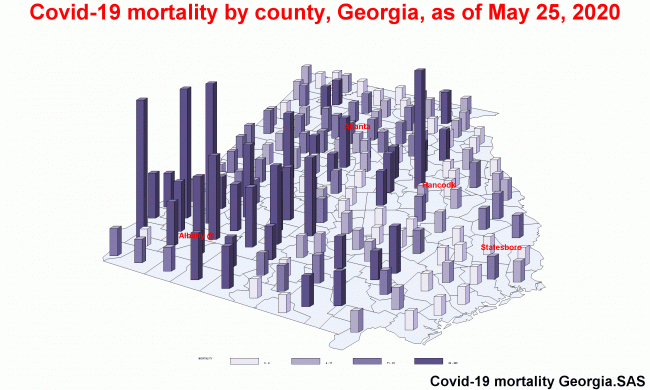
Graduate students in the Jiann-Ping Hsu College of Public Health at Georgia Southern University analyzed mortality data to reveal that a county in southwest Georgia is dealing with deaths from COVID-19 at a rate higher than most other counties in the country. The students found that the mortality rate of 305 per 100,000 residents (as of May 28, 2020) for Terrell County in southwestern Georgia, is 50% higher than that of New York state’s Nassau County, the documented highest rate in New York. The three other Georgia counties that are highest in terms of mortality rate are Hancock, Early and Dougherty counties. Three out of these four are in southwest Georgia, around the Albany area. That accounts for almost half of the 10 counties in the United States with the highest mortality rate, which is defined as a measure of the frequency of occurrence of death among a defined population. However, it’s interesting to note that none of Georgia counties reached the top 20 in terms of incidence and the death numbers per 100 confirmed Covid-19 cases, said professor Dr. Jian Zhang, a veteran medical epidemiologist. “Georgia is doing pretty well to stop the spread of the virus, and hospitals in Georgia are doing well to save hospitalized COVID-19 patients. The high mortality rate, in this case, may be deeply rooted in the historical burden of poverty in Georgia,” Zhang said. The findings are part of a service-learning project Zhang led. A six-student group formed the surveillance team that began running a real-time COVID-19 numbers in his Public Health Surveillance class. If you are a journalist covering COVID-19 and would like to learn more about this research taking place at Georgia Southern University – then let us help. Dr. Jian Zhang has worked with the Chinese Centers for Disease Control and Prevention, and the World Health Organization prior to moving to the United States.








